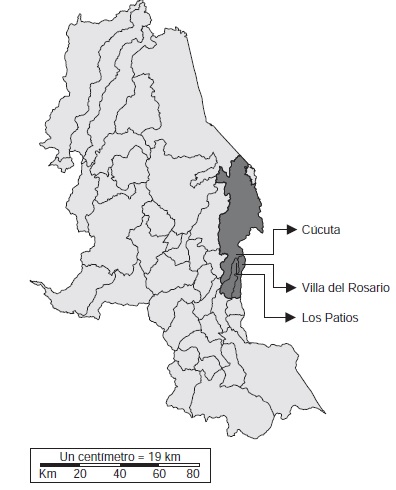
Manifestaciones mucocutáneas atípicas por fiebre por el virus del chikungunya en neonatos y lactantes de Cúcuta, Los Patios y Villa del Rosario, Norte de Santander, Colombia, 2014
Resumen
Introducción. Se han observado manifestaciones clínicas atípicas en recién nacidos y lactantes con fiebre por el virus del chikungunya. Objetivo. Describir los casos de fiebre causada por el virus del chikungunya en recién nacidos y lactantes con lesiones mucocutáneas atípicas. Materiales y métodos. Se revisaron las historias clínicas y los resultados de laboratorio y de patología en tres hospitales regionales de los casos de recién nacidos y lactantes diagnosticados con el virus del chikungunya que presentaban lesiones mucocutáneas atípicas; se hizo una búsqueda activa comunitaria en los barrios de residencia de los pacientes. Resultados. De 18 casos sospechosos de chikungunya en recién nacidos y lactantes, 11 pacientes con diagnóstico confirmado presentaron manifestaciones mucocutáneas atípicas. Seis de los 11 casos confirmados eran niños menores de cinco meses de edad. Los síntomas más frecuentes fueron: fiebre, eritema, irritabilidad y diarrea. Tres de los pacientes estaban infectados con dengue y chikungunya. Las úlceras se presentaron en cuero cabelludo, abdomen, región genital y perianal. En la búsqueda activa comunitaria se encontraron altas tasas de ataque de la enfermedad. Conclusiones. Se presenta un informe de las manifestaciones mucocutáneas en recién nacidos y lactantes diagnosticados con fiebre por el virus del chikungunya en Colombia. El rápido desarrollo de las úlceras se debe, probablemente, a la reacción inmunitaria al virus. Es necesario priorizar la atención de las mujeres embarazadas que presenten síntomas una semana antes del parto y hacerle seguimiento a los recién nacidos, para hacer el diagnóstico temprano del chikungunya y evitar complicaciones.
Descargas
Referencias bibliográficas
Morrison T. Reemergence of Chikungunya virus. J Virol. 2014;88:11644-7. http://dx.doi.org/10.1128/JVI.01432-14
Rezza G, Nicoletti L, Angelini R, Romi R, Finarelli AC, Panning M, et al. Infection with Chikungunya virus in Italy: An outbreak in a temperate region. Lancet. 2007;370:1840-6. http://dx.doi.org/10.1016/S0140-6736(07) 61779-6
Gérardin P, Barau G, Michault A, Bintner M, Randrianaivo H, Choker G, et al. Multidisciplinary prospective study of mother-to-child Chikungunya virus infections on the Island of La Réunion. PLoS Med 2008;5:e60. http://dx.doi.org/10.1371/journal.pmed.0050060
Moro M, Gagliotti C, Silvi G, Angelini R, Sambri V, Rezza G, et al. Chikungunya virus in North-Eastern Italy: A seroprevalence survey. Am J Trop Med Hyg. 2010;82:508-11. http://dx.doi.org/10.4269/ajtmh.2010.09-0322
Diallo M, Thonnon J, Traore-Lamizana M, Fontenille D. Vectors of Chikungunya virus in Senegal: Current data and transmission cycles. Am J Trop Med Hyg. 1999;60:281-6.
Thiberville SD, Moyen N, Dupuis-Maguiraga L, Nougairede A, Gould EA, Roques P, et al. Chikungunya fever: Epidemiology, clinical syndrome, pathogenesis and therapy. Antiviral Res. 2013;99:345-70. http://dx.doi.org/10.1016/j.antiviral.2013.06.009
Pialoux G, Gaüzère B, Jauréguiberry S, Strobel M. Chikungunya, an epidemic arbovirosis. Lancet Infect Dis. 2007;7:319-27. http://dx.doi.org/10.1016/S1473-3099(07) 70107-X
Organización Panamericana de Salud. Preparación y res-puesta ante la eventual introducción del virus Chikungunya en las Américas. Washington, D.C.: OMS; 2011. Fecha de consulta: 20 de enero de 2015. Disponible en: http://www1.paho.org/hq/dmdocuments/CHIKV_Spanish.pdf.
Pimentel R, Skewes-Ramm, Moya J. Chikungunya en la República Dominicana: lecciones aprendidas en los primeros seis meses. Rev Panam Salud Pública. 2014;36:336-41.
