Nutritional status in pediatric patients with predominant antibody deficiency
Abstract
Introduction. Predominant antibody deficiency is the most frequent group of innate immunity errors, but information about patients’ nutritional status is scarce.
Objective. To characterize the nutritional status of Colombian patients with predominant antibody deficiencies.
Material and methods. We analyzed medical charts of patients with predominant antibody deficiency in a pediatric hospital in Bogotá.
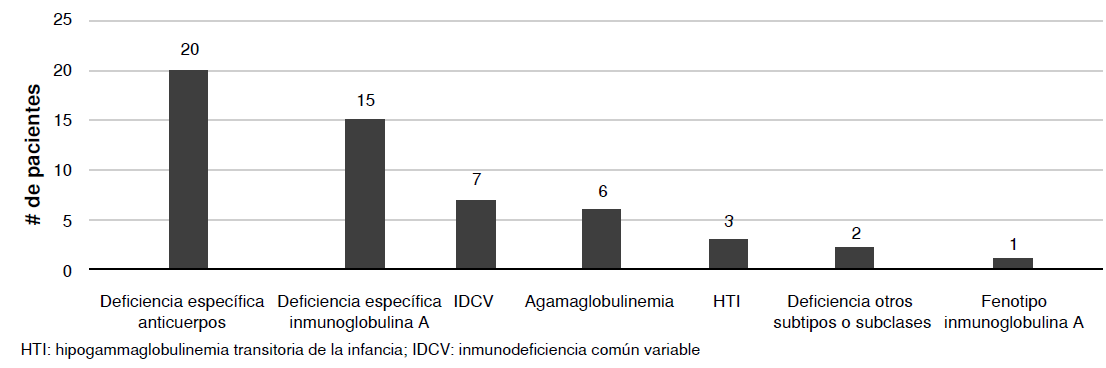
Results. We analyzed 55 medical charts. The most frequent diagnoses were specific deficiencies of polysaccharide antibodies and immunoglobulin A, common variable
immunodeficiency, and agammaglobulinemia. More than 70% of the patients had sinopulmonary infections, with pneumonia being the most frequent, followed by otitis and
sinusitis. In children under five years, 45% had adequate weight for their height, 18% had a risk of malnutrition, and 18% had moderate acute malnutrition. Four-point-five percent had obesity, 4.5% showed overweight, and 9% had a risk of being overweight. Of those older than five years, 54% had an adequate body mass index, 22.5% showed overweight, 9.6% were at risk of thinness, and 9.6% were thin. We found that the risk of short stature and short stature per se were more frequent than the expected height in these patients. The percentages of patients with short stature were higher than those reported nationally.
Conclusions. Due to the epidemic of childhood obesity, it will be more frequent to find overweight or obesity in children above five years. Therefore, finding short stature could be a more sensitive alarm sign for predominant antibody deficiency.
Downloads
References
Tangye SG, Al-Herz W, Bousfiha A, Cunningham-Rundles C, Franco JL, Holland SM, et al. Human inborn errors of immunity: 2022 Update on the Classification from the International Union of Immunological Societies Expert Committee. J Clin Immunol. 2022;42:1473-507. https://doi.org/10.1007/s10875-022-01289-3
Condino-Neto A, Sorensen RU, Gómez-Raccio AC, King A, Espinosa-Rosales FJ, Franco JL. Current state and future perspectives of the Latin American Society for Immunodeficiencies (LASID). Allergol Immunopathol (Madr). 2015;43:493-7. https://doi.org/10.1016/j.aller.2014.05.007
Min Q, Meng X, Wang JY. Primary antibody deficiencies. Adv Exp Med Biol. 2021;70:44-55. https://link.springer.com/article/10.1007/s12026-021-09242-z
Eldeniz FC, Gul Y, Yorulmaz A, Guner SN, Keles S, Reisli I. Evaluation of the 10 warning signs in primary and secondary immunodeficient patients. Front Immunol. 2022;13:900055. https://doi.org/10.3389/fimmu.2022.900055
Bjelac JA, Yonkof JR, Fernández J. Differing performance of the warning signs for immunodeficiency in the diagnosis of pediatric versus adult patients in a two-center tertiary referral population. J Clin Immunol. 2019;39:90-8. https://doi.org/10.1007/s10875-018-0582-z
Karhan AN, Esenboğa S, Gümüş E, Karaatmaca B, Cagdas D, Demir H, et al. Nutritional status of children with primary immunodeficiency: A single center experience. Pediatr Int. 2022;64:e14996. https://doi.org/10.1111/ped.14996
USIDNET. Registry-Reported Statistics. Fecha de consulta: 25 de mayo de 2023. Disponible en: https://usidnet.org/registry-data/stats-registry-enrollment
Thalhammer J, Kindle G, Nieters A, Rusch S, Seppänen MRJ, Fischer A, et al. Initial presenting manifestations in 16,486 patients with inborn errors of immunity include infections and noninfectious manifestations. J Allergy Clin Immunol. 2021;148:1332-41.e5. https://doi.org/10.1016/j.jaci.2021.04.015
Katoch OR. Determinants of malnutrition among children: A systematic review. Nutrition. 2022;96:111565. https://doi.org/10.1016/j.nut.2021.111565
