Microcephaly in Colombia before the Zika outbreak: A systematic literature review
Abstract
Introduction: Microcephaly is characterized by a smaller than normal head circumference. Recently, Zika virus (ZV) has been associated with microcephaly.
Objective: To describe the prevalence of microcephaly in Colombia taking as the baseline the information from the period before the Zika virus infection epidemics.
Materials and methods: We reviewed Medline, Scopus, Scielo, Lilacs and annual reports of congenital malformation monitoring systems across Latin America, among others sources, for articles published before April, 2015, reporting the prevalence of microcephaly in Colombia between 1982 and 2013.
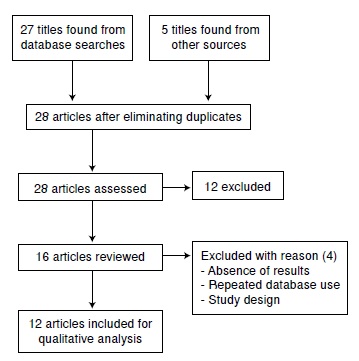
Results: We identified 32 non-duplicate articles; we selected 25 articles for revision of which 12 met the criteria for inclusion in the systematic review, including 2,808,308 births.
Conclusions: The prevalence of microcephaly in Colombia from 1982 to 2013, before the introduction of ZV, ranged from 0.3 to 3.1 per 10,000 births, with an average of 1.8 (95% CI 1.7-1.8) per 10,000 births. These findings are important to determine if the prevalence after the introduction of the Zika virus infection registered significant changes.
Downloads
References
Ministerio de Salud, Instituto Nacional de Salud. Protocolo de Vigilancia en Salud Pública: defectos congénitos. Bogotá: Instituto Nacional de Salud; 2014.
Ashwal S, Michelson D, Plawner L, Dobyns WB, Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Practice parameter: Evaluation of the child with microcephaly (an evidence-based review): Report of the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society. Neurology. 2009;73:887-97. https://doi.org/10.1212/WNL.0b013e3181b783f7
World Health Organization. Screening, assessment and management of neonates and infants with complications associated with Zika virus exposure in utero. Geneva: World Health Organization; 2016.
Jaworski M, Hersh JH, Donat J, Shearer LT, Weisskopf B. Computed tomography of the head in the evaluation of microcephaly. Pediatrics. 1986;78:1064-9.
Steinlin M, Zürrer M, Martin E, Boesch C, Largo RH, Boltshauser E. Contribution of magnetic resonance imaging in the evaluation of microcephaly. Neuropediatrics. 1991;22:184-9. https://doi.org/10.1055/s-2008-1071438
Sugimoto T, Yasuhara A, Nishida N, Murakami K, Woo M, Kobayashi Y. MRI of the head in the evaluation of microcephaly. Neuropediatrics. 1993;24:4-7. https://doi.org/10.1055/s-2008-1071504
Opitz JM, Holt MC. Microcephaly: General considerations and aids to nosology. J Craniofac Genet Dev Biol. 1990;10:175-204.
