Multidisciplinary management of antiepileptic drug-induced toxic epidermal necrolysis in a young woman
Abstract
Toxic epidermal necrolysis is a rare, life-threatening dermatological emergency characterized by extensive epidermal detachment and mucosal involvement, associated with high morbidity and mortality. Early diagnosis and prompt treatment are imperative to improving patient outcomes.
This case report describes the clinical course, management, and outcomes of a 29-year-old female diagnosed with toxic epidermal necrolysis. She had a history of polypharmacy and medication allergies and presented with a sudden-onset fever, malaise, and a diffuse rash.
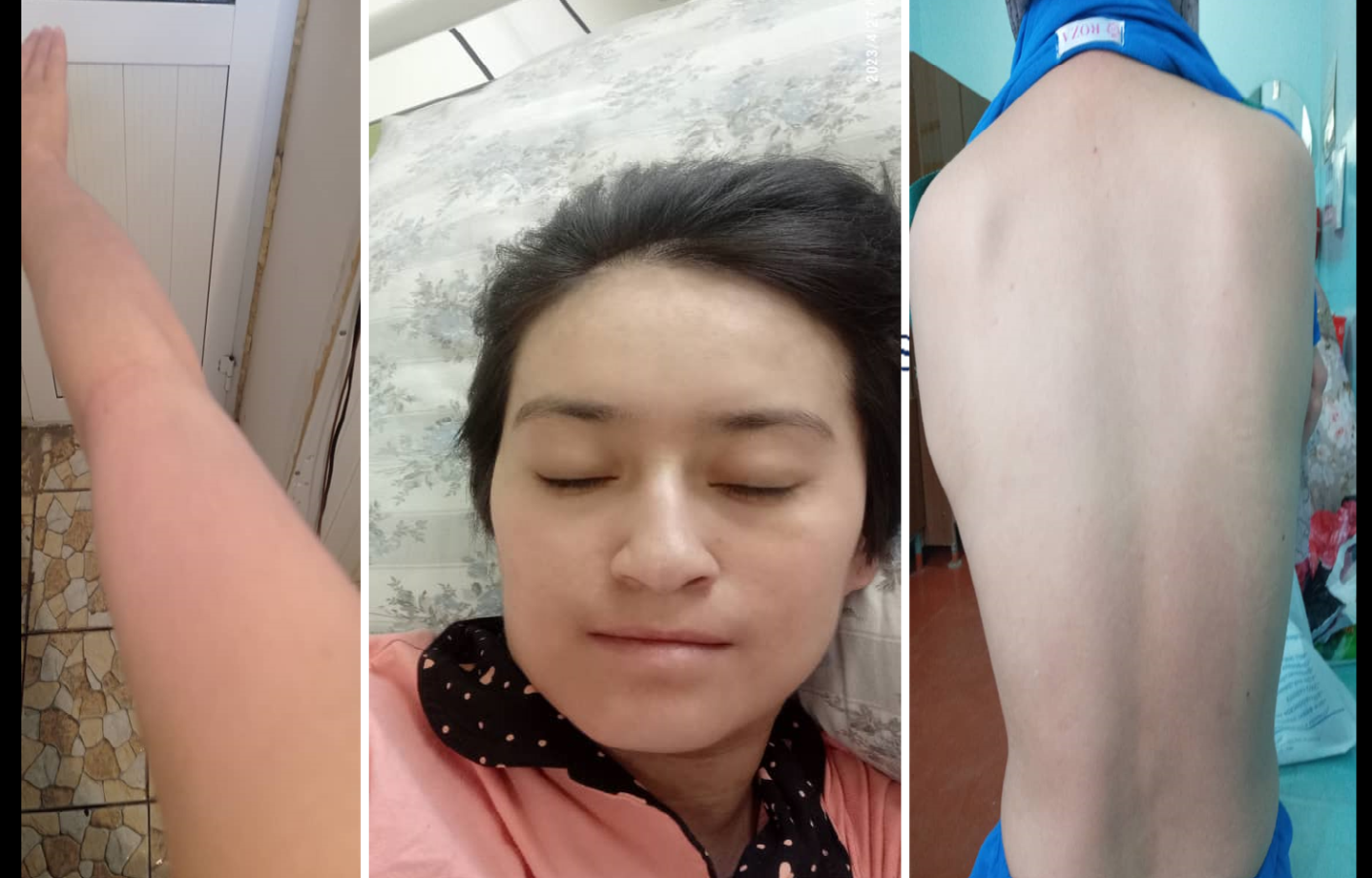
Clinical examination revealed extensive epidermal detachment involving more than 80% of the body surface area, including mucous membranes. Carbamazepine, administered recently, was identified as the suspected causative agent.