Rytter MJH, Kolte L, Briend A, Friis H, Christensen VB. The immune system in children with malnutrition--A systematic review. PLoS ONE. 2014;9:e105017. https://doi.org/10.1371/journal.pone.0105017
Lankisch P, Schiffner J, Ghosh S, Babor F, Borkhardt A, Laws HJ. The Duesseldorf warning signs for primary immunodeficiency: Is it time to change the rules? J Clin Immunol. 2015;35:273-9. https://doi.org/10.1007/s10875-015-0149-1
Keusch GT. The history of nutrition: Malnutrition, infection and immunity. J Nutr. 2003;133:S336-40. https://doi.org/10.1093/jn/133.1.336S
Modell V, Orange JS, Quinn J, Modell F. Global report on primary immunodeficiencies: 2018 update from the Jeffrey Modell Centers Network on disease classification, regional trends, treatment modalities, and physician reported outcomes. Immunol Res. 2018;66:367-80. https://doi.org/10.1007/s12026-018-8996-5
Subbarayan A, Colarusso G, Hughes SM, Gennery AR, Slatter M, Cant AJ, et al. Clinical features that identify children with primary immunodeficiency diseases. Pediatrics. 2011;127:810-6. https://doi.org/10.1542/peds.2010-3680
Ruffner MA, USIDNET Body Weight Group, Sullivan KE. Complications associated with underweight primary immunodeficiency patients: Prevalence and associations within the USIDNET Registry. J Clin Immunol. 2018;38:283-93. https://doi.org/10.1007/s10875-018-0492-0
Barron MA, Makhija M, Hagen LEM, Pencharz P, Grunebaum E, Roifman CM. Increased resting energy expenditure is associated with failure to thrive in infants with severe combined immunodeficiency. J Pediatr. 2011;159:628-32.e1. https://doi.org/10.1016/j.jpeds.2011.03.041
Dos Santos Nunes Pereira AC, Chahin BM, Tarzia A, Vilela RM. Nutritional status and prognosis in children with immunodeficiencies undergoing hematopoietic stem cell transplantation. Clin Nutr ESPEN. 2022;52:1-11. https://doi.org/10.1016/j.clnesp.2022.09.027
Fajardo Bonilla E. Obesidad Infantil: Otro problema de malnutrición. Revista Med. 2012;20:6-8.
Herman KM, Sabiston CM, Mathieu ME, Tremblay A, Paradis G. Correlates of sedentary behaviour in 8- to 10-year-old children at elevated risk for obesity. Appl Physiol Nutr Metab. 2015;40:10-9. https://doi.org/10.1139/apnm-2014-0039
Troiano RP, Flegal KM, Kuczmarski RJ, Campbell SM, Johnson CL. Overweight prevalence and trends for children and adolescents. The National Health and Nutrition Examination Surveys, 1963 to 1991. Arch Pediatr Adolesc Med. 1995;149:1085-91. https://doi.org/10.1001/archpedi.1995.02170230039005
Laue T, Wrann CD, Hoffmann-Castendiek B, Pietsch D, Hübner L, Kielstein H. Altered NK cell function in obese healthy humans. BMC Obes. 2015;2:1. https://doi.org/10.1186/s40608-014-0033-1
Tanaka S, Inoue S, Isoda F, Waseda M, Ishihara M, Yamakawa T, et al. Impaired immunity in obesity: Suppressed but reversible lymphocyte responsiveness. Int J Obes Relat Metab Disord. 1993;17:631-6.
Ouchi N, Parker JL, Lugus JJ, Walsh K. Adipokines in inflammation and metabolic disease. Nat Rev Immunol. 2011;11:85-97. https://doi.org/10.1038/nri2921
Sheridan PA, Paich HA, Handy J, Karlsson EA, Hudgens MG, Sammon AB, et al. Obesity is associated with impaired immune response to influenza vaccination in humans. Int J Obes (Lond). 2012;36:1072-7. https://doi.org/10.1038/ijo.2011.208
Abolhassani H, Azizi G, Sharifi L, Yazdani R, Mohsenzadegan M, Delavari S, et al. Global systematic review of primary immunodeficiency registries. Expert Rev Clin Immunol. 2020;16:717-32. https://doi.org/10.1080/1744666X.2020.1801422
Abolhassani H, Hirbod-Mobarakeh A, Shahinpour S, Panahi M, Mohammadinejad P, Mirminachi B, et al. Mortality and morbidity in patients with X-linked agammaglobulinaemia. Allergol Immunopathol (Madr). 2015;43:62-6. https://doi.org/10.1016/j.aller.2013.09.013
Kouhkan A, Pourpak Z, Moin M, Dorosty AR, Safaralizadeh R, Teimorian S, et al. A study of malnutrition in Iranian patients with primary antibody deficiency. Iran J Allergy Asthma Immunol. 2004;3:189-96.
