Leishmaniasis cutánea y embarazo
Resumen
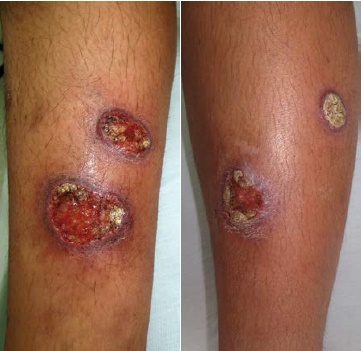
Se estudió a una mujer de 19 años, con embarazo de cuatro meses, que presentaba cuatro úlceras cutáneas de tres meses de evolución, diagnosticadas por biopsia como leishmaniasis cutánea. El frotis directo y la leishmanina fueron negativos.
Dado que todos los medicamentos usuales para la leishmaniasis cutánea están contraindicados en el embarazo, la paciente no recibió tratamiento, aunque curó espontáneamente durante el embarazo. Se cree que la leishmaniasis cutánea no tiene peligro para la mujer embarazada y que no hay transmisión de la madre al feto en el humano, aunque se ha detectado en animales en condiciones experimentales.
La paciente tuvo un parto sin complicaciones y la condición de salud tanto de ella como de su hijo era normal a los dos años de seguimiento.
Descargas
Referencias bibliográficas
Rodríguez G, Arenas C, Ovalle C, Hernández CA, Camargo C. Las leishmaniasis. Atlas y texto. Bogotá: Centro Dermatológico Federico Lleras Acosta; 2016.
Organización Panamericana de la Salud - Organización Mundial de la Salud. Informe Leishmaniasis No 4, julio 2016. Ginebra; OPS: 2016.
Instituto Nacional de Salud. Boletín Epidemiológico Semanal. Semana epidemiológica número 52 de 2016. 25 de diciembre - 31 de diciembre, 2016. Bogotá: Instituto Nacional de Salud; 2016. Fecha de consulta: 14 de julio de 2017. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2016%20Bolet%C3%ADn%20
epidemiol%C3%B3gico%20semana%2052%20-.pdf
Vélez ID, Hendrickx E, Robledo SM, Agudelo SM. Leishmaniosis cutánea en Colombia y género. Cad Saúde Pública. 2001;17:171-81. https://doi.org/10.1590/S0102-311X2001000100018
Morgan DJ, Guimaraes LH, Machado PR, D´Oliveira Jr A, Almeida RP, Lago EL, et al. Cutaneous leishmaniasis during pregnancy: Exhuberant lesions and potential fetal complications. Clin Infect Dis. 2007;45:478-82. https://doi.org/10.1086/520017
Conceicao-Silva F, Morgado FN, Pimentel FM, Vasconcellos EC, Schubach AO, Valete-Roselino CM, et al. Two women presenting worsening cutaneous ulcers during pregnancy: Diagnosis, immune response, and follow-up. PLoS Negl Trop Dis. 2013;7:e2472. https://doi.org/10.1371/journal.pntd.0002472
Berger BA, Bartlett AH, Saravia NG, Galindo SN. Pathophysiology of Leishmania infection during pregnancy. Trends Parasitol. 2017;33:935-46. https://doi.org/10.1016/j.pt.2017.08.012
Ávila-García M, Mancilla-Ramírez J, Segura-Cervantes E, Farfán-Labone B, Ramírez-Ramírez A, Sevilla-Galindo N. Transplacental transmission of cutaneous Leishmania mexicana strain in BALB/c mice. Am J Trop Med Hyg. 2013;89:354-8. https://doi.org/10.4269/ajtmh.12-0716
Osorio Y, Rodríguez LD, Bonilla Dl, Peniche AG, Henao H, Saldarriaga O, et al. Congenital transmission of experimental leishmaniasis in a hamster model. Am J Trop Med Hyg. 2012;86:812-20. https://doi.org/10.4269/ajtmh.2012.11-0458
Rodríguez-Barraquer I, Góngora R, Prager M, Pacheco R, Montero LM, Navas A, et al. Etiologic agent of an epidemic of cutaneous leishmaniasis in Tolima, Colombia. Am J Trop Med Hyg 2008;78:276-82.
