Seroprevalence and molecular detection of Toxoplasma gondii among donors in a blood bank in Cúcuta, Colombia Introduction: Toxoplasma gondii infection
Abstract
Introduction: Toxoplasma gondii infection manifests differently in humans according to their immunity ranging from asymptomatic profiles to severe disease. There are multiple transmission mechanisms including blood transfusions, but little is known about the frequency of T. gondii infection in Colombia’s blood banks.
Objective: To determine the prevalence of T. gondii infection in blood donors of a blood bank in the city of Cúcuta by serological and molecular diagnostic techniques.
Materials and methods: We identified IgG and IgM antibodies against T. gondii by immunoassay in serum from 348 donors. The frequency of T. gondii DNA was determined by polymerase chain reaction (PCR) in whole blood from seropositive donors and relevant variables were analyzed based on the information obtained from surveys during blood donor selection.
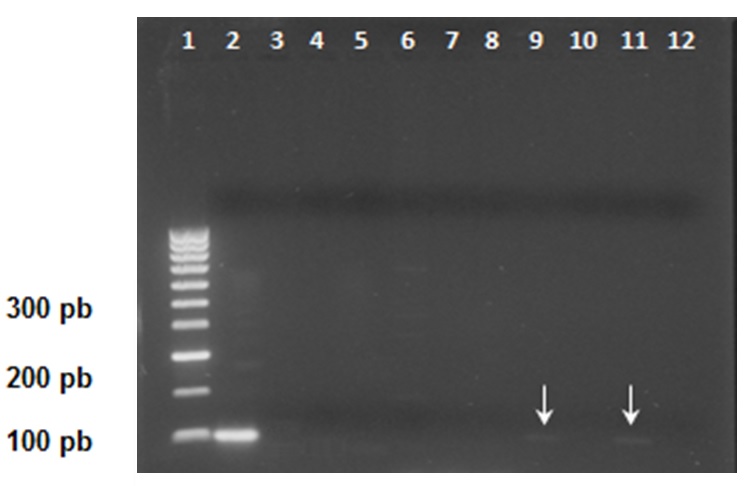
Results: Out of the 348 enrolled donors, 134 (38.5%) showed IgG antibodies against T. gondii; two of them (0.6%) had both IgG and IgM, and in two of them (1.5%), parasite DNA was detected in blood samples. A bivariate analysis indicated an association between seropositivity to T. gondii and being over 26 years of age (p=0.020).
Conclusions: The prevalence of T. gondii infection found in the blood donors of this study suggests a significant exposure to the infectious agent that becomes relevant when parasitemia is detected.
Downloads
References
Gómez-Marín JE. Toxoplasmosis. En: Gómez Marín JE, editor. Protozoología médica: protozoos parásitos en el contexto latinoamericano. Primera edición. Bogotá: Editorial Manual Moderno; 2010. p. 65-85.
Robert-Gangneux F, Dardé ML. Epidemiology of and diagnostic strategies for toxoplasmosis. Clin Microbiol Rev. 2012;25:264-96. https://doi.org/10.1128/CMR.05013-11
Dard C, Fricker-Hidalgo H, Brenier-Pinchart M, Pelloux H. Relevance of and new developments in serology for toxoplasmosis. Trends Parasitol. 2016;32:492-506. https://doi.org/10.1016/j.pt.2016.04.001
Díaz AD, Aristizábal BH. Métodos tradicionales y moleculares en el diagnóstico de la toxoplasmosis y su aplicación en el contexto clínico. Medicina UPB. 2013;32:54-67.
Pérez JE, Villada JS, Naranjo OD, Castaño SV. Formas alternas de transmisión de Toxoplasma gondii. Biosalud. 2011;10:123-37.