Instituto Colombiano de Bienestar Familiar ICBF. ENSIN: Encuesta Nacional de Situación Nutricional. Fecha de consulta: 19 de enero 19 de 2023. Disponible en: https://www.icbf.gov.co/bienestar/nutricion/encuesta-nacional-situacion-nutricional
Dellepiane RM, Dell’Era L, Beilis LV, Pavesi P, Raimondi M, Soresina A, et al. Nutritional status in agammaglobulinemia: An Italian multicenter study. J Clin Immunol. 2015;35:595-7. https://doi.org/10.1007/s10875-015-0195-8
Weinberger T, Fuleihan R, Cunningham-Rundles C, Maglione PJ. Factors beyond lack of antibody govern pulmonary complications in primary antibody deficiency. J Clin Immunol. 2019;39:440-7. https://doi.org/10.1007/s10875-019-00640-5
Pérez EE, Ballow M. Diagnosis and management of specific antibody deficiency. Immunol Allergy Clin North Am. 2020;40:499-510. https://doi.org/10.1016/j.iac.2020.03.005
Latin American Society for Immunodeficiencies. LASID. Estadísticas. Fecha de consulta: 10 de abril de 2024. Disponible en: https://lasidregistry.org/lasid
Some similar items:
- Dra Guzmán, Dra Villamil, Dra Martínez Betancur, Dra Arias, Jacobo Triviño-Arias, Jessica Largo, Dra Lotero, Dr Franco, Dra Castro , Dra Rodríguez, Dra Urcuqui, Dr Medina , Dra Olaya, Understanding secondary hypogammaglobulinemia and its implications for cancer prognosis in children: A retrospective cohort study , Biomedica: Vol. 44 No. Sp. 2 (2024): Inmunología clínica
- Liliana Franco-Hincapié, Constanza Elena Duque, María Victoria Parra, Natalia Gallego, Alberto Villegas, Andrés Ruiz-Linares, Gabriel Bedoya, Association between polymorphism in uncoupling proteins and type 2 diabetes in a northwestern Colombian population , Biomedica: Vol. 29 No. 1 (2009)
- Elpidia Poveda, Diana Giraldo, Yibby Forero, Carlos Mendivil, Self-reported physical activity in comparison with anthropometric body fat indicators in school children , Biomedica: Vol. 28 No. 3 (2008)
- Juan Bernardo Pinzón, Norma Cecilia Serrano, Luis Alfonso Díaz, Gerardo Mantilla, Harvey Mauricio Velasco, Luz Ximena Martínez, Paula Andrea Millán, Sandra Milena Acevedo, Daniel Moreno, Impact of the new definitions in the prevalence of the metabolic syndrome in an adult population at Bucaramanga, Colombia , Biomedica: Vol. 27 No. 2 (2007)
- Berta Nelly Restrepo, María Teresa Restrepo, Juan Camilo Beltrán, Mónica Rodríguez, Ruth Emilia Ramírez, Nutritional status of indigenous children aged up to six years in the Embera-Katio Indian , Biomedica: Vol. 26 No. 4 (2006)
- Yaliana Tafurt-Cardona, Leidy D. Jaramillo-Ruiz, Wilson Muñoz-Ordóñez, Sulma L. Muñoz-Benítez, Carlos H. Sierra-Torres, High frequency of chromosome aberrations observed in lymphocytes in postmenopausal obese women , Biomedica: Vol. 32 No. 3 (2012)
- Nora Elena Múnera, Rosa Magdalena Uscátegui, Beatriz Elena Parra, Luz Mariela Manjarrés, Fredy Patiño, Claudia María Velásquez, Alejandro Estrada, Gabriel Bedoya, Vicky Parra, Angélica María Muñoz, Ana Carolina Orozco, Gloria María Agudelo, Environmental risk factors and metabolic syndrome components in overweight youngsters , Biomedica: Vol. 32 No. 1 (2012)
- Yiby Forero, Gina E. Morales, Edgar Benítez, Comparison of two methodologies used for determining metabolic syndrome in adult population , Biomedica: Vol. 33 No. 2 (2013)
- Tomas Carvajal, Diana L. Franco, Adriana Martínez, Iván M. Peña, Wernicke’s encephalopathy and polyneuropathy associated with vitamin B complex deficiencyafter a bariatric surgery , Biomedica: Vol. 32 No. 4 (2012)
- Álvaro J. Ruiz, Pablo J. Aschner, María Fernanda Puerta, Rafael Alfonso-Cristancho, IDEA Study (International Day for the Evaluation of Abdominal Obesity): Primary care study of the prevalence of abdominal obesity and associated risk factors in Colombia , Biomedica: Vol. 32 No. 4 (2012)
Copyright (c) 2024 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























