Síntesis de nanopartículas de ácido poli-láctico cargadas con antibióticos y su actividad antibacteriana contra Escherichia coli O157:H7 y Staphylococcus aureus resistente a meticilina
Resumen
Introducción. Las nanopartículas poliméricas constituyen una herramienta nanotecnológica que podría ayudar a combatir los microorganismos patógenos que han desarrollado resistencia a los antibióticos convencionales.
Objetivo. Sintetizar nanopartículas de ácido poliláctico cargadas con ofloxacina y vancomicina, y determinar su actividad antibacteriana frente a Escherichia coli O157:H7 y Staphylococcus aureus resistente a la meticilina (SARM).
Materiales y métodos. Las nanopartículas de ácido poliláctico cargadas con ofloxacina y vancomicina se sintetizaron utilizando el método de emulsión y evaporación de solvente. Se caracterizaron mediante dispersión de luz en modo dinámico, electroforesis Doppler con láser y microscopía electrónica de barrido (S-TEM). Se evaluó la actividad antibacteriana in vitro de las nanopartículas de ácido poliláctico con ofloxacina contra E. coli O157:H7 y nanopartículas de ácido poliláctico con vancomicina contra SARM, mediante el método de microdilución en caldo.
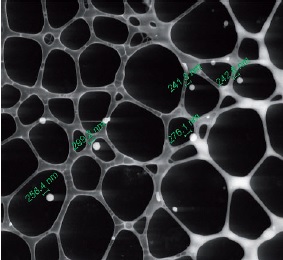
Resultados. Se obtuvieron nanopartículas poliméricas con tamaños inferiores a 379 nm y carga superficial positiva de hasta 21 mV. Las nanopartículas cargadas con ofloxacina presentaron una concentración inhibitoria mínima (CIM50) de 0,001 μg/ml frente a E. coli O157:H7, valor 40 veces menor que la concentración de antibiótico libre necesaria para lograr el mismo efecto (CIM50=0,04 μg/ml). Para SARM, las nanopartículas mejoraron la potencia farmacológica in vitro de la vancomicina al
exhibir una MIC50 de 0,005 μg/ml, comparada con la de 0,5 μg/ml del antibiótico libre.
Conclusiones. Se mejoró el efecto antibacteriano de la ofloxacina y la vancomicina incorporadas en la matriz polimérica de ácido poliláctico. Las nanopartículas poliméricas constituirían una alternativa para el control de cepas bacterianas de interés en salud pública.
Descargas
Referencias bibliográficas
Turos E, Reddy GS, Greenhalgh K, Ramaraju P, Abeylath SC, Jang S, et al. Penicillin-bound polyacrylate nanoparticles: Restoring the activity of β-lactam antibiotics against MRSA. Bioorg Med Chem. 2007;17:3468-72. http://dx.doi.org/10.1016/j.bmcl.2007.03.077
Sharpe JN, Shively EH, Polk HC. Clinical and economic outcomes of oral linezolid versus intravenous vancomycin in the treatment of MRSA-complicated, lower-extremity skin and soft-tissue infections caused by methicillin-resistant Staphylococcus aureus. Am J Surg. 2005;189:425-8. http://dx.doi.org/10.1016/j.amjsurg.2005.01.011
Wong C, Jelacic S, Habeeb R, Watkins S, Tarr P. The risk of the hemolytic–uremic syndrome after antibiotic treatment of Escherichia coli O157:H7 infections. N Engl J Med. 2000;342:1930-6. http://dx.doi.org/10.1056/NEJM200006293422601
Besser RE, Griffin PM, Slutsker L. Escherichia coli O157:H7 gastroenteritis and the hemolytic uremic syndrome: An emerging infectious disease. Annu Rev Med. 1999;50:355-67. http://dx.doi.org/10.1146/annurev.med.50.1.355