Stoll C. Problems in the diagnosis of fragile X syndrome in young children are still present. Am J Med Genet. 2001;100:110-5. https://doi.org/10.1002/1096-8628(20010422)100:2<110::AID-AJMG1242>3.0.CO;2-I
Dolk H. The predictive value of microcephaly during the first year of life for mental retardation at seven years. Dev Med Child Neurol. 1991;33:974-83. https://doi.org/10.1111/j.1469-8749.1991.tb14813.x
Rasmussen SA, Jamieson DJ, Honein MA, Petersen LR. Zika virus and birth defects--reviewing the evidence for causality. N Engl J Med. 2016;374:1981-7. https://doi.org/10.1056/NEJMsr1604338
Mysorekar IU, Diamond MS. Modeling Zika virus infection in pregnancy. N Engl J Med. 2016;375:481-4. https://doi.org/10.1016/j.cell.2016.05.008
Mlakar J, Korva M, Tul N, Popović M, Poljšak-Prijatelj M, Mraz J, et al. Zika virus associated with microcephaly. N Engl J Med. 2016;374:951-8. https://doi.org/10.1056/NEJMoa1600651
Schuler-Faccini L, Ribeiro EM, Feitosa IM, Horovitz DD, Cavalcanti DP, Pessoa A, et al. Possible association between zika virus infection and microcephaly - Brazil, 2015. MMWR Morb Mortal Wkly Rep. 2016;65:59-62. https://doi.org/10.15585/mmwr.mm6503e2
World Health Organization. Disease outbreak news. Microcephaly-Brazil. 2016;91:237-48. Accessed: June 22, 2018. Available at: http://www.who.int/wer/2016/wer9118/en/
World Health Organization. Microcephaly – Brazil. Weekly Epidemiological Record. Accessed: June 22, 2018. Available at: http://www.who.int/csr/don/8-january-2016-brazilmicrocephaly/en/
Gulland A. Zika virus is a global public health emergency, declares WHO. BMJ. 2016;352:i657. https://doi.org/10.1136/bmj.i657
Fauci AS, Morens DM. Zika virus in the Americas — yet another arbovirus threat. N Engl J Med. 2016;374:601-4. https://doi.org/10.1056/NEJMp1600297
Rubin EJ, Greene MF, Baden LR. Zika virus and microcephaly. N Engl J Med. 2016;374:984-5. https://doi.org/10.1056/NEJMe1601862
Kumar A, Singh HN, Pareek V, Raza K, Dantham S, Kumar P, et al. A possible mechanism of Zika virus associated microcephaly: Imperative Role of Retinoic Acid Response Element (RARE) Consensus Sequence Repeats in the Viral Genome. Front Hum Neurosci. 2016;10:403. https://doi.org/10.3389/fnhum.2016.00403
Mawson AR. Pathogenesis of Zika virus-associated embryopathy. Biores Open Access. 2016;5:171-6. https://doi.org/10.1089/biores.2016.0004
Huang W-C, Abraham R, Shim B-S, Choe H, Page DT. Zika virus infection during the period of maximal brain growth causes microcephaly and corticospinal neuron apoptosis in wild type mice. Sci Rep. 2016;6:34793. https://doi.org/10.1038/srep34793
Pacheco O, Beltrán M, Nelson CA, Valencia D, Tolosa N, Farr SL, et al. Zika virus disease in Colombia - preliminary report. N Engl J Med. 2016. p. 1-10. https://doi.org/10.1056/NEJMoa1604037
Porras GL, León OM, Molano J, Quiceno SL, Pachajoa H, Montoya JJ. Prevalencia de defectos congénitos en Risaralda, 2010-2013. Biomédica. 2016;36:556-63. https://doi.org/10.7705/biomedica.v36i4.2771
Carmona RH. The global challenges of birth defects and disabilities. Lancet. 2005;366:1142-4. https://doi.org/10.1016/S0140-6736(05)67459-4
Medina MR. Geografía de la mortalidad infantil en Colombia, 1985-1994. Bogotá: Departamento Administrativo Nacional de Estadística (DANE); 1999.
González Y. Informe final del evento anomalías congénitas hasta el periodo epidemiológico 13 del año 2012. Bogotá:Instituto Nacional de Salud; 2012.
Observatorio Nacional de Salud. Tercer informe ONS: Mortalidad evitable en Colombia para 1998-2011. Bogotá: Instituto Nacional de Salud; 2014.
Organización Mundial de la Salud. Estadísticas sanitarias mundiales, 2014. Geneva: Organización Mundial de la Salud; 2014. p. 13-22.
García H, Salguero GA, Moreno J, Arteaga C, Giraldo A. Frecuencia de anomalías congénitas en el Instituto Materno-Infantil, Bogotá. Biomédica. 2003;23:161-72.
https://doi.org/10.7705/biomedica.v23i2.1208
Victora CG, Schuler-Faccini L, Matijasevich A, Ribeiro E, Pessoa A, Barros FC. Microcephaly in Brazil: How to interpret reported numbers? Lancet. 2016;387:621-4.
https://doi.org/10.1016/S0140-6736(16)00273-7
Boom JA. Microcephaly in infants and children: Etiology and evaluation. Accessed on: June 22, 2018. Available at: https://www.uptodate.com/contents/microcephaly-in-infantsand-children-etiology-and-evaluation 32. Roche AF, Mukherjee D, Guo SM, Moore WM. Head circumference reference data: Birth to 18 years. Pediatrics. 1987;79:706-12.