The patient was promptly admitted to the intensive care unit for specialized care, including supportive measures, wound care, and close monitoring of fluid and electrolyte balance.
Intravenous immunoglobulin therapy was initiated, together with a multidisciplinary approach involving dermatology, ophthalmology, and nutritional support. The patient’s condition gradually improved over the following weeks, with re-epithelialization of the affected areas and resolution of systemic symptoms.
This case highlighted the importance of early diagnosis, prompt management, and a multidisciplinary approach in optimizing patient outcomes. As toxic epidermal necrolysis is a rare disease, prospective studies, immunogenetic biomarkers, and randomized controlled trials remain limited. Further research in these areas is needed to provide valuable insights into the management of this disease.
Downloads
References
Lyell A. Toxic epidermal necrolysis: An eruption resembling scalding of the skin. Br J Dermatol. 1956;68:355-61. https://doi.org/10.1111/j.1365-2133.1956.tb12766.x
Harr T, French LE. Toxic epidermal necrolysis and Stevens-Johnson syndrome. Orphanet J Rare Dis. 2010;5:39. https://doi.org/10.1186/1750-1172-5-39
Wolkenstein P, Revuz J. Drug-induced severe skin reactions: Incidence, management, and prevention. Drug Saf. 1995;13:56-68. https://doi.org/10.2165/00002018-199513010-00006
Bastuji-Garin S, Rzany B, Stern RS, Shear NH, Naldi L, Roujeau JC. Clinical classification of cases of toxic epidermal necrolysis, Stevens-Johnson syndrome, and erythema multiforme. Arch Dermatol. 1993;129:92-6. https://doi.org/10.1001/archderm.1993.01680220104022
Mockenhaupt M. The current understanding of Stevens-Johnson syndrome and toxic epidermal necrolysis. Expert Rev Clin Immunol. 2011;7:803-13. https://doi.org/10.1586/eci.11.66
Wolkenstein P, Latarjet J, Roujeau JC, Dégos L, Revuz J. Randomised comparison of thalidomide versus placebo in toxic epidermal necrolysis. Lancet. 2002;359:543-4. https://doi.org/10.1016/S0140-6736(02)07754-8
Creamer D, Walsh SA, Dziewulski P, Exton LS, Lee HY, Dart JK, et al. U.K. guidelines for the management of Stevens-Johnson syndrome/toxic epidermal necrolysis in adults 2016. Br J Dermatol. 2016;174:1194-227. https://doi.org/10.1111/bjd.14530
Gupta LK, Martin AM, Agarwal N, D’Souza P. The use of intravenous immunoglobulin in toxic epidermal necrolysis: A retrospective study of non-burn intensive care unit patients. Indian J Dermatol Venereol Leprol. 2006;72:375-8. https://doi.org/10.4103/0378-6323.27700
Roujeau JC, Stern RS. Severe adverse cutaneous reactions to drugs. N Engl J Med. 1994;331:1272-85. https://doi.org/10.1056/NEJM199411103311906
Mockenhaupt M, Viboud C, Dunant A, Naldi L, Halevy S, Bouwes Bavinck JN, et al. Stevens-Johnson syndrome and toxic epidermal necrolysis: Assessment of medication risks with emphasis on recently marketed drugs. The EuroSCAR-study. J Invest Dermatol. 2008;128:35-44. https://doi.org/10.1038/sj.jid.5701033
Bachot N, Roujeau JC. Intravenous immunoglobulin treatment for Stevens-Johnson syndrome and toxic epidermal necrolysis. Dermatol Online J. 2003;9:5. https://escholarship.org/uc/item/4ng9p77w