Pialoux G, Gaüzère B, Strobel M. Infection à virus Chikungunya: revue générale par temps d´épidémie. Med Mal Infect. 2006;36:253-63. http://dx.doi.org/10.1016/j.medmal.2006.04.002
Ramesh M, Yashaswi R, Amith R, Nandakishore B, Sukumar D, Martis J, et al. Mucocutaneous manifestations of Chikungunya fever: A study from an epidemic in coastal Karnataka. Indian J Dermatol. 2011;56:290-4. http://dx.doi.org/10.4103/0019-5154.82483
Economopoulou A, Domínguez M, Helynck B, Sissoko D, Wichmann O, Quenel P, et al. Atypical Chikungunya virus infections: Clinical manifestations, mortality and risk factors for severe disease during the 2005–2006 outbreak on Reunion. Epidemiol Infect. 2009;137:534-41. http://dx.doi.org/10.1017/S0950268808001167
Robin S, Ramful D, Zettor J, Benhamou L, Jaffar M, Rivière J, et al. Severe bullous skin lesions associated with Chikungunya virus infection in small infants. Eur J Pediatr. 2010;169:67-72. http://dx.doi.org/10.1007/s00431-009-0986-0
Organización Mundial de la Salud. Chikungunya. Fecha de consulta: 20 de enero de 2015. Disponible en: http://www.who.int/mediacentre/factsheets/fs327/es/.
Organización Panamericana de la Salud. Número de casos reportados de Chikungunya en países o territorios de las Américas 2013-2014. Semana epidemiológica 51 de 2014. Fecha de consulta: 20 de enero de 2015. Disponible en: http://www.paho.org/hq/index.php?option=com_topics&view=readall&cid=5932&Itemid=40931&lang=es.
Instituto Nacional de Salud. Boletín Epidemiológico Nacional, Semana Epidemiológica 51 de 2014. Bogotá: Instituto Nacional de Salud; 2014. Fecha de consulta: 20 de enero de 2015. Disponible en: http://www.ins.gov.co/boletin-epidemiologico/Boletn%20Epidemiolgico/2014%20Boletin%20epidemiologico%20semana%2051.pdf.
Martínez M, Gómez S. Chikungunya en Colombia, el inicio de la transmisión autóctona, 2014. Inf Quinc Epidemiol Nac. 2014;19:260-79. Fecha de consulta: 21 de enero de 2015. Disponible en: http://www.ins.gov.co/iqen/IQUEN/IQEN%20vol%2019%202014%20num%2018.pdf.
Instituto Nacional de Salud. Lineamientos de vigilancia en salud pública, entomológica y de laboratorio en transmisión autóctona del virus chikungunya en Colombia. Fase II. Bogotá: Instituto Nacional de Salud; 2014. Fecha de consulta: 21 de enero de 2015. Disponible en: http://www.ins.gov.co/Noticias/Chikungunya/Lineamientos%20de%20vigilancia%20chikungunya%202014.pdf.
Alcaldía Municipal de Los Patios. Plan de Desarrollo - Municipio de Los Patios, 2012-2015. Los Patios: Alcaldía; 2012. Fecha de consulta: 21 de enero de 2015. Disponible en: http://cdim.esap.edu.co/BancoMedios/Documentos%20PDF/lospatiosnortedesantanderpd20122015.pdf.
Alcaldía Municipal de Villa del Rosario. Plan de Desarrollo - Municipio de Villa de Rosario, 2012-2015. Villa del Rosario: Alcaldía; 2012. Fecha de consulta: 21 de enero de 2015. Disponible en: http://www.villadelrosario-nortedesantander.gov.co/apc-aa-files/64356430383236653039663635623561/version-final-plan-desarr-documento-tecnico.pdf-
Instituto Nacional de Salud. Grupo de Enfermedades Transmitidas por Vectores. Resumen, Chikunguña a semana 53. Bogotá: Instituto Nacional de Salud; 2014. Fecha de consulta: 21 de enero de 2015. Disponible en: http://www.ins.gov.co/Noticias/Chikungunya/Forms/AllItems.aspx?Paged=TRUE&p_SortBehavior=0&p_orden=&p_ID=89&PageFirstRow=61&&View={F354C77A-609B-4AE6-8D9D-7C203FE1526F}
Institut de Veille Sanitaire. Surveillance des formes émergentes hospitalières de chikungunya, la Réunion, avril 2005 - mars 2006. Rapport détaillé. Saint Maurice, France: INVS; 2007. Fecha de consulta: 30 de agosto de 2015. Disponible en: http://www.invs.sante.fr/publications/2007/chik_surveillance_2007/chik_surveillance_2007.pdf.