Ateba CN, Mbewe M. Detection of Escherichia coli O157:H7 virulence genes in isolates from beef, pork, water, human and animal species in the northwest province, South Africa: Public health implications. Res Microbiol. 2011;162:240-8. http://dx.doi.org/10.1146/annurev.med.50.1.355
Doyle MP. Escherichia coli O157:H7 and its significance in foods. Int J Food Microbiol. 1991;12:289-301. http://dx.doi.org/10.1016/0168-1605(91)90143-D
Thomas KM, McCann MS, Collery MM, Logan A, Whyte P, McDowell DA, et al. Tracking verocytotoxigenic Escherichia coli O157, O26, O111, O103 and O145 in Irish cattle. Int J Food Microbiol. 2012;153:288-96. http://dx.doi.org/10.1016/j.ijfoodmicro.2011.11.012
Xavier RN, Morgan HW, McDonald IR, Withers H. Effect of long-term starvation on the survival, recovery, and carbon utilization profiles of a bovine Escherichia
coli O157: H7 isolate from New Zealand. Appl Environ Microbiol. 2014;80:4383-90. http://dx.doi.org/10.1128/AEM.00045-14
Michino H, Akari K, Minami S, Takaya S, Sakai N, Miyazaki M, et al. Massive outbreak of Escherichia coli O157:H7 infection in schoolchildren in Sakai city, Japan, associated with consumption of white radish sprouts. Am J Epidemiol. 1999;150:787-96. http://dx.doi.org/10.1093/oxfordjournals.aje.a010082
Pennington H. Escherichia coli O157. Lancet. 2010;376:1428-35. http://dx.doi.org/10.1016/S0140-6736(10)60963-4
Park S, Worobo RW, Durst RA. Escherichia coli O157:H7 as an emerging foodborne pathogen: A literature review. Crit Rev Biotechnol. 2001;21:27-48. http://dx.doi.org/10.1080/20013891081674
Piedrahíta D, Márquez T, Máttar S. Detección de Escherichia coli 0157: H7 en poblaciones porcinas, canal bovina y productos cárnicos en el departamento de Córdoba. Rev MVZ Córdoba. 2001;6:119-26.
Mora A, Blanco JE, Blanco M, Alonso MP, Dhabi G, Echeita A, et al. Antimicrobial resistance of Shiga toxin (verotoxin)-producing Escherichia coli O157:H7 and non-O157 strains isolated from humans, cattle, sheep and food in Spain. Res Microbiol. 2005;156:793-806. http://dx.doi.org/10.1016/j.resmic.2005.03.006
Boucher HW, Corey GR. Epidemiology of methicillinresistant Staphylococcus aureus. Clin Infect Dis. 2008;46 (Suppl.5):S344-9. http://dx.doi.org/10.1086/533590
Martínez E, Hernández C, Pallares C, Pacheco R, Hurtado K, Recalde M. Frecuencia de aislamientos microbiológicos y perfil de resistencia bacteriana en 13 clínicas y hospitales de alta complejidad en Santiago de Cali - Colombia. Infectio. 2014;18:3-11. http://dx.doi.org/10.1016/S0123-9392(14)70734-9
Moellering RC. MRSA: The first half century. J Antimicrob Chemother. 2012;67:4-11. http://dx.doi.org/10.1093/jac/dkr437
Normanno G, Corrente M, La Salandra G, Dambrosio A, Quaglia NC, Parisi A, et al. Methicillin-resistant Staphylococcus aureus (MRSA) in foods of animal origin product in Italy. Int J Food Microbiol. 2007;117:219-22. http://dx.doi.org/10.1016/j.ijfoodmicro.2007.04.006
Shopsin B, Kreiswirth BN. Molecular epidemiology of methicillin-resistant Staphylococcus aureus. Emerg Infect Dis. 2001;7:323-6.
