Non-cystic fibrosis bronchiectasis in pediatrics: A cohort profile of patients with inborn errors of immunity at a referral center in Cali, Colombia
Abstract
Introduction. Inborn errors of immunity are frequently associated with bronchiectasis. The diagnostic performance of these inborn errors has improved because the association of some of these entities with progressive airway damage is better known. This knowledge has allowed recognition and appropriate intervention reducing deterioration of the pulmonary function and improving quality of life.
Objective. To describe a group of patients with bronchiectasis not related to cystic fibrosis who were diagnosed with inborn errors of immunity and have been studied in an immunology reference center in Colombia.
Materials and methods. We conducted an observational, descriptive, and retrospective study with participating patients under 18 years, diagnosed with inborn errors of immunity and non-cystic fibrosis bronchiectasis, between December 2013 and December 2023 at the Fundación Valle del Lili in Cali, Colombia.
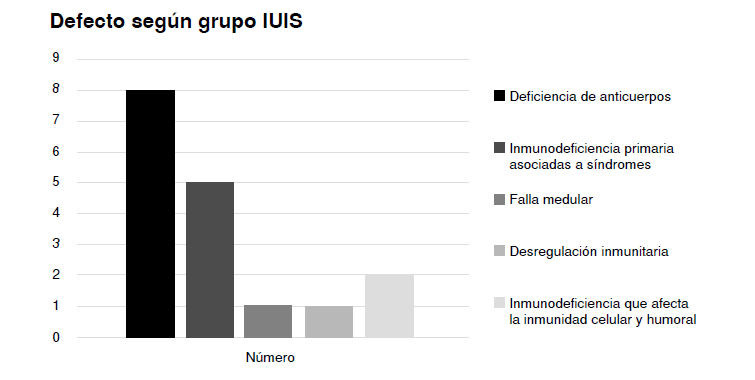
Results. Seventeen patients were diagnosed with non-cystic fibrosis bronchiectasis and inborn errors of immunity. Their mean age was nine years. The lower pulmonary lobe was the most frequently affected segment, and in most cases, unilaterally. The most prevalent alteration was predominantly antibody inmunodeficiency, followed by combined immunodeficiencies associated with syndromes. Thirteen patients had humoral immunity compromise, while 4 exhibited humoral and cellular immunity alterations. Additionally, 12 patients presented genetic mutations related to their phenotype. Thirteen patients, underwent supplementation with intravenous immunoglobulin, and 3 died.
Conclusion. The inborn errors of immunity most frequently associated with noncystic fibrosis bronchiectasis, were predominantly antibody deficiency and combined
immunodeficiencies with syndromic features.
Downloads
References
Chan ED, Wooten WI, Hsieh EWY, Johnston KL, Shaffer M, Sandhaus RA, et al. Diagnostic evaluation of bronchiectasis. Respir Med X. 2019;1. https://doi.org/10.1016/j.yrmex.2019.100006
Boyton RJ, Altmann DM. Bronchiectasis: Current concepts in pathogenesis, immunology, and microbiology. Annu Rev Pathol. 2016:11:523-54. https://doi.org/10.1146/annurev-pathol-012615-044344
Wall LA, Wisner EL, Gipson KS, Sorensen RU. Bronchiectasis in primary antibody deficiencies: A multidisciplinary approach. Front Immunol. 2020;11. https://doi.org/10.3389/fimmu.2020.00522
Tangye SG, Al-Herz W, Bousfiha A, Cunningham-Rundles C, Franco JL, Holland SM, et al. Human inborn errors of immunity: 2022 Update on the Classification from the International Union of Immunological Societies Expert Committee. J Clin Immunol. 2022;42:1473-507. https://doi.org/10.1007/s10875-022-01289-3
