Characterization of the health condition of people convalescing from a dengue episode
Abstract
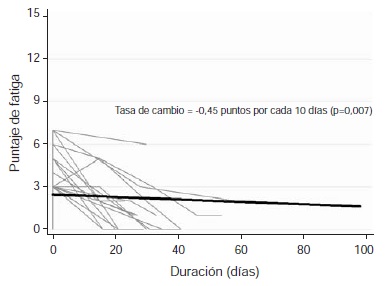
Introduction: Although dengue and its acute manifestations have been broadly described in the literature, the symptoms during the convalescence phase have so far been little studied. Objective: To describe the clinical manifestations of a population during the convalescence phase from a dengue episode. Materials and methods: We conducted an observational study in individuals that were in the hospital after being serologically diagnosed with dengue. After being discharged from the hospital, they were visited in order to verify the persistence of clinical symptoms, fatigue (assessed using the Chalder’s Fatigue Questionnaire) and quality of life (assessed with the EuroQoL-5D questionnaire). Significant fatigue was defined with a score equal to or greater than four in the corresponding scale. Participants with positive [+] fatigue signs were supervised by phone and/or by visiting them in their places of residence until the symptoms disappeared, with a maximum follow-up term of three months. Results: We included 32 individuals in the study (average age: 35 years old, 59% women) and a fatigue prevalence of 34.4% was observed (CI 95% 17.0-51.8). Sociodemographic differences were not defined as determinants with regard to fatigue; by contrast, we found a greater frequency of physical tiredness (100% vs 47.6%; p-0.005) and mental tiredness (54.6% vs 9.5%; p=0.010). Even though patients with fatigue had a poor quality of life, this sign was not statistically different from the group not reporting fatigue when we adjusted by age and sex (OR=5.5; CI 95% 0.83-36.5). In addition, fatigue scores dropped half point in average every 10 days of follow-up. Conclusions: Our results demonstrated that the burden of disease in dengue has not been entirely described, as clinical signs are still present during the convalescence phase, and this represents an obstacle for the normal recovery of individuals.
Downloads
References
Shepard DS, Undurraga EA, Betancourt-Cravioto M, Guzmán MG, Halstead SB, Harris E, et al. Approaches to refining estimates of global burden and economics of dengue. PLoS Negl Trop Dis. 2014;8:e3306. http://dx.doi.org/10.1371/journal.pntd.0003306
Gubler DJ. Dengue, urbanization and globalization: The unholy trinity of the 21st century. Trop Med Health. 2011;39(Suppl.4):S3-11. http://dx.doi.org/10.2149/tmh. 2011-S05
Organización Panamericana de la Salud. Plan detallado de acción para la próxima generación: prevención y control del dengue. Programa de enfermedades transmisibles. Washington, D.C.: OPS; 1999. p. 3-13.
Struchiner CJ, Rocklöv J, Wilder-Smith A, Massad E. Increasing dengue incidence in Singapore over the past 40 years: Population growth, climate and mobility. PLoS One. 2015;10:e0136286. http://dx.plos.org/10.1371/journal.pone.0136286
Malagón JN, Padilla JC, Rojas-Álvarez DP. Guía de atención clínica integral del paciente con dengue. Infectio. 2011;15:293-301.
Instituto Nacional de Salud. Rol del Laboratorio Nacional de Referencia en la epidemia de dengue, Colombia 2010. Fecha de consulta: 17 de abril de 2014. Disponible en: http://190.26.202.205/index.php?idcategoria=86275#
Instituto Nacional de Salud. Dengue. Boletín Epide-miolgógico Semanal. 2015;12:20-1. Fecha de consulta: 17 de abril de 2014. Disponible en: http://www.ins.gov.co/boletin-epidemiologico/Boletn%20Epidemiolgico/2015%20Boletin%20epidemiologico%20semana%2012.pdf
Padilla JC, Rojas-Álvarez DP, Sáenz-Gómez R. Dengue en Colombia, epidemiología de la reemergencia a la hiperendemia. Primera edición. Bogotá, D.C.; Guías de Impresión Ltda.: 2012. p.142-5.
Murray CJ, López AD. Quantifying disability: Data, methods and results. Bull World Health Organ. 1994;72:481-94.
Suaya JA, Shepard DS, Beatty ME. Dengue burden of disease and cost of illness. Scientific Working Group: Report on dengue (Vol. TDR/SWG/08), Geneva: WHO; 2007.
Meltzer MI, Rigau-Pérez JG, Clark GG, Reiter P, Gubler DJ. Using disability-adjusted life years to assess the economic impact of dengue in Puerto Rico: 1984-1994. Am J Trop Med Hyg. 1998;59:265-71.