Schneck J, Fagot JP, Sekula P, Sassolas B, Roujeau JC, Mockenhaupt M. Effects of treatments on the mortality of Stevens-Johnson syndrome and toxic epidermal necrolysis: A retrospective study on patients included in the prospective EuroSCAR Study. J Am Acad Dermatol. 2008;58:33-40. https://doi.org/10.1016/j.jaad.2007.08.036
Devarbhavi H, Raj S, Aradya VH, Rangegowda VT, Veeranna GP, Singh R, Patil M. Druginduced liver injury associated with Stevens-Johnson syndrome/toxic epidermal necrolysis: Patient characteristics, causes, and outcome in 36 cases. Hepatology, 2016;63:993-9. https://doi.org/10.1002/hep.28389
Sanabria-Cabrera J, Medina-Cáliz I, Stankevičiūtė S, Rodríguez-Nicolás A, Almarza-Torres M, Lucena MI, Andrade RJ. Drug-induced liver injury associated with severe cutaneous hypersensitivity reactions: A complex entity in need of a multidisciplinary approach. Curr Pharm Des. 2019;25:3855-71. https://doi.org/10.2174/1381612825666191107161912
Chung WH, Hung SI, Hong HS, Hsih MS, Yang LC, Ho HC, et al. Medical genetics: A marker for Stevens-Johnson syndrome. Nature. 2004;428:486. https://doi.org/10.1038/428486a
Man CB, Kwan P, Baum L, Yu E, Lau KM, Cheng AS, Ng MH. Association between HLA-B*15:02 allele and antiepileptic drug-induced cutaneous reactions in Han Chinese. Epilepsia. 2007;48:1015-8. https://doi.org/10.1111/j.1528-1167.2007.01022.x
Tassaneeyakul W, Tiamkao S, Jantararoungtong T, Chen P, Lin SY, Chen WH, et al. Association between HLA-B*15:02 and carbamazepine-induced severe cutaneous adverse drug reactions in a Thai population. Epilepsia. 2010;51:926-30. https://doi.org/10.1111/j.1528-1167.2010.02533.x
Lonjou C, Thomas L, Borot N, Ledger N, de Toma C, LeLouet H, et al. A marker for Stevens-Johnson syndrome: Ethnicity matters. Pharmacogenomics J. 2006;6:265-8. https://doi.org/10.1038/sj.tpj.6500362
Lonjou C, Borot N, Sekula P, Ledger N, Thomas L, Halevy S, et al. A European study of HLA-B in Stevens-Johnson syndrome and toxic epidermal necrolysis related to five high-risk drugs. Pharmacogenet Genomics. 2008;18:99-107. https://doi.org/10.1097/FPC.0b013e3282f3ef9c
Trent JT, Kirsner RS, Romanelli P, Kerdel FA. Use of wound care products and regimens in patients with chronic wounds at outpatient wound centers: A descriptive study. Adv Skin Wound Care. 2015;28:121-6. https://doi.org/10.1097/01.ASW.0000465328.54013.1c
Some similar items:
- Carolina Guerra, Carlos Santiago Uribe, Alejandro Guerra, Olga H. Hernández, Bickerstaff brain encephalitis: case report and review , Biomedica: Vol. 33 No. 4 (2013)
- Ana Milena Lozano, Juan Felipe López, Josefina Zakzuk, Elizabeth García, Papular urticaria: A review of causal agents in Colombia , Biomedica: Vol. 36 No. 4 (2016)
- Jorge Sánchez, Andrés Sánchez, Ricardo Cardona, Exposure and sensitization to insects in allergic patients in the tropics , Biomedica: Vol. 38 No. Sup. 2 (2018): Suplemento 2, Medicina tropical
- John A. Patiño, Mario J. Olivera, Gastro-allergic anisakiasis: The first case reported in Colombia and a literature review , Biomedica: Vol. 39 No. 2 (2019)
- Ana María Navarro , Gabriela Mantilla, Jorge Andrés Fernández , Mario Fernando Unigarro, Alfonso Suárez , María Claudia Ortega , Severe immunodeficiency spectrum associated with NHEJ1 gene mutation: Cernunnos/XLF deficiency , Biomedica: Vol. 44 No. Sp. 2 (2024): Inmunología clínica
Copyright (c) 2025 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