Siegel SE, Lunde MN, Levine AS, Graw RJ, Miller RW. Transmission of toxoplasmosis by leukocyte (WBC) transfusion. Pediatr Res. 1970;4:461. https://doi.org/10.1203/00006450-197009000-00107
Gómez-Marín JE, de la Torre A, Ángel-Muller E, Rubio J, Arenas J, Osorio E, et al. First Colombian multicentric newborn screening for congenital toxoplasmosis. PLoS Negl Trop Dis. 2011;5:e1195. https://doi.org/10.1371/journal.pntd.0001195
Foroutan-Rad M, Majidiani H, Dalvand S, Daryani A, Kooti W, Saki J, et al. Toxoplasmosis in blood donors: A systematic review and meta-analysis. Transfus Med Rev. 2016;30:116-22. https://doi.org/10.1016/j.tmrv.2016.03.002
van der Colf BE, Noden BH, Wilkinson R, Chipare I. Low seroprevalence of antibodies to Toxoplasma gondii in blood donors in central Namibia. S Afr J Infect Dis. 2014;29:101-4. https://doi.org/10.1080/23120053.2014.11441579
Coêlho RA, Kobayashi M, Carvalho Jr. LB. Prevalence of IgG antibodies specific to Toxoplasma gondii among blood donors in Recife, Northeast Brazil. Rev Inst Med Trop Sao Paulo. 2003;45:229-31. https://doi.org/10.1590/S0036-46652003000400011
Elhence P, Agarwal P, Prasad KN, Chaudhary RK. Seroprevalence of Toxoplasma gondii antibodies in North Indian blood donors: Implications for transfusion transmissible toxoplasmosis. Transfus Apher Sci. 2010;43:37-40. https://doi.org/10.1016/j.transci.2010.05.004
Alvarado-Esquivel C, Mercado-Suárez MF, Rodríguez-Briones A, Fallad-Torres L, Ayala-Ayala JO, Nevarez-Piedra LJ, et al. Seroepidemiology of infection with Toxoplasma gondii in healthy blood donors of Durango, México. BMC Infect Dis. 2007;7:75. https://doi.org/10.1186/1471-2334-7-75
Pinlaor S, Leamviteevanich K, Pinlaor P, Maleewong W, Pipitgool V. Seroprevalence of specific total immunoglobulin (Ig), IgG and IgM antibodies to Toxoplasma gondii in blood donors from Loei Province, Northeast Thailand. S Afr J Infect Dis. 2000;31:123-7.
Jafari Modrek M, Mousavi M, Saravani R. Toxoplasma gondii seroprevalence among blood donors in Zahedan, Southeastern Iran. Int J Infect. 2014;1:e21111. https://doi.org/10.17795/iji-21111
Zainodini N, Zare-Bidaki M, Abdollahi SH, Afrooz M, Ziaali N, Ebrahimian M, et al. Molecular and serological detection of acute and latent toxoplasmosis using real-time PCR and ELISA techniques in blood donors of Rafsanjan City, Iran, 2013. Iran J Parasitol. 2014;9:336-41.
Sarkari B, Shafiei R, Zare M, Sohrabpour S, Kasraian L. Seroprevalence and molecular diagnosis of Toxoplasma gondii infection among blood donors in southern Iran. J Infect Dev Ctries. 2014;8:543-47. https://doi.org/10.3855/jidc.3831
Chiang TY, Hsieh HH, Kuo MC, Chiu KT, Lin WC, Fan CK, et al. Seroepidemiology of Toxoplasma gondii Infection among healthy blood donors in Taiwan. PLoS One. 2012;7:e48139. https://doi.org/10.1371/journal.pone.0048139
Vasina S, Dunaeva Z. On the length of survival of Toxoplasma outside the host organism. Med Prom SSSR.1960;29:451-4.
Singh G, Sehgal R. Transfusion-transmitted parasitic infections. Asian J Transf Sci. 2010;4:73-7. https://doi.org/10.4103/0973-6247.67018
Shulman I. Parasitic infections and their impact on blood donor selection and testing. Arch Pathol Lab Med. 1994;118:366-70.