Valamparampil J, Chirakkarot S, Letha S, Jayakumar C, Gopinathan K. Clinical profile of Chikungunya in infants. Indian J Pediatr. 2009;76:151-5. http://dx.doi.org/10.1007/s12098-009-0045-x
Riyaz N, Riyaz A, Rahima A, Latheef E, Anitha P, Aravindan K, et al. Cutaneous manifestations of chikungunya during a recent epidemic in Calicut, north Kerala, south India. Indian J Dermatol Venereol Leprol. 2010;76:671-6. http://dx.doi.org/10.4103/0378-6323.72466
Seetharam KA, Sridevi K, Vidyasagar P. Cutaneous manifestations of Chikungunya fever. Indian Pediatr. 2012; 49:51-3.
Inamadar A, Palit A, Sampagavi W, Raghunath S, Deshmukh N. Cutaneous manifestations of Chikungunya fever: Observations made during a recent outbreak in South India. Int J Dermatol. 2008;47:154-9. http://dx.doi.org/10.1111/j.1365-4632.2008.03478.x
Prashant S, Kumar A, Basheeruddin D, Chowdhary T, Madhu B. Cutaneous manifestations in patients suspected of Chikungunya disease. Indian J Dermatol. 2009;54:128-31. http://dx.doi.org/10.4103/0019-5154.53186
Mishra K, Rajawat V. Chikungunya-induced genital ulcers. Indian J Dermatol Venereol Leprol. 2008;74:383-4. http://dx.doi.org/10.4103/0378-6323.42903
Rajapakse S, Rodrigo C, Rajapakse A. Atypical manifestations of Chikungunya infection. Trans R Soc Trop Med Hyg. 2010;104:89-96. http://dx.doi.org/10.1016/j.trstmh.2009.07.031
Faingezicht I, Ávila M. Diagnóstico clínico y de laboratorio del paciente con el dengue. Rev Med Hosp Nac Niños (Costa Rica). 1999;34:33-41.
Algunos artículos similares:
- Daniel Eduardo Henao, Fabián Alberto Jaimes, Medicina basada en la evidencia: una aproximación epistemológica , Biomédica: Vol. 29 Núm. 1 (2009)
- Rubén Gómez, Cristina Fleitas, Carlos Teja, Miguel Carrascosa, Xavier Arrastio, Isabel Celemín, Úlcera aterosclerótica penetrada en cayado aórtico , Biomédica: Vol. 28 Núm. 3 (2008)
- Luz Elena Velásquez, Catalina Gómez, Erika Valencia, Laura Salazar, Eudoro Casas, Estudio de foco de paragonimosis en Fuente Clara, Robledo, área periurbana de Medellín, Antioquia , Biomédica: Vol. 28 Núm. 3 (2008)
- Juan P. Gómez, Juan C. Quintana, Patricia Arbeláez, Jorge Fernández, Juan F. Silva, Jacqueline Barona, Juan C. Gutiérrez, Abel Díaz, Rafael Otero, Picaduras por escorpión Tityus asthenes en Mutatá, Colombia: aspectos epidemiológicos, clínicos y toxinológicos , Biomédica: Vol. 30 Núm. 1 (2010)
- Juan Gabriel Piñeros, Malaria y determinantes sociales de la salud: un nuevo marco heurístico desde la medicina social latinoamericana , Biomédica: Vol. 30 Núm. 2 (2010)
- Richard Hoyos, Lisandro Pacheco, Luz Adriana Agudelo, German Zafra, Pedro Blanco, Omar Triana, Seroprevalencia de la enfermedad de Chagas y factores de riesgo asociados en una población de Morroa, Sucre , Biomédica: Vol. 27 Núm. 1esp (2007): Enfermedad de Chagas
- Angélica María Delgado-Vega, Javier Martín, Julio Granados, Juan Manuel Anaya, Epidemiología genética de la artritis reumatoide: ¿qué esperar de América Latina? , Biomédica: Vol. 26 Núm. 4 (2006)
- Diana Marcela Echeverry, Juan Miguel Rengifo, Jhon Carlos Castaño, Germán Alberto Téllez, María Mercedes González, Prevalencia de Mammomonogamus laryngeus (Strongylida: Syngamidae) en ganado bovino de la central de beneficio del municipio de La Tebaida, Quindío, Colombia , Biomédica: Vol. 31 Núm. 3 (2011)
- Gladys Acuña-González, Carlo E. Medina-Solís, Gerardo Maupomé, Mauricio Escoffie-Ramírez, Jesús Hernández-Romano, María de L. Márquez-Corona, Arturo J. Islas-Márquez, Juan J. Villalobos-Rodelo, Factores de riesgo hereditarios y socioeconómicos para labio o paladar hendido no asociados a un síndrome en México: estudio de casos y controles pareado , Biomédica: Vol. 31 Núm. 3 (2011)
- Pablo Chaparro, Julio Padilla, Mortalidad por paludismo en Colombia, 1979-2008 , Biomédica: Vol. 32 (2012): Suplemento 1, Malaria
| Estadísticas de artículo | |
|---|---|
| Vistas de resúmenes | |
| Vistas de PDF | |
| Descargas de PDF | |
| Vistas de HTML | |
| Otras vistas | |

