Estudio Colaborativo Latino Americano de Malformaciones Congénitas. Microcefalia no ECLAMC e no Brasil. Buenos Aires: Estudio Colaborativo Latino-Americano de Malformaciones Congénitas; 2015.
Some similar items:
- Gloria Liliana Porras-Hurtado, Olga Mercedes León-Castañeda, Jaime Molano-Hurtado, Sandra Lorena Quiceno, Harry Pachajoa, Juan José Montoya, Prevalence of birth defects in Risaralda, 2010-2013 , Biomedica: Vol. 36 No. 4 (2016)
- Nataly Orozco-Hoyos , Armando Baena, Carolina Montoya-Ruiz, Gloria I. Sánchez, Eliana Restrepo , Prevalence of Chlamydia trachomatis in an asymptomatic female population attending cervical cytology services of three healthcare centers in Medellín, Colombia , Biomedica: Vol. 40 No. 3 (2020)
- Julián A. Fernández-Niño, Claudia I. Astudillo-García, Laura María Segura, Natalia Gómez, Ángela Skantria Salazar, Juan Hember Tabares, Cristian Andrés Restrepo, Miguel Ángel Ruiz, Myriam Consuelo López, Patricia Reyes, Profiles of intestinal polyparasitism in a community of the Colombian Amazon region , Biomedica: Vol. 37 No. 3 (2017)
- María Isabel Bermúdez-Forero, Maritza Berrío-Pérez, Andrea Magally Herrera-Hernández, Magda Juliana Rodríguez-Rodríguez, Sandra García-Blanco, Guillermo Orjuela-Falla, Mauricio Beltrán, Prevalence of human T-cell lymphotropic virus I and II in Colombian blood donors, 2001-2014: Implications for transfusion safety , Biomedica: Vol. 36 (2016): Suplemento 2, Enfermedades virales
- Angélica María Ramírez, Yesmit Karina Ríos, Néstor Fabián Galvis, Elsie Entrena, Nidia Victoria Mariño, Diana Marcela Rangel, María Alejandra Araque, Darlis Mayerlis Cabarique, Mateo Murillo , Jorge Enrique Gómez-Marín, Seroprevalence and molecular detection of Toxoplasma gondii among donors in a blood bank in Cúcuta, Colombia Introduction: Toxoplasma gondii infection , Biomedica: Vol. 39 No. Supl. 2 (2019): Enfermedades transmisibles en el trópico, agosto
- María Luz Gunturiz, Liliana Cortés, Ester Liliana Cuevas, Pablo Chaparro, Martha Lucía Ospina, Congenital cerebral toxoplasmosis, Zika and chikungunya virus infections: a case report , Biomedica: Vol. 38 No. 2 (2018)
- Carolina Montoya, Priscila Bascuñán, Julián Rodríguez-Zabala, Margarita M. Correa, Abundance, composition and natural infection of Anopheles mosquitoes from two malaria-endemic regions of Colombia , Biomedica: Vol. 37 No. Sup. 2 (2017): Suplemento 2, Entomología médica, 2017
- Mónica Marcela Jiménez, Jesús Arias, Gabriel Carrasquilla, Seroprevalence of dengue infection in the municipalities of Armenia, Calarcá, La Tebaida and Montenegro in Quindío, 2014 , Biomedica: Vol. 37 No. 1 (2017)
- Diana Marcela Echeverry, Juan Miguel Rengifo, Jhon Carlos Castaño, Germán Alberto Téllez, María Mercedes González, Prevalence of Mammomonogamus laryngeus (Strongylida: Syngamidae) nematodes in a bovine slaughterhouse , Biomedica: Vol. 31 No. 3 (2011)
- Guillermo Mora, María Clara Echeverry, Gustavo Enrique Rey, Myriam Consuelo López, Luisa Fernanda Posada, Fabio Aurelio Rivas, Frequency of Trypanosoma cruzi infection in patients with implanted pacemaker , Biomedica: Vol. 27 No. 4 (2007)
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