Guzmán-Blanco M, Mejía C, Isturiz R, Álvarez C, Bavestrello L, Gotuzzo E, et al. Epidemiology of meticillinresistant Staphylococcus aureus (MRSA) in Latin America. Int J Antimicrob Agents. 2009;34:304-8. http://dx.doi.org/10.1016/j.ijantimicag.2009.06.005
González L, Cortés JA. Revisión sistemática de la farmacorresistencia en enterobacterias de aislamientos hospitalarios en Colombia. Biomédica. 2014;34:180-97. http://dx.doi.org/10.7705/biomedica.v34i2.1550
Machuca MA, González CI, Sosa LM. Methicillinresistant Staphylococcus aureus causes both community associated and health care-associated infections in children at the Hospital Universitario de Santander. Biomédica. 2014;34(Suppl.1):163-9. http://dx.doi.org/10.7705/biomedica.v34i0.1648
Gemmell CG, Edwards DI, Fraise AP, Gould FK, Ridgway GL, Warren RE. Guidelines for the prophylaxis and treatment of methicillin-resistant Staphylococcus aureus (MRSA) infections in the UK. J Antimicrob Chemother. 2006;57:589-608. http://dx.doi.org/10.1093/jac/dkl017
Schroeder CM, Zhao C, Debroy C, Torcolini J, Zhao S, White DG, et al. Antimicrobial resistance of Escherichia coli O157 isolated from humans, cattle, swine, and food. Appl Environ Microbiol. 2002;68:576-81. http://dx.doi.org/10.1128/AEM.68.2.576
Zhang L, Pornpattananangku D, Hu C-MJ, Huang C-M. Development of nanoparticles for antimicrobial drug delivery. Curr Med Chem. 2010;17:585-94. http://dx.doi.org/10.2174/092986710790416290
Radovic-Moreno AF, Lu TK, Puscasu VA, Yoon CJ, Langer R, Farokhzad OC. Surface charge-switching polymeric nanoparticles for bacterial cell wall-targeted delivery of antibiotics. ACS Nano. 2012;6:4279-87. http://dx.doi.org/10.1021/nn3008383
Soppimath K, Aminabhavi, Rudzinski WE T, Kulkarni AR. Biodegradable polymeric nanoparticles as drug delivery devices. J Control Release. 2001;70:1-20. http://dx.doi.org/10.1016/S0168-3659(00)00339-4
Kumari A, Yadav SK, Yadav SC. Biodegradable polymeric nanoparticles based drug delivery systems. Colloids Surf B Biointerfaces. 2010;75:1-18. http://dx.doi.org/10.1016/j.colsurfb.2009.09.001
Reinert RR, Low DE, Rossi F, Zhang X, Wattal C, Dowzicky MJ. Antimicrobial susceptibility among organisms from the Asia/Pacific Rim, Europe and Latin and North America collected as part of TEST and the in vitro activity of tigecycline. J Antimicrob Chemother. 2007;60:1018-29. http://dx.doi.org/10.1093/jac/dkm310
Jeffery H, Davis SS, O’Hagan DT. The preparation and characterisation of poly(lactide-co-glycolide) microparticles. I: Oil-in-water emulsion solvent evaporation. Int J Pharm. 1991;77:169-75. http://dx.doi.org/10.1016/0378-5173(91)90314-E
Jones DS, Pearce KJ. Contribution of process variables to the entrapment efficiency of propranolol hydrochloride within ethylcellulose microspheres prepared by the solvent evaporation method as evaluated using a factorial design. Int J Pharm. 1996;131:25-31. http://dx.doi.org/10.1016/0378-5173(95)04298-9
Rosca ID, Watari F, Uo M. Microparticle formation and its mechanism in single and double emulsion solvent evaporation. J Control Release. 2004;99:271-80. http://dx.doi.org/10.1016/j.jconrel.2004.07.007
Loveymi BD, Jelvehgari M, Zakeri-Milani P, Valizadeh H. Statistical optimization of oral vancomycin-eudragit rs nanoparticles using response surface methodology. Iran J Pharm Res. 2012;11:1001-12.
Lotfipour F, Abdollahi S, Jelvehgari M, Valizadeh H, Hassan M, MIlani M. Study of antimicrobial effects of vancomycin loaded PLGA nanoparticles against enterococcus clinical isolates. Drug Res (Stuttg). 2014;64:348-52. http://dx.doi.org/10.1055/s-0033-1358747
Yang YY, Chia HH, Chung TS. Effect of preparation temperature on the characteristics and release profiles of PLGA microspheres containing protein fabricated by double-emulsion solvent extraction/evaporation method. J Control Release. 2000;69:81-96. http://dx.doi.org/10.1016/S0168-3659(00)00291-1
Yang YY, Chung TS, Ng NP. Morphology, drug distribution, and in vitro release profiles of biodegradable polymeric microspheres containing protein fabricated by doubleemulsion solvent extraction/evaporation method. Biomaterials. 2001;22:231-41. http://dx.doi.org/10.1016/S0142-9612(00)00178-2
Martínez-Gutiérrez F, Olive PL, Bañuelos A, Orrantía E, Niño N, Sánchez EM, et al. Synthesis, characterization, and evaluation of antimicrobial and cytotoxic effect of silver and titanium nanoparticles. Nanomedicine. 2010;6:681-8. http://dx.doi.org/10.1016/j.nano.2010.02.001
Paredes-Guerrero DJ. Estudio del efecto antibacteriano de nanopartículas de plata sobre Escherichia coli y Staphylococcus aureus (tesis). Bucaramanga: Universidad Industrial de Santander; 2011. p. 1-99.
