Direct costs of neonatal infection acquired in the community in full-term newborns and low risk at birth, Cundinamarca, Colombia
Abstract
Introduction: Half of the episodes of neonatal sepsis are acquired in the community with a high percentage of mortality and complications.
Objective: To estimate the direct costs of hospitalizations due to systemic neonatal infection acquired in the community in low-risk newborns.
Materials and methods: For the estimation of costs, we used the perspective of the health systems and the microcosting technique and we established the duration of hospitalization as the time horizon. We identified cost-generating events through expert consensus and the quantification was based on the detailed bill of 337 hospitalized newborns diagnosed with neonatal infection. The costs of the medications were calculated based on the drug price information system (SISMED) and the ISS 2001 rate manuals adjusting percentage, and the mandatory insurance rates for traffic accidents (SOAT). We used the bootstrapping method for cost distribution to incorporate data variability in the estimate.
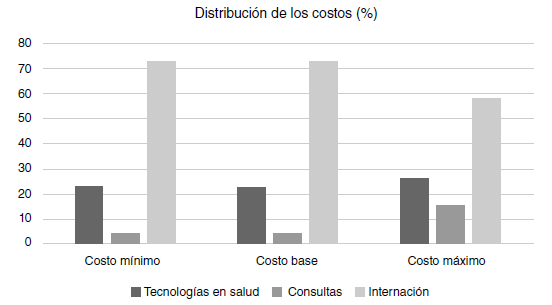
Results: We included the medical care invoices for 337 newborns. The average direct cost of care per patient was USD$ 2,773,965 (Standard Deviation, SD=USD$ 198,813.5; 95% CI: $ 2,384,298 - $ 3,163,632). The main cost-generating categories were hospitalization in intensive care units and health technologies. The costs followed a log-normal distribution.
Conclusions: The categories generating the greatest impact on the care costs of newborns with infection were hospitalization in neonatal units and health technologies. The costs followed a log-normal distribution.
Downloads
References
Yang X, Meng T. Admission of full-term infants to the neonatal intensive care unit: A 9.5-year review in a tertiary teaching hospital. J Matern Neonatal Med. 2020;33:3003-9. https://doi.org/10.1080/14767058.2019.1566901
Santos Burgoa-Larrañaga L, Iglesias-Leboreiro J, Bernardez-Zapata I. Early discharge of the healthy newborn from the nursery of the Hospital Español de México. Rev Med Inst Mex Seguro Soc. 2016;54:696-705.
Harron K, Gilbert R, Cromwell D, Oddie S, van der Meulen J. Newborn length of stay and risk of readmission. Paediatr Perinat Epidemiol. 2017;31:221-32. https://doi.org/10.1111/ppe.12359
Waters D, Jawad I, Ahmad A, Lukšić I, Nair H, Zgaga L, et al. Aetiology of communityacquired neonatal sepsis in low- and middle-income countries. J Glob Health. 2011;1:154-70.
Weber MW, Carlin JB, Gatchalian S, Lehmann D, Muhe L, Mulholland EK. Predictors of neonatal sepsis in developing countries. Pediatr Infect Dis J. 2003;22:711-7. https://doi.org/10.1097/01.inf.0000078163.80807.88
Osrin D, Vergnano S, Costello A. Serious bacterial infections in newborn infants in developing countries. Curr Opin Infect Dis. 2004;17:217-24. https://doi.org/10.1097/00001432-200406000-00008
Downie L, Armiento R, Subhi R, Kelly J, Clifford V, Duke T. Community-acquired neonatal and infant sepsis in developing countries: Efficacy of WHO’s currently recommended antibiotics -Systematic review and meta-analysis. Arch Dis Child. 2013;98:146-54. https://doi.org/10.1136/archdischild-2012-30203
Jaramillo-Mejía MC, Chernichovsky D, Jiménez-Moleón JJ. Brechas regionales de la mortalidad infantil en Colombia. Rev Peru Med Exp Salud Pública. 2014;30:550-9.