Stramer S, Hollinger F, Katz L, Kleinman S, Metzel P, Gregory K, et al. Emerging infectious disease agents and their potential threat to transfusion safety. Transfusion. 2009;49:1S-29S. https://doi.org/10.1111/j.1537-2995.2009.02279.x
Cañón-Franco WA, López-Orozco N, Gómez-Marín JE, Dubey JP. An overview of seventy years of research (1944 – 2014) on toxoplasmosis in Colombia, South America. Parasit Vectors. 2014;7:427. https://doi.org/10.1186/1756-3305-7-427
Su C, Khan A, Zhou P, Majumdar D, Ajzenberg D, Dardé ML, et al. Globally diverse Toxoplasma gondii isolates comprise six major clades originating from a small number of distinct ancestral lineages. Proc Natl Acad Sci USA. 2012;109:5844-9. https://doi.org/10.1073/pnas.1203190109
Sánchez V, de la Torre A, Gómez-Marín JE. Characterization of ROP18 alleles in human toxoplasmosis. Parasitol Int. 2014;63:463-9. https://doi.org/10.1016/j.parint.2013.10.012
Torres-Morales E, Taborda L, Cardona N, de la Torre A, Sepúlveda-Arias JC, Patarroyo MA, et al. Th1 and Th2 immune response to P30 and ROP18 peptides in human toxoplasmosis. Med Microbiol Immunol. 2014;203:315-22. https://doi.org/10.1007/s00430-014-0339-0
Pernas L, Ramírez R, Holmes TH, Montoya JG, Boothroyd JC. Immune profiling of pregnant Toxoplasma-infected US and Colombia patients reveals surprising impacts of infection on peripheral blood cytokines. J Infect Dis. 2014;210:923-31. https://doi.org/10.1093/infdis/jiu189
Jewell M, Thompson D, Frenkel J. Toxoplasmosis: títulos de anticuerpos en humanos y gatos domésticos de Medellín, Colombia. Antioquia Med. 1973;23:145-52.
Betancur CA, Jaramillo JM, Puyana JD, Quintero MI, Estrada S, Salazar LM. Seroprevalencia de toxoplasmosis en donantes de sangre de la Clínica Cardiovascular Santa María, Medellín, Colombia, 2009-2010. Infectio. 2011;15:14-9.
Coordinación Red Nacional de Bancos de Sangre y Servicios de Transfusión, Instituto Nacional de Salud. Leucorreducción de componentes sanguíneos. Documento técnico. Fecha de consulta: 20 de diciembre de 2017. Disponible en: https://www.ins.gov.co/Direcciones/RedesSaludPublica/DonacionSangre/Publicaciones/Manual%20Leucoreduccion.pdf
Coordinación Red Nacional de Bancos de Sangre y Servicios de Transfusión, Instituto Nacional de Salud. Anexo Técnico Circular No.1-Circular No.0082 de 2011. Fecha de consulta: 21 de julio de 2017. Disponible en: https://www.ins.gov.co/Direcciones/RedesSaludPublica/DonacionSangre/NormatividadRelNalBancosSangro/Anexo%20Tecnico%203%20Circular%200082%20de%202011.pdf
E.S.E. Hospital Universitario Erasmo Meoz. herasmomeoz.gov.co. Fecha de consulta: 29 de septiembre de 2017. Disponible en: http://www.herasmomeoz.gov.co/index.php