Poeta M, Maglione M, Borrelli M, Santamaría F. Non-cystic fibrosis bronchiectasis in children and adolescents: Neglected and emerging issues. Pediatr Neonatol. 2020;61:255-62. https://doi.org/10.1016/j.pedneo.2019.09.013
McShane PJ. Common variable immunodeficiency and other immunodeficiency syndromes in bronchiectasis. Semin Respir Crit Care Med. 2021;42:525-36. https://doi.org/10.1055/s-0041-1730893
Edwards EA, Asher MI, Byrnes CA. Paediatric bronchiectasis in the twenty-first century: Experience of a tertiary children’s hospital in New Zealand. J Paediatr Child Health. 2003;39:111-7. https://doi.org/10.1046/j.1440-1754.2003.00101.x
Gutiérrez MJ, Nino G, Sun D, Restrepo-Gualteros S, Sadreameli SC, Fiorino EK, et al. The lung in inborn errors of immunity: From clinical disease patterns to molecular pathogenesis. J Allergy Clin Immunol. 2022;150:1314-24. https://doi.org/10.1016/j.jaci.2022.08.024
McCusker C, Upton J, Warrington R. Primary immunodeficiency. Allergy Asthma Clin Immunol. 2018;14(Supl.2):61. https://doi.org/10.1186/s13223-018-0290-5
Mahlaoui N, Warnatz K, Jones A, Workman S, Cant A. Advances in the care of primary immunodeficiencies (PIDs): From birth to adulthood. J Clin Immunol. 2017;37:452-60. https://doi.org/10.1007/s10875-017-0401-y
Slade CA, Bosco JJ, Giang TB, Kruse E, Stirling RG, Cameron PU, et al. Delayed diagnosis and complications of predominantly antibody deficiencies in a cohort of Australian adults. Front Immunol. 2018;9:694. https://doi.org/10.3389/fimmu.2018.00694
Haidopoulou K, Calder A, Jones A, Jaffe A, Sonnappa S. Bronchiectasis secondary to primary immunodeficiency in children: Longitudinal changes in structure and function. Pediatr Pulmonol. 2009;44:669-75. https://doi.org/10.1002/ppul.21036
Reyes F, Müller G. Bronquiectasias no fibrosis quística. Desde la infancia a la adultez. Enfoque diagnóstico y terapéutico. Neumol Pediatr. 2019;14:86-91. https://doi.org/10.51451/np.v14i2.92
Cinetto F, Scarpa R, Rattazzi M, Agostini C. The broad spectrum of lung diseases in primary antibody deficiencies. Eur Respir Rev. 2018;27. https://doi.org/10.1183/16000617.0019-2018
Banjar HH. Clinical profile of Saudi children with bronchiectasis. Indian J Pediatr. 2007;74:149-52. https://doi.org/10.1007/s12098-007-0008-z
Pedraza Á, Vargas-Rumilla MI, Ramírez-Roa JL. Registry of primary immunodeficiencies in children at a fourth level hospital. Bogotá, 2010-2016. Rev Alerg Mex. 2018;65:341-8. https://doi.org/10.29262/ram.v65i4.338
European Society for Immunodeficiencies - ESID. Working Definitions for Clinical Diagnosis of PID. Fecha de consulta: 2 de febrero de 2024.