Stoll BJ, Gary L. Darmstadt AK. Neonatal infections: A global perspective. En: Wilson C, Nizet V, Maldonado Y, Remington J. Klein J, editors. Remington and Klein’s Infectious diseases of the fetus and newborn infant. Eighth edition. Amsterdam: Saunders; 2016. p. 24-53.
Bulkowstein S, Ben-Shimol S, Givon-Lavi N, Melamed R, Shany E, Greenberg D. Comparison of early onset sepsis and community-acquired late onset sepsis in infants less than 3 months of age. BMC Pediatr. 2016;16:82. https://doi.org/10.1186/s12887-016-0618-6
Lantos JD, Meadow WL. Costs and end-of-life care in the NICU: Lessons for the MICU? J Law, Med Ethics. 2011;39:194-200. https://doi.org/10.1111/j.1748-720X.2011.00588.x
Mugford M. Outcome and cost of neonatal intensive care. Curr Paediatr. 1994;4:30-2.
WHO. Disease burden and mortality estimates. Geneva: WHO; 2019. Fecha de consulta: 6 de agosto de 2020. Disponible en: http://www.who.int/healthinfo/global_burden_disease/estimates/en/
Murthy S, John D, Godinho IP, Godinho MA, Guddattu V, Nair NS. A protocol for a systematic review of economic evaluation studies conducted on neonatal systemic infections in South Asia. Syst Rev. 2017;6:252. https://doi.org/10.1186/s13643-017-0648-7
Mejía-Mejía A, Moreno-Viscaya M. Evaluación económica para la toma de decisiones en salud en Colombia. Superintendencia Nacional de Salud. 2014;5:70-7.
Departamento Administrativo Nacional de Estadísticas, DANE. Defunciones no fetales. Internet. Primeras causas de defunción. 2019. Fecha de consulta: 6 de agosto de 2020. Disponible en: https://www.dane.gov.co/index.php/estadisticas-por-tema/salud/nacimientosy-defunciones/defunciones-no-fetales
Liu L, Oza S, Hogan D, Chu Y, Perin J, Zhu J, et al. Global, regional, and national causes of under-5 mortality in 2000–15: An updated systematic analysis with implications for the Sustainable Development Goals. Lancet. 2016;388:3027-35. https://doi.org/10.1016/S0140-6736(16)31593-8
Cheah IGS. Economic assessment of neonatal intensive care. Transl Pediatr. 2019;8:246-56. https://doi.org/10.21037/tp.2019.07.03
Alvarado-Jaramillo JC, Gonzáles-Ramos AJ, Mendoza-Arana P. Análisis de costos en dos unidades de cuidados intensivos pediátricos del Ministerio de Salud del Perú. Anales de la Facultad de Medicina. 2011;72:249-54.
Shanmugasundaram R, Padmapriya E, Shyamala J. Cost of neonatal intensive care. Indian J Pediatr. 1998;65:249-55. https://doi.org/10.1007/BF02752301
Profit J, Lee D, Zupancic JA, Papile L, Gutiérrez C, Goldie SJ, et al. Clinical benefits, costs, and cost-effectiveness of neonatal intensive care in México. PLoS Med. 2010;7:e1000379. https://doi.org/10.1371/journal.pmed.1000379
Amador-Morán R, Labrada-Despaigne A, Campo-González A, Díaz-Aguilar R. Costo-beneficio en una unidad de cuidados intensivos neonatales. Rev Cubana Pediatr. 2011;83:166-72.