Osorio A, Melo A, Herrera A, Patiño A, Niño B, Reina B, et al. Guía para la selección y atención de donantes de sangre y hemocomponentes en Colombia. Bogotá: Instituto Nacional de Salud; 2012. Fecha de consulta: 21 de julio de 2017. Disponible en: https://www.ins.gov.co/Direcciones/RedesSaludPublica/DonacionSangre/Publicaciones/Gu%C3%ADa%20para%20Selecci%C3%B3n%20de%20Donantes%20de%20Sangre%20en%20Colombia%202013.pdf
Cardona N, Basto N, Parra B, Zea AF, Pardo CA, Bonelo A, et al. Detection of Toxoplasma DNA in the peripheral blood of HIV-positive patients with neuro-opportunistic infections by a real-time PCR assay. J Neuroparasitology. 2011; 2:1-6. https://doi.org/10.4303/jnp/N110402
Ministerio de Salud y Protección Social. Análisis de situación de salud de poblaciones diferenciales relevantes. Colombia. Fecha de consulta: 13 de julio de 2016. Disponible en: https://www.minsalud.gov.co/sites/rid/Lists/BibliotecaDigital/RIDE/VS/ED/PSP/IMP+MS_ASIS_PoblDiferenciales.pdf
Departamento Administrativo Nacional de Estadística. Estratificación socioeconómica. Fecha de consulta: 15 de octubre de 2017. Disponible en: http://www.dane.gov.co/index.php/servicios-al-ciudadano/servicios-de-informacion/estratificacionsocioeconomica#preguntas-frecuentes
Gómez-Marín JE, de la Torre A, Barrios P, Cardona N, Álvarez C, Herrera C. Toxoplasmosis in military personnel involved in jungle operations. Acta Trop. 2012;122:46-51. https://doi.org/10.1016/j.actatropica.2011.11.019
Vallochi A, Goldberg A, Falcai A, Ramasawmy R, Kalil J, Silveira C, et al. Molecular markers of susceptibility to ocular toxoplasmosis, host and guest behaving badly. Clin Ophthalmol. 2008;2:837-48. https://doi.org/10.2147/OPTH.S1629
Loges L, González B, Farias-da-Rosa N. Seroprevalence and associated factors to Toxoplasma gondii infection in blood donors in Southern Brazil. Rev Panam Infectol. 2012;14:27-31.
La Opinión. Temperatura en Cúcuta aumentó 2,2 °C. 2016. Fecha de consulta: 21 de diciembre de 2017. Disponible en: https://www.laopinion.com.co/cucuta/temperatura-encucuta-aumento-22-degc-ideam-106636#OP
WHO Expert Group. Expert Consensus Statement on achieving self-suffciency in safe blood and blood products, based on voluntary non-remunerated blood donation (VNRBD). Vox Sanguinis. 2012;103:337-42. https://doi.org/10.1111/j.1423-0410.2012.01630.x
Morales J, Fuentes-Rivera J, Delgado-Silva C, Matta-Solís H. Marcadores de infección para hepatitis viral en donantes de sangre de un hospital nacional de Lima metropolitana. Rev Peru Med Exp Salud Pública. 2017;34:466-71. https://doi.org/10.17843/rpmesp.2017.343.2503
Mahmood S, AL-Qadhi B, Zghair K. Prevalence of toxoplasmosis of male blood donors in Baghdad. Iraqui Journal of Science. 2013;54:832-41.