Zea-Vera AF, Chacón MA, Parra B. Antibody deficiencies with normal IgG in adults with noncystic fibrosis bronchiectasis or recurrent pneumonia: Cross-sectional study. Colomb Med. 2022;53. https://doi.org/10.25100/cm.v53i2.4832
Bush A, Floto RA. Pathophysiology, causes and genetics of paediatric and adult bronchiectasis. Respirology. 2019;24:1053-62 https://doi.org/10.1111/resp.13509
Huggard D, Doherty DG, Molloy EJ. Immune dysregulation in children with Down syndrome. Front Pediatr. 2020;8. https://doi.org/10.3389/fped.2020.00073
Brower KS, Del Vecchio MT, Aronoff SC. The etiologies of non-CF bronchiectasis in childhood: A systematic review of 989 subjects. BMC Pediatr. 2014;14. https://doi.org/10.1186/s12887-014-0299-y
Bekir M, Aydıner EK, Yıldızeli ŞO, Öğülür İ, Kocakaya D, Barış S, et al. Primary immun deficiency in patients with non-cystic fibrosis bronchiectasis and its relationship with clinical parameters. Turk Thorac J. 2021;22:37-44. https://doi.org/10.5152/TurkThoracJ.2020.19077
Baumann U, Routes JM, Soler-Palacín P, Jolles S. The lung in primary immunodeficiencies: New concepts in infection and inflammation. Front Immunol. 2018;9. https://doi.org/10.3389/fimmu.2018.01837
Sil A, Basu S, Joshi V, Pilania RK, Siniah S, Suri D, et al. Immunoglobulin replacement therapies in inborn errors of immunity: A review. Front Pediatr. 2024;12. https://doi.org/10.3389/fped.2024.1368755
Correa-Jiménez O, Restrepo-Gualteros S, Nino G, Cunningham-Rundles C, Sullivan KE, Fuleihan RL, et al. Respiratory comorbidities associated with bronchiectasis in patients with common variable immunodeficiency in the USIDNET registry. J Clin Immunol. 2023;43:2208-20. https://doi.org/10.1007/s10875-023-01593-6
Some similar items:
- Marcela González, Claudia Patricia González, Alvaro Sanabria, Ultrasonographic estimation of the normal volume of the thyroid gland in pediatric populations. , Biomedica: Vol. 26 No. 1 (2006)
- Wilson Daza, Silvana Dadan, Michelle Higuera, Profile of gastrointestinal diseases in a pediatric gastroenterology center in Colombia: 15 years of follow-up , Biomedica: Vol. 37 No. 3 (2017)
- Luisa F. Imbachi, Lina M. Ibañez , Paula Hurtado-Villa, Health status and barriers in health care for children with birth defects born between 2011 and 2017 in two institutions in Cali , Biomedica: Vol. 40 No. 1 (2020)
- Freddy Israel Pantoja, Willinton Robert Ricaurte , Diana Elizabeth Rosero , Relationship between death and admission of pediatric patients to intensive care due to Staphylococcus aureus bacteremia acquired in the community, 2014-2017 , Biomedica: Vol. 41 No. 1 (2021)
- Yesica Llimpe, Cytogenetic risk groups for childhood acute myeloid leukemia based on survival analysis in a cancer referral hospital from Perú , Biomedica: Vol. 41 No. 2 (2021)
- Jorge Andrés Puerto, Susana Uribe , Víctor Calvo, Ricardo Cardona, Impact of the allergen-specific immunotherapy in pediatric patients with asthma treated at a health institution in Colombia , Biomedica: Vol. 41 No. 3 (2021)
- Miguel Ángel Medina, Wendy Meyer , Carolina Echeverri , Natalia Builes , Langerhans cell histiocytosis: Case report and literature review , Biomedica: Vol. 41 No. 3 (2021)
- Luis Carlos Salazar, Luz Ángela Moreno , Lina Eugenia Jaramillo , Edgar Vladimir Cabrera , Erdheim-Chester disease: First pediatric case report in Colombia , Biomedica: Vol. 41 No. 4 (2021)
- Natalia Vélez-Tirado , Lina Castaño-Jaramillo , Sonia Restrepo-Gualteros , Catalina Alcalá-Lozano, Erika Ruge , Carolina Puente , Diana Li-Zeng , Diego Chaparro-Arce , María Camila Beltrán-Dimas , Juan Francisco López , Miguel Luengas-Monroy , Diego Galvis-Trujillo , Iván Gutiérrez-Tobar , Pablo Vásquez-Hoyos , Germán Camacho-Moreno , Severe adenovirus infection outbreak in Colombia: Experience from a tertiary pediatric hospital in 2022 , Biomedica: Vol. 44 No. 1 (2024)
- Rafael Adrián Pacheco-Orozco, Jessica María Forero-Delgadillo, Vanessa Ochoa, Juan Sebastián Toro, Harry Pachajoa, Jaime Manuel Restrepo, Genetic and radiological aspects of pediatric renal cystic disease: A case series , Biomedica: Vol. 44 No. Sp. 1 (2024): Enfermedades crónicas no transmisibles
Copyright (c) 2024 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |
Funding data

