Abazinge M, Jackson T, Yang Q, Owusu-Ababio G. Comparison of in vitro and in vivo release characteristics of sustained release ofloxacin microspheres. Drug Deliv. 2000;7:77-81. http://dx.doi.org/10.1080/107175400266632
Hans ML, Lowman AM. Biodegradable nanoparticles for drug delivery and targeting. Curr Opin Solid State Mater Sci. 2002;6:319-27. http://dx.doi.org/10.1016/S1359-0286(02)00117-1
Li M, Rouaud O, Poncelet D. Microencapsulation by solvent evaporation: State of the art for process engineering approaches. Int J Pharm. 2008;363:26-39. http://dx.doi.org/10.1016/j.ijpharm.2008.07.018
Wischke C, Schwendeman SP. Principles of encapsulating hydrophobic drugs in PLA/PLGA microparticles. Int J Pharm. 2008;364:298-327. http://dx.doi.org/10.1016/j.ijpharm.2008.04.042
Quintanar-Guerrero D, Fessi H, Allémann E, Doelker E. Influence of stabilizing agents and preparative variables on the formation of poly(D,L-lactic acid) nanoparticles by an emulsification-diffusion technique. Int J Pharm. 1996;143:133-41. http://dx.doi.org/10.1016/S0378-5173(96) 04697-2
Desgouilles S, Vauthier C, Bazile D, Vacus J, Grossiord JL, Veillard M, et al. The design of nanoparticles obtained by solvent evaporation: A comprehensive study. Langmuir. 2003;19:9504-10. http://dx.doi.org/10.1021/la034999q
Vauthier C, Bouchemal K. Methods for the preparation and manufacture of polymeric nanoparticles. Pharm Res. 2009;26:1025-58. http://dx.doi.org/10.1007/s11095-008-9800-3
Redhead HM, Davis SS, Illum L. Drug delivery in poly (lactide-co-glycolide) nanoparticles surface modified with poloxamer 407 and poloxamine 908: In vitro characterisation and in vivo evaluation. J Control Release. 2001;70:353-63.http://dx.doi.org/10.1016/S0168-3659(00)00367-9
Cheng YH, Illum L, Davis SS. A poly(D,L-lactide-coglycolide) microsphere depot system for delivery of haloperidol. J Control Release. 1998;55:203-12. http://dx.doi.org/10.1016/S0168-3659(98)00056-X
Hermans K, van Den Plas D, Everaert A, Weyenberg W, Ludwig A. Full factorial design, physicochemical characterisation and biological assessment of cyclosporine A loaded cationic nanoparticles. Eur J Pharm Biopharm. 2012;82:27-35. http://dx.doi.org/10.1016/j.ejpb.2012.05.003
Cheow WS, Hadinoto K. Factors affecting drug encapsulation and stability of lipid-polymer hybrid nanoparticles. Colloids Surf B Biointerfaces. 2011;85:214-20. http://dx.doi.org/10.1016/j.colsurfb.2011.02.033
Moghimi SM, Hunter AC. Poloxamers and poloxamines in nanoparticle engineering and experimental medicine. Trends Biotechnol. 2000;18:412-20. http://dx.doi.org/10.1016/S0167-7799(00)01485-2
Hachicha W, Kodjikian L, Fessi H. Preparation of vancomycin microparticles: Importance of preparation parameters. Int J Pharm. 2006;324:176-84. http://dx.doi.org/10.1016/j.ijpharm.2006.06.005
Schugens C, Laruelle N, Nihant N, Grandfils C, Jkrome R, Teyssi P. Effect of the emulsion stability on the morphology and porosity of semicrystalline poly I-lactide microparticles prepared by w/o/w double emulsion-evaporation. J Control Release. 1994;32:161-76. http://dx.doi.org/10.1016/0168-3659(94)90055-8
Makadia HK, Siegel SJ. Poly Lactic-co-Glycolic Acid (PLGA) as biodegradable controlled drug delivery carrier. Polymers (Basel). 2011;3:1377-97. http://dx.doi.org/10.3390/polym3031377
