From phenotypic to molecular diagnosis: Insights from a clinical immunology service focused on inborn errors of immunity in Colombia
Abstract
Introduction. Inborn errors of immunity include a broad spectrum of genetic diseases, in which a specific gene mutation might alter the entire emphasis and approach for an individual patient.
Objective. To conduct a comprehensive analysis of the correlation between phenotypic and molecular diagnoses in patients with confirmed inborn errors of immunity at a tertiary hospital in Cali, Colombia.
Materials and methods. We conducted a retrospective study in which we sequentially evaluated all available institutional medical records with a diagnosis of inborn errors of immunity.
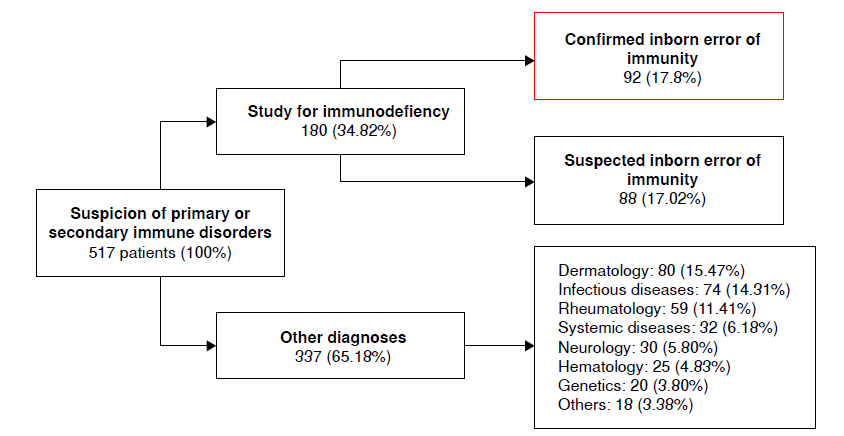
Results. In the Clinical Immunology Service of the Hospital Universitario del Valle, 517 patients were evaluated. According to the IUIS-2022 classification, 92 patients (17.35%) were definitively diagnosed with an inborn error of immunity. Of these, 38 patients underwent genetic studies. The most prevalent category was predominantly antibody deficiencies (group III) (38/92 - 41.3%). A broad spectrum of genetic defects, novel and previously reported, were described, including mutations in the following genes: ATM, BTK, ERBIN, MAB21L2, RAG2, SAVI, SH2D1A, STAT1, SYK, and TMEM173. Less frequent findings included cases of the WHIM syndrome, SYK gain-of-function, and IL-7 deficiency.
Conclusions. The establishment of the Clinical Immunology Service in the Hospital Universitario del Valle has emerged as a pivotal resource, catering to individuals with limited financial means and covered by public health insurance within the southwest region of Colombia. Molecular genetics confirmatory diagnosis was achieved in 38 patients (41.3%) with inborn errors of immunity and changed the diagnosis in 24 cases (26%).
Downloads
References
Boyle JM, Buckley RH. Population prevalence of diagnosed primary immunodeficiency diseases in the United States. J Clin Immunol. 2007;27:497-502. https://doi.org/10.1007/s10875-007-9103-1
Vásquez E, Villada F, Orrego JC, Franco JL. Espectro de las inmunodeficiencias primarias en Colombia: reporte del Centro Nacional de Referencia Jeffrey Modell para diagnóstico e investigación en inmunodeficiencias primarias (CJM-UDEA). Iatreia. 2013;26 (Supp. 3):S43.
Ochs HD, Hitzig WH. History of primary immunodeficiency diseases. Curr Opin Allergy Clin Immunol. 2012;12:577-87. https://doi.org/10.1097/ACI.0b013e32835923a6
Montoya CJ, Henao J, Salgado H. Diagnóstico fenotípico de las inmunodeficiencias primarias en Antioquia, Colombia, 1994-2002. Biomédica. 2002;22:510-8. https://doi.org/10.7705/biomedica.v22i4.1177
Pareja-Arcila ML. Situación actual de las enfermedades huérfanas en Colombia 2017. CES Derecho. 2017;8:231-41. https://doi.org/10.21615/cesder.8.2.2
Immune Deficiency Foundation. Primary Immunodeficiency Diseases in America: 2007: The Third National Survey of Patients. Hanover: Immune Deficiency Foundation; 2009.