Alvarado-Esquivel C, Sánchez-Anguiano LF, Hernández-Tinoco J, Ramos-Nevarez A, Estrada-Martínez S, Cerrillo-Soto SM, et al. Association between Toxoplasma gondii
infection and history of blood transfusion: A case-control seroprevalence study. J Int Med Res. 2018;46:1626-33. https://doi.org/10.1177/0300060518757928
Bastien P. Molecular diagnosis of toxoplasmosis. Trans R Soc Trop Med Hyg. 2002;96:S205-S15. https://doi.org/10.1016/S0035-9203(02)90078-7
Ivovic V, Vujanic M, Zivkovic T, Klun I, Djurkovic-Djakovic O. Molecular detection genotyping of Toxoplasma gondii from clinical samples. Intechopen. 2012 Fecha de consulta: 9 de septiembre de 2017. Disponible en: https://www.intechopen.com/books/toxoplasmosisrecent-advances/molecular-detection-and-genotyping-of-toxoplasma-gondii-from- andclinical-samples
Silveira C, Vallochi AL, da Silva UR, Muccioli C, Holland GN, Nussenblatt RB, et al. Toxoplasma gondii in the peripheral blood of patients with acute and chronic toxoplasmosis. J Ophthalmology. 2010;95:396-400. https://doi.org/10.1136/bjo.2008.148205
Bianchi M, Vaglio S, Pupella S, Marano G, Facco G, Liumbruno GM, et al. Leucoreduction of blood components: An effective way to increase blood safety? Blood Transfus. 2016;14:214-27. https://doi.org/10.2450/2015.0154-15
Some similar items:
- Sebastián Posada-Bustos, Ana Cristina Mariño , Eugenia Espinosa-García , Clinical outcomes of pediatric patients with congenital toxoplasmosis in a fourthlevel center Introduction. Congenital , Biomedica: Vol. 44 No. 4 (2024)
- Armando Daniel Cortés, Natalia Aguirre, Severe disseminated acute toxoplasmosis in an adult immunocompetent patient from the Colombian Pacific , Biomedica: Vol. 38 No. Sup. 2 (2018): Suplemento 2, Medicina tropical
- Liliana María Zuluaga, John Camilo Hernández, Carlos Felipe Castaño, Jorge Hernando Donado, Effect of antenatal spiramycin treatment on the frequency of retinochoroiditis due to congenital toxoplasmosis in a Colombian cohort , Biomedica: Vol. 37 No. Sup.1 (2017): Suplemento 1, Alteraciones del sistema nervioso
- Estephania Candelo, Gabriela Caicedo, Max Feinstein, Harry Pachajoa, Microcephaly in Colombia before the Zika outbreak: A systematic literature review , Biomedica: Vol. 38 No. Sup. 2 (2018): Suplemento 2, Medicina tropical
- Paola Andrea Rueda , Sara Orozco , Juan Raúl Castro , Ángela María Londoño, Elsa María Vásquez, Andrea Arango, Carlos Esteban Builes , Incidence and prevalence of vitiligo by gender and age in the Colombian population , Biomedica: Vol. 45 No. 4 (2025)
- María Isabel Bermúdez-Forero, Maritza Berrío-Pérez, Andrea Magally Herrera-Hernández, Magda Juliana Rodríguez-Rodríguez, Sandra García-Blanco, Guillermo Orjuela-Falla, Mauricio Beltrán, Prevalence of human T-cell lymphotropic virus I and II in Colombian blood donors, 2001-2014: Implications for transfusion safety , Biomedica: Vol. 36 (2016): Suplemento 2, Enfermedades virales
- Beatriz Eugenia Ferro, Ana Lucía Rodríguez, Mauricio Pérez, Bruno Luis Travi, Seroprevalence of Leptospira infection in habitants of peripheral neighborhoods in Cali, Colombia. , Biomedica: Vol. 26 No. 2 (2006)
- Julián A. Fernández-Niño, Claudia I. Astudillo-García, Laura María Segura, Natalia Gómez, Ángela Skantria Salazar, Juan Hember Tabares, Cristian Andrés Restrepo, Miguel Ángel Ruiz, Myriam Consuelo López, Patricia Reyes, Profiles of intestinal polyparasitism in a community of the Colombian Amazon region , Biomedica: Vol. 37 No. 3 (2017)
- Mauricio Beltrán, Andrea Herrera, Astrid Carolina Flórez, Maritza Berrio, María Isabel Bermúdez, Detection of Trypanosoma cruzi antibodies in multitransfused patients in Colombia , Biomedica: Vol. 37 No. 3 (2017)
- Diana Marcela Echeverry, Juan Miguel Rengifo, Jhon Carlos Castaño, Germán Alberto Téllez, María Mercedes González, Prevalence of Mammomonogamus laryngeus (Strongylida: Syngamidae) nematodes in a bovine slaughterhouse , Biomedica: Vol. 31 No. 3 (2011)
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