Anderson KB, Chunsuttiwat S, Nisalak A, Mammen MP, Libraty DH, Rothman AL, et al. Burden of symptomatic dengue infection in children at primary school in Thailand: A prospective study. Lancet. 2007;369:1452-9. http://dx.doi.org/10.1016/S0140-6736(07)60671-0
Tiga-Loza DC, Villar-Centeno LA, Martínez-Vega RA. Discapacidad en dengue y su relación con severidad. Salud UIS. 2011;43:49-55.
Shepard DS, Coudeville L, Halasa YA, Zambrano B, Dayan GH. Economic impact of dengue illness in the Americas. Am J Trop Med Hyg. 2011;84:200-7. http://dx.doi.org/10.4269/ajtmh.2011.10-0503
Castañeda-Orjuela C, Díaz H, Álvis-Guzmán N, Olarte A, Rodríguez H, Camargo G, et al. Burden of disease and economic impact of dengue and severe dengue in Colombia, 2011. Value Heal Reg Issues. 2012;1:123-8. http://dx.doi.org/10.1016/j.vhri.2012.09.014
González D, Martínez R, Castro O, Serrano T, Portela D, Vázquez S, et al. Evaluation of some clinical, humoral and imagenological parameters in patients of dengue haemorrhagic fever six months after acute illness. Dengue Bulletin. 2005;29:79-84.
López-Barroso R, Deulofeu-Betancourt I, Fayad-Saeta Y, Macías-Navarro MM. Convalecencia de mujeres que sufrieron dengue serotipo 3 durante el embarazo. Rev Cuba Med Trop. 2011;63:206-10.
Seet RC, Quek AM, Lim EC. Post-infectious fatigue syndrome in dengue infection. J Clin Virol. 2007;38:1-6. http://dx.doi.org/10.1016/j.jcv.2006.10.011
Chalder T, Berelowitz G, Pawlikowska T, Watts L, Wessely S, Wright D, et al. Development of a fatigue scale. J Psychosom Res. 1993;37:147-53. http://dx.doi.org/10.1016/0022-3999(93)90081-P
Lum LC, Suaya JA, Tan LH, Sah BK, Shepard DS. Quality of life of dengue patients. Am J Trop Med Hyg. 2008;78:862-7.
Olivares P, Departamento de Estudios y Desarrollo. Calidad de vida relacionada a la salud (HR-QoL) en poblacion general de Chile 2005. Santiago de Chile: Superintendencia de Salud; 2006. p. 1-24.
Herdman M, Badia X, Berra S. El EuroQol-5D: una alternativa sencilla para la medición de la calidad de vida relacionada con la salud en atención primaria. Atención Primaria. 2001;28:425-9.
Urzúa MA, Caqueo-Urízar A. Calidad de vida: una revisión teórica del concepto. Ter Psicol. 2012;30:61-71. http://dx. doi.org/10.4067/S0718-48082012000100006
Kondo K. Post-infectious fatigue. JMAJ. 2006;49:27-33.
Holmes GP, Kaplan JE, Gantz NM, Komaroff AL, Schonberger LB, Straus SE, et al. Chronic fatigue syndrome: A working case definition. Ann Intern Med. 1988;108:387-9. http://dx.doi.org/10.7326/0003-4819-108-3-387
Fukuda K, Straus SE, Hickie I, Sharpe MC, Dobbins JG, Komaroff A. The chronic fatigue syndrome: A comprehensive approach to its definition and study. Am Coll Physicians. 1994;121:953-9. http://dx.doi.org/doi:10. 7326/0003-4819-121-12-199412150-00009
Organización Panamericana de la Salud. Dengue: guías para el diagnóstico, tratamiento, prevención y control del dengue, 2009. La Paz: OPS/OMS; 2010. Fecha de consulta: 17 de abril de 2014. Disponible en: http://whqlibdoc.who.int/publications/2009/9789995479213_spa.pdf
Teixeira LD, Lopes JS, Martins AG, Campos FA, Miranzi SD, Nascentes GA. Persistência dos sintomas de dengue em uma população de Uberaba, Minas Gerais, Brasil. Cad Saúde Pública. 2010;26:624-30. http://dx.doi.org/10.1590/S0102-311X2010000300019
García G, González N, Pérez AB, Sierra B, Aguirre E, Rizo D, et al. Long-term persistence of clinical symptoms in dengue-infected persons and its association with immunological disorders. Int J Infect Dis. 2011;15:38-43. http://dx.doi.org/doi:10.1016/j.ijid.2010.09.008
Tristão-Sá R, Kubelka CF, Zandonade E, Zagne SM, Rocha N de S, Zagne LO, et al. Clinical and hepatic evaluation in adult dengue patients: A prospective two-month cohort study. Rev Soc Bras Med Trop. 2012;45:675-81. http://dx.doi.org/10.1590/S0037-86822012000600004