Bousfiha A, Moundir A, Tangye SG, Picard C, Jeddane L, Al-Herz W, et al. The 2022 Update of IUIS Phenotypical Classification for Human Inborn Errors of Immunity. J Clin Immunol. 2022;42:1508-20. https://doi.org/10.1007/s10875-022-01352-z
Rojas-Restrepo J, Caballero-Oteyza A, Huebscher K, Haberstroh H, Fliegauf M, Keller B, et al. Establishing the molecular diagnoses in a cohort of 291 patients with predominantly antibody deficiency by targeted next-generation sequencing: Experience from a monocentric study. Front Immunol. 2021;12. https://doi.org/10.3389/fimmu.2021.786516
Moundir A, Ouair H, Benhsaien I, Jeddane L, Rada N, Amenzoui N, et al. Genetic diagnosis of inborn errors of immunity in an emerging country: A retrospective study of 216 Moroccan patients. J Clin Immunol. 2023;43:485-94. https://doi.org/10.1007/s10875-022-01398-z
Zea-Vera AF. Common variable immunodeficiency and chronic hepatitis B: Therapeutic challenge. Clin Res Hepatol Gastroenterol. 2020;44:e38-40. https://doi.org/10.1016/j.clinre.2019.07.002
Zea-Vera AF, Agudelo-Rojas OL. Disseminated bronchiectasis in an adult with common variable immunodeficiency. Colomb Med (Cali). 2015;46:47-50.
Zea-Vera AF, Estupiñán-López FE, Cifuentes-Burbano J, Vargas MJ, Bonelo A. Interleukin-36 receptor antagonist deficiency (DITRA) with a novel IL36RN homozygous mutation c.200G>T (p.Cys67Phe) in a young Colombian woman. J Clin Immunol. 2019;39:261-3. https://doi.org/10.1007/s10875-019-00622-7
Zea-Vera AF, Chacón MA, Parra B. Antibody deficiencies with normal IgG in adults with noncystic fibrosis bronchiectasis or recurrent pneumonia: Cross-sectional study. Colomb Med. 2022;53. https://doi.org/10.25100/cm.v53i2.4832
Giraldo-Ocampo S, Bonelo A, Zea-Vera AF. B cell subsets in Colombian adults with predominantly antibody deficiencies, bronchiectasis, or recurrent pneumonia. Adv Respir Med. 2022;90:254-66. https://doi.org/10.3390/arm90040035
Fernandes-Pineda M, Matta-Cortés L, Zea-Vera A. Errores innatos de la inmunidad. Acta Med Colomb. 2023;49. https://doi.org/10.36104/amc.2024.3092
European Society for Immunodeficiencies. Registry Working Party List of diseases and genes 2019. Accessed: November 2, 2023. Available at: https://esid.org/Working-Parties/Registry-Working-Party/ESID-Registry/List-of-diseases-and-genes
Giraldo A. Genetic services in Colombia. Community Genets. 2004;7:126-9. https://doi.org/10.1159/000080782
Olaya M, Cleves D, Guzmán T, Torres-Canchala L, Pachajoa H, Medina-Valencia D, et al. Demographic and clinical characterization of pediatric group patients with inborn errors of the immune system in a Colombian tertiary hospital. Allergol Immunopathol (Madr). 2022;50:17-22. https://doi.org/10.15586/aei.v50i4.55
Rosenberg E, Dent PB, Denburg JA. Primary immune deficiencies in the adult: A previously underrecognized common condition. J Allergy Clin Immunol Pract. 2016;4:1101-7. https://doi.org/10.1016/j.jaip.2016.09.004
Wang JJ, Dhir A, Hildebrand KJ, Turvey SE, Schellenberg R, Chen LY, et al. Inborn errors of immunity in adulthood. Allergy Asthma Clin Immunol. 2024;20:6. https://doi.org/10.1186/s13223-023-00862-8
Dorsey MJ, Condino-Neto A. Improving access to therapy for patients with inborn errors of immunity: A call to action. J Allergy Clin Immunol Pract. 2023;11:1698-702. https://doi.org/10.1016/j.jaip.2023.04.019