Pagliano P, Carannante N, Rossi M, Gramiccia M, Gradoni L, Faella FS, et al. Visceral leishmaniasis in pregnancy: A case series and a systematic review of the literature. J Antimicrobial Chem. 2005;55:229-33. https://doi.org/10.1093/jac/dkh538
Turine-Neto P, Figueiró-Fihlo E, Oliveira V, Coehlo L, Breda I, Melo L, et al. Visceral leishmaniasis and pregnancy: A retrospective study of cases reported in Brazil. Int J Gynecol Obstet. 2009;107(Suppl.2):S364. https://doi.org/10.1016/S0020-7292(09)61326-6
Fontenele SJ, Freire GT, Gomes PM, Tolentino SM. Treatment of American tegumentary leishmaniasis in special populations: A summary of evidence. Rev Soc Bras Med Trop. 2013;46:669-77. https://doi.org/10.1590/0037-8682-0104-2013
Layegh P, Pezeshkpoor F, Soruri AH, Naviafar P, Moghiman T. Efficacy of cryotherapy versus intralesional meglumine antimoniate (Glucantime) for treatment of cutaneous leishmaniasis in children. Am J Trop Meg Hyg. 2009;80:172-5.
Vega JC, Sánchez BF, Montero LM, Montaña R, Mahecha MP, Dueñas B, et al. The efficacy of thermotherapy to treat cutaneous leishmaniasis in Colombia. A comparative observational study in an operational setting. Trans R Soc Trop Med Hyg. 2009;103:703-6. https://doi.org/10.1016/j.trstmh.2008.10.039
López L, Robayo M, Vargas M, Vélez ID. Thermotherapy. An alternative for the treatment of American cutaneous leishmaniasis. Trials. 2012;13:58. https://doi.org/10.1186/1745-6215-13-58
Sundar S, Chakravarty J, Agarwai D, Rai M, Murray HW. Single-dose liposomal amphotericin B for visceral leishmaniasis in India. N Engl J Med 2010;362:604-12. https://doi.org/10.1056/NEJMoa0903627
Algunos artículos similares:
- Luis Miguel Sosa, Luz Libia Cala, Julio César Mantilla, Tuberculosis congénita asociada con tuberculosis materna miliar diseminada , Biomédica: Vol. 27 Núm. 4 (2007)
- Juan Gabriel Piñeros, Malaria y determinantes sociales de la salud: un nuevo marco heurístico desde la medicina social latinoamericana , Biomédica: Vol. 30 Núm. 2 (2010)
- Rafael José Vivero, Maria Angélica Contreras-Gutiérrez, Eduar Elías Bejarano, Análisis de la estructura primaria y secundaria del ARN de transferencia mitocondrial para serina en siete especies de Lutzomyia , Biomédica: Vol. 27 Núm. 3 (2007)
- Elsa Nieves, Neudo Buelvas, Maritza Rondón, Néstor González, Las glándulas salivales de dos flebotominos vectores de Leishmania: Lutzomyia migonei (França) y Lutzomyia ovallesi (Ortiz) (Diptera: Psychodidae) , Biomédica: Vol. 30 Núm. 3 (2010)
- Carlos Pérez, Yoanet Solías, Gerzaín Rodríguez, Leishmaniasis cutánea difusa en un paciente con sida , Biomédica: Vol. 26 Núm. 4 (2006)
- María Angélica Contreras, Rafael José Vivero, Eduar Elías Bejarano, Lina María Carrillo, Iván Darío Vélez, Nuevos registros de flebotomíneos (Diptera: Psychodidae) en el área de influencia del río Amoyá en Chaparral, Tolima , Biomédica: Vol. 32 Núm. 2 (2012)
- Luz Adriana Acosta, Karina Mondragon-Shem, Daniela Vergara, Andrés Velez-Mira, Horacio Cadena, Lina Maria Carrillo, Ampliación de la distribución de Lutzomyia longipalpis (Lutz & Neiva, 1912) (Diptera: Psychodidae) en el departamento de Caldas: potencial aumento del riesgo de leishmaniasis visceral , Biomédica: Vol. 33 Núm. 2 (2013)
- Stella Carrasco Rodríguez, Myriam Sanchez Gómez, Niveles séricos de IGF-I e IGFBP-3 en adolescentes embarazadas provenientes de un sector socioeconómico de bajos ingresos , Biomédica: Vol. 21 Núm. 4 (2001)
- Berta N. Restrepo, Diana M. Isaza, Clara L. Salazar, José L. Ramírez, Gloria E. Upegui, Marta Ospina, Ruth Ramírez, Dengue en el embarazo: efectos en el feto y el recién nacido. , Biomédica: Vol. 23 Núm. 4 (2003)
- Clemencia Ovalle-Bracho, Carolina Camargo, Yira Díaz-Toro, Marcela Parra-Muñoz, Tipificación molecular de Leishmania (Leishmania) amazonensis y especies del subgénero Viannia asociadas a la leishmaniasis cutánea y la mucosa en Colombia: un estudio de concordancia , Biomédica: Vol. 38 Núm. 1 (2018)
| Estadísticas de artículo | |
|---|---|
| Vistas de resúmenes | |
| Vistas de PDF | |
| Descargas de PDF | |
| Vistas de HTML | |
| Otras vistas | |

