Mora-Huertas CE, Fessi H, Elaissari A. Polymer-based nanocapsules for drug delivery. Int J Pharm. 2010;385:113-42. http://dx.doi.org/10.1016/j.ijpharm.2009.10.018
Jalil R, Nixonts JR. Review biodegradable poly (lactic acid) and poly (1actide-co-glycolide) microcapsules: Problems associated with preparative techniques and release properties. Microencapsulation. 1990;7:297-325. http://dx.doi.org/10.3109/02652049009021842
Hombreiro M, Zinutti C, Lamprecht A, Ubrich N, Astier A, Hoffman M, et al. The preparation and evaluation of poly(ε-caprolactone) microparticles containing both a lipophilic and a hydrophilic drug. J Control Release. 2000;65:429-38.http://dx.doi.org/10.1016/S0168-3659(99)00253-9
Vrignaud S, Benoit JP, Saulnier P. Strategies for the nanoencapsulation of hydrophilic molecules in polymerbased nanoparticles. Biomaterials. 2011;32:8593-604. http://dx.doi.org/10.1016/j.biomaterials.2011.07.057
Panyam J, William D, Dash A, Leslie-Pelecky D, Labhasetwar V. Solid-state solubility influences encapsulation and release of hydrophobic drugs from PLGA/PLA nanoparticles. J Pharm Sci. 2004;93:1804-14. http://dx.doi.org/10.1002/jps.20094
Mohanraj VJ, Chen Y. Nanoparticles - A review. Trop J Pharm Res. 2007;5:561-73. http://dx.doi.org/10.4314/tjpr.v5i1.14634
Kim IS, Lee SK, Park YM, Lee YB, Shin SC, Lee KC, et al. Physicochemical characterization of poly(l-lactic acid) and poly(d,l-lactide-co-glycolide) nanoparticles with polyethylenimine as gene delivery carrier. Int J Pharm.2005;298:255-62. http://dx.doi.org/10.1016/j.ijpharm.2005.04.017
Okeri HA, Arhewoh IM. Analytical profile of the fluoroquinolone antibacterials. African J Biotechnol. 2008;7:670-80. http://dx.doi.org/10.5897/AJB07.174
Allahverdiyev AM, Kon KV, Abamor ES, Bagirova M, Rafailovich M. Coping with antibiotic resistance: Combining nanoparticles with antibiotics and other antimicrobial agents. Expert Rev Anti Infect Ther. 2011;9:1035-52. http://dx.doi.org/10.1586/eri.11.121
Puglisi G, Fresta M, Mazzone G, Furneri PM, Tempera G. Formulation parameters of fluoroquinolone-loaded liposomes and in vitro antimicrobial activity. Int J Pharm. 1995;118:65-76. http://dx.doi.org/10.1016/0378-5173(94)00340-B
Jeong Y Il, Na HS, Seo DH, Kim DG, Lee HC, Jang MK, et al. Ciprofloxacin-encapsulated poly(dl-lactide-co-glycolide) nanoparticles and its antibacterial activity. Int J Pharm.2008;352:317-23. http://dx.doi.org/10.1016/j.ijpharm.2007.11.001
Fresta M, Puglisi G, Giammona G, Cavallaro G, Micali N, Furneri PM. Pefloxacine mesilate- and ofloxacin-loaded polyethylcyanoacrylate nanoparticles: Characterization of the colloidal drug carrier formulation. J Pharm Sci. 1995;84:895-902. http://dx.doi.org/10.1002/jps.2600840721
Chakraborty SP, Sahu SK, Mahapatra SK, Santra S, Bal M, Roy S, et al. Nanoconjugated vancomycin: New opportunities for the development of anti-VRSA agents. Nanotechnology. 2010;21:105103. http://dx.doi.org/10.1088/0957-4484/21/10/105103
Lai H-Z, Chen W-Y, Wu C-Y, Chen Y-C. Potent antibacterial nanoparticles for pathogenic bacteria. ACS Appl Mater Interfaces. 2015;73:2046-54. http://dx.doi.org/10.1021/am507919m
Liu P-F, Lo C-W, Chen C-H, Hsieh M-F, Huang C-M. Use of nanoparticles as therapy for methicillin-resistant Staphylococcus aureus infections. Curr Drug Metab. 2009;10:875-84. http://dx.doi.org/10.2174/138920009790274522