Boton-Pereira DH, Primo LS, Pelizari G, Flores E, Moraes-Vasconcelos D de, Condino-Neto A, et al. Primary immunodeficiencies in a Mesoregion of São Paulo, Brazil: epidemiologic, clinical, and geospatial approach. Front Immunol. 2020;11. https://doi.org/10.3389/fimmu.2020.00862
Dorsey MJ, Puck JM. Newborn screening for severe combined immunodeficiency in the United States. Immunol Allergy Clin North Am. 2019;39:1-11. https://doi.org/10.1016/j.iac.2018.08.002
Leiva LE, Bezrodnik L, Oleastro M, Condino-Neto A, Costa-Carvalho BT, Sevciovic-Grumach A, et al. Primary immunodeficiency diseases in Latin America: Proceedings of the Second Latin American Society for Immunodeficiencies (LASID) Advisory Board. Allergol Immunopathol (Madr). 2011;39:106-10. https://doi.org/10.1016/j.aller.2010.10.007
Abolhassani H, Avcin T, Bahceciler N, Balashov D, Bata Z, Bataneant M, et al. Care of patients with inborn errors of immunity in thirty J Project countries between 2004 and 2021. Front Immunol. 2022;13. https://doi.org/10.3389/fimmu.2022.1032358
Echeverri EV, Orrego-Arango JC, Arias JAM, Franco JL. Telemedicine for inborn errors of immunity in Colombian patients: Pilot study. Clinical Immunology. 2023;250:109416. https://doi.org/10.1016/j.clim.2023.109416
Seidel MG, Kindle G, Gathmann B, Quinti I, Buckland M, van Montfrans J, et al. The European Society for Immunodeficiencies (ESID) Registry working definitions for the clinical diagnosis of inborn errors of immunity. J Allergy Clin Immunol Pract. 2019;7:1763-70. https://doi.org/10.1016/j.jaip.2019.02.004
Ameratunga R, Lehnert K, Woon S-T. All patients with common variable immunodeficiency disorders (CVID) should be routinely offered diagnostic genetic testing. Front Immunol. 2019;10. https://doi.org/10.3389/fimmu.2019.02678
Elsink K, van Montfrans JM, van Gijn ME, Blom M, van Hagen PM, Kuijpers TW, et al. Cost and impact of early diagnosis in primary immunodeficiency disease: A literature review. Clin Immunol. 2020;213. https://doi.org/10.1016/j.clim.2020.108359
Guaní-Guerra E, Jiménez-Romero AI, García-Ramírez UN, Velázquez-Ávalos JM, Martínez-Guzmán E, Sandoval-Ramírez E, et al. Disease burden for patients with primary immunodeficiency diseases identified at reference hospitals in Guanajuato, Mexico. PLoS ONE. 2017;12:e0175867. https://doi.org/10.1371/journal.pone.0175867
Nabavi M, Arshi S, Bemanian MH, Aghamohammadi A, Mansouri D, Hedayat M, et al. Longterm follow-up of ninety eight Iranian patients with primary immune deficiency in a single tertiary centre. Allergol Immunopathol (Madr). 2016;44:322-30. https://doi.org/10.1016/j.aller.2015.09.006
Reda SM, Afifi HM, Amine MM. Primary immunodeficiency diseases in Egyptian children: A single-center study. J Clin Immunol. 2009;29:343-51. https://doi.org/10.1007/s10875-008-9260-x
Staels F, Collignon T, Betrains A, Gerbaux M, Willemsen M, Humblet-Baron S, et al. Monogenic adult-onset inborn errors of immunity. Front Immunol. 2021;12. https://doi.org/10.3389/fimmu.2021.753978
Al-Tamemi S, Al-Zadjali S, Bruwer Z, Naseem S-U-R, Al-Siyabi N, ALRawahi M, et al. Genetic causes, clinical features, and survival of underlying inborn errors of immunity in Omani patients: A single-center study. J Clin Immunol. 2023;43:452-65. https://doi.org/10.1007/s10875-022-01394-3