Lassi ZS, Bhutta ZA. Community-based intervention packages for reducing maternal and neonatal morbidity and mortality and improving neonatal outcomes. Cochrane Database Syst Rev. 2015;3:CD007754. https://doi.org/10.1002/14651858.CD007754.pub3
Nkonki LL, Chola LL, Tugendhaft AA, Hofman KK. Modelling the cost of community interventions to reduce child mortality in South Africa using the Lives Saved Tool (LiST). BMJ Open. 2017;7:e011425. https://doi.org/10.1136/bmjopen-2016-011425
Mangham-Jefferies L, Pitt C, Cousens S, Mills A, Schellenberg J. Cost-effectiveness of strategies to improve the utilization and provision of maternal and newborn health care in low-income and lower-middle-income countries: A systematic review. BMC Pregnancy Childbirth. 2014;14:243. https://doi.org/10.1186/1471-2393-14-243
Bhutta ZA, Das JK, Bahl R, Lawn JE, Salam RA, Paul VK, et al. Can available interventions end preventable deaths in mothers, newborn babies, and stillbirths, and at what cost? Lancet. 2014;384:347-70. https://doi.org/10.1016/S0140-6736(14)60792-3
Ranjeva SL, Warf BC, Schiff SJ. Economic burden of neonatal sepsis in sub-Saharan Africa. BMJ Glob Health. 2018;3:e000347. https://doi.org/10.1136/bmjgh-2017-000347
Some similar items:
- Juan Sebastián Peinado-Acevedo, Estephanía Chacón-Valenzuela, Laura Liliana Rodríguez-Moncada, Bronze baby syndrome, an unpredictable complication of phototherapy: A case report , Biomedica: Vol. 38 No. Sup.1 (2018): Suplemento 1, Enfermedades crónicas
- Roxana De las Salas, Daniela Díaz-Agudelo, Adverse drug reactions in neonates hospitalized in neonatal intensive care units in Barranquilla, Colombia , Biomedica: Vol. 37 No. Sup.1 (2017): Suplemento 1, Alteraciones del sistema nervioso
- Juan Gabriel Piñeros, Margarita Arboleda, Juan Camilo Jaramillo, Silvia Blair, Report of five cases of severe neonatal Plasmodium vivax malaria in Urabá, Colombia , Biomedica: Vol. 28 No. 4 (2008)
- Yolanda Cifuentes, Martha Isabel Murcia, Jorge Piar, Patricia Pardo, Cerebral microcalcifications in a newborn with congenital tuberculosis , Biomedica: Vol. 36 No. 1 (2016)
- Luis Miguel Sosa, Luz Libia Cala, Julio César Mantilla, Congenital tuberculosis associated with maternal disseminated miliary tuberculosis , Biomedica: Vol. 27 No. 4 (2007)
- Eliana Patricia Calvo, Carolina Coronel-Ruiz, Syrley Velazco, Myriam Velandia-Romero, Jaime E. Castellanos, Dengue and Chikungunya differential diagnosis in pediatric patients , Biomedica: Vol. 36 (2016): Suplemento 2, Enfermedades virales
- Claudia Marcela Muñoz, José Orlando Castillo, Daniela Salas, Milena Alexandra Valderrama, Claudia Teresa Rangel, Heiddy Patricia Vargas, Diana Carolina Silva, Atypical mucocutaneous manifestations in neonates and infants with chikungunya fever in the municipalities of Cúcuta, Los Patios and Villa del Rosario, Norte de Santander, Colombia, 2014 , Biomedica: Vol. 36 No. 3 (2016)
- Husein Husein-El Ahmed, Guillermo Arturo Cañadas-De la Fuente, Rafael Fernández-Castillo, Emilio González-Jiménez, Jesús Cantero-Hinojosa, Marita Lardón-Fernández, Generalized cutaneous candidiasis in newborn at term , Biomedica: Vol. 32 No. 2 (2012)
- Luis Alfonso Pérez, Diana Marcela González, Karen Margarita de Jesús Álvarez, Luis Alfonso Díaz-Martínez, Nasal CPAP versus mechanical ventilation in 28 to 32-week preterm infants with early surfactant administration , Biomedica: Vol. 34 No. 4 (2014)
- Doris Martha Salgado, Jairo Antonio Rodríguez, Liliana del Pilar Lozano, Tatiana Esther Zabaleta, Perinatal dengue , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