Ayres JG, Flint N, Smith EG, Tunnicliffe WS, Fletcher TJ, Hammond K, et al. Post-infection fatigue syndrome following Q fever. QJM. 1998;91:105-23. http://dx.doi.org/10.1093/qjmed/91.2.105
Straus SE, Tosato G, Armstrong G, Lawley T, Preble OT, Henle W, et al. Persisting illness and fatigue in adults with evidence of Epstein-Barr virus infection. Ann Intern Med. 1985;102:7-16. http://dx.doi.org/10.7326/0003-4819-102-1-7
Hickie I, Davenport T, Wakefield D, Vollmer-Conna U, Cameron B, Vernon SD, et al. Post-infective and chronic fatigue syndromes precipitated by viral and non-viral pathogens: Prospective cohort study. BMJ. 2006;333:575. http://dx.doi.org/10.1136/bmj.38933.585764.AE
Richman DD, Whitley RJ, Hayden FG. Clinical Virology. Third edition. Washington, D.C.: ASM Press: 2009. p. 371-83. http://dx.doi.org/10.1128/9781555815981
Halsey ES, Williams M, Laguna-Torres VA, Vilcarromero S, Ocaña V, Kochel TJ, et al. Occurrence and correlates of symptom persistence following acute dengue fever in Perú. Am J Trop Med Hyg. 2014;90:449-56. http://dx.doi.org/10.4269/ajtmh.13-0544
Some similar items:
- Clara Beatriz Ocampo, Camila González, Carlos A. Morales, Mauricio Pérez, Dawn Wesson, Charles S. Apperson, Evaluation of community-based strategies for Aedes aegypti control inside houses , Biomedica: Vol. 29 No. 2 (2009)
- María Elena Cuéllar-Jiménez, Olga Lucía Velásquez-Escobar, Ranulfo González-Obando, Carlos Andrés Morales-Reichmann, Detection of Aedes albopictus (Skuse) (Diptera: Culicidae) in the city of Cali, Valle del Cauca, Colombia , Biomedica: Vol. 27 No. 2 (2007)
- Natalia Houghton-Triviño, Katherine Martín, Kris Giaya, Jairo A. Rodríguez, Irene Bosch, Jaime E. Castellanos, Comparison of the transcriptional profiles of patients with dengue fever and dengue hemorrhagic fever reveals differences in the immune response and clues in immunopathogenesis , Biomedica: Vol. 30 No. 4 (2010)
- Berta Nelly Restrepo, Margarita Arboleda, Ruth Ramírez, Gonzalo Álvarez, Serum platelet-activating factor acetylhydrolase activity in dengue patients of African or mestizo descendency , Biomedica: Vol. 31 No. 4 (2011)
- Sandy Milena Caldera, María Cristina Jaramillo, Suljey Cochero, Alveiro Pérez-Doria, Eduar Elías Bejarano, Genetic differences between populations of Aedes aegypti from municipalities in northern Colombia, with high and low dengue incidence , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
- Raquel E. Ocazionez-Jiménez, Ayda Susana Ortiz-Báez, Sergio Yebrail Gómez-Rangel, Daniel R. Miranda-Esquivel, Dengue virus serotype 1 (DENV-1) from Colombia: its contribution to dengue occurrence in Santander , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
- Mabel Carabalí, Clara Beatriz Ocampo, María Eugenia Toledo, Lyda Osorio, Mass communication of dengue surveillance data: effect of an intervention in Guadalajara de Buga, Colombia , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
- Luis Ángel Villar-Centeno, Anyela Lozano-Parra, Doris Salgado-García, Óscar F. Herrán, Biochemical alterations as prediction markers for the severity of illness in dengue fever patients , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
- Luis Ángel Villar, Rosa Margarita Gélvez, Jairo Antonio Rodríguez, Doris Salgado, Beatriz Parra, Lyda Osorio, Irene Bosch, Biomarkers for the prognosis of severe dengue , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
- Susanne Ardila-Roldán, Liliana Santacoloma, Helena Brochero, Status of insecticide susceptibility of public health use in natural populations of Aedes aegypti (Diptera: Culicidae) of Casanare, Colombia , Biomedica: Vol. 33 No. 3 (2013)
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