Al-Herz W, Moussa MAA. Survival and predictors of death among primary immunodeficient patients: A registry-based study. J Clin Immunol. 2012;32:467-73. https://doi.org/10.1007/s10875-011-9636-1
Modell V, Orange JS, Quinn J, Modell F. Global report on primary immunodeficiencies: 2018 update from the Jeffrey Modell Centers Network on disease classification, regional trends, treatment modalities, and physician reported outcomes. Immunol Res. 2018;66:367-80. https://doi.org/10.1007/s12026-018-8996-5
Locke BA, Dasu T, Verbsky JW. Laboratory diagnosis of primary immunodeficiencies. Clin Rev Allergy Immunol. 2014;46:154-68. https://doi.org/10.1007/s12016-014-8412-4
Some similar items:
- Felipe García, Martha C. Domínguez, Miyerlandi Torres, Óscar Tamayo, William Criollo, Milton Quintana, Adalberto Sánchez, Autoimmune syndrome in the tropical spastic paraparesis/myelopathy associated with human T-lymphotropic virus infections , Biomedica: Vol. 28 No. 4 (2008)
- Marcel Marín, Yudy Alexandra Aguilar, José Robinson Ramírez, Omar Triana, Carlos Enrique Muskus, Molecular and immunological analyses suggest the absence of hydrophilic surface proteins in Leishmania (Viannia) panamensis , Biomedica: Vol. 28 No. 3 (2008)
- Jorge H. Botero, Martha Nelly Montoya, Adriana Lucía Vanegas, Abel Díaz, Luis Navarro-i-Martínez, Fernando Jorge Bornay, Fernando Izquierdo, Carmen del Aguila, Sonia del Pilar Agudelo, Frequency of intestinal microsporidian infections in HIV-positive patients, as diagnosis by quick hot Gram chromotrope staining and PCR. , Biomedica: Vol. 24 No. 4 (2004)
- Paula A. Correa, Luis M. Gómez, Juan Manuel Anaya, Polymorphism of TNF-alpha in autoimmunity and tuberculosis. , Biomedica: Vol. 24 (2004): Suplemento 1
- José Bustos, Yasmin Sánchez, Jhon Medina, Rommy Olivieri, Julián Mojica, Johan Ortiz, Autoimmune encephalitis associated to antibodies against the N-methyl-D-aspartate receptor: Report of two cases , Biomedica: Vol. 37 No. Sup.1 (2017): Suplemento 1, Alteraciones del sistema nervioso
- Pierina D’Angelo, Rossana Celeste Jaspe, Carmen Luisa Loureiro, Cristina Gutiérrez, María Zulay Sulbarán, Yoneira Sulbarán, Felix Toro, Flor Helene Pujol, Performance of molecular methods for identification of unusual subtypes of hepatitis C virus genotype 2 , Biomedica: Vol. 38 No. 2 (2018)
- Germán Briceño, Jaime Céspedes, Martha Leal, Sarha Vargas, Prevalence of cardiovascular risk factors in schoolchildren from a rural and urban area in Colombia , Biomedica: Vol. 38 No. 4 (2018)
- Judith Sofía García , María Paula Sarmiento , Jesús David Bello , Nora Alejandra Zuluaga, Adriana Carolina Forero , Laura Fernanda Niño , Hyperthyroidism in children and adolescents: Experience in a university hospital in Colombia , Biomedica: Vol. 42 No. 2 (2022)
- Mónica Fernandes-Pineda , Andrés F. Zea-Vera, Lymphoproliferation and hyper-IgM as the first manifestation of activated phosphoinositide 3-kinase δ syndrome: A case report , Biomedica: Vol. 44 No. Sp. 2 (2024): Inmunología clínica
- Iván Insignares, Luis E. Rodríguez, Óscar Correa-Jiménez, Alberto Alfaro-Murillo, Laura Rincón-Arenas, Andrés Sánchez, Marlon Múnera , Autoimmunity against cytokines: Double strike in autoimmune disease, a historical perspective , Biomedica: Vol. 44 No. Sp. 2 (2024): Inmunología clínica
Copyright (c) 2024 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