Panyam J, Labhasetwar V. Biodegradable nanoparticles for drug and gene delivery to cells and tissue. Adv Drug Deliv Rev. 2003;55:329-47. http://dx.doi.org/10.1016/S0169-409X(02)00228-4
Xie S, Tao Y, Pan Y, Qu W, Cheng G, Huang L, et al. Biodegradable nanoparticles for intracellular delivery of antimicrobial agents. J Control Release. 2014;187:101-17. http://dx.doi.org/10.1016/j.jconrel.2014.05.034
Algunos artículos similares:
- Carmelo José Espinosa, Jorge Alberto Cortés, Juan Sebastián Castillo, Aura Lucía Leal, Revisión sistemática de la resistencia antimicrobiana en cocos Gram positivos intrahospitalarios en Colombia , Biomédica: Vol. 31 Núm. 1 (2011)
- Andrés Leonardo González, Aura Lucía Leal, Jorge Alberto Cortés, Ricardo Sánchez, Liliana Isabel Barrero, Juan Sebastián Castillo, Carlos Arturo Álvarez, Efecto del tratamiento antibiótico inicial adecuado sobre la mortalidad en pacientes en estado crítico con bacteriemia por Pseudomonas aeruginosa , Biomédica: Vol. 34 (2014): Abril, Suplemento 1, Resistencia bacteriana
- Virgilio Galvis, Alejandro Tello, Alfredo Guerra, María Fernanda Acuña, Donaldo Villarreal, Sensibilidad antibiótica de bacterias obtenidas de queratitis e infecciones intraoculares en la Fundación Oftalmológica de Santander (FOSCAL), Floridablanca, Colombia , Biomédica: Vol. 34 (2014): Abril, Suplemento 1, Resistencia bacteriana
- Marlen Cháves, Caracterización de reacciones adversas a medicamentos en adultos mayores de 44 años en Bogotá, D.C., enero a diciembre, 2012 , Biomédica: Vol. 35 Núm. 1 (2015)
- Christian José Pallares, Ernesto Martínez, Factores de riesgo asociados a mortalidad en infecciones relacionadas con la atención en salud en un hospital universitario de tercer nivel en Colombia , Biomédica: Vol. 34 (2014): Abril, Suplemento 1, Resistencia bacteriana
- Adriana Jiménez, Alejandra Alvarado, Felipe Gómez, Germán Carrero, Claudia Fajardo, Factores de riesgo asociados al aislamiento de Escherichia coli o Klebsiella pneumoniae productoras de betalactamasas de espectro extendido en un hospital de cuarto nivel en Colombia , Biomédica: Vol. 34 (2014): Abril, Suplemento 1, Resistencia bacteriana
- Manuel Medell, Marcia Hart, María Luisa Batista, Sensibilidad antimicrobiana in vitro en aislamientos de Enterococcus faecalis y Enterococcus faecium obtenidos de pacientes hospitalizados , Biomédica: Vol. 34 (2014): Abril, Suplemento 1, Resistencia bacteriana
- Katerina Klímová, Camilo Padilla, Juan Carlos Ávila, Gerardo Clemente, Alejandra Ochoa, Epidemiología de las infecciones bacterianas en pacientes con cirrosis hepática, experiencia de un centro español de atención terciaria , Biomédica: Vol. 36 Núm. 1 (2016)
- Mónica Alejandra Bernal-Vargas, Jorge Alberto Cortés, Ricardo Sánchez, Adaptación transcultural del cuestionario de puntuación de la neumonía adquirida en la comunidad en pacientes con neumonía leve a moderada en Colombia , Biomédica: Vol. 37 Núm. 1 (2017)
- Carlos Carvajal, Carlos Pacheco, Fabián Jaimes, Perfil clínico y demográfico y factores de riesgo frente a la infección por Clostridium difficile , Biomédica: Vol. 37 Núm. 1 (2017)
| Estadísticas de artículo | |
|---|---|
| Vistas de resúmenes | |
| Vistas de PDF | |
| Descargas de PDF | |
| Vistas de HTML | |
| Otras vistas | |

























