Four-month-old infant with chronic granulomatous disease and invasive aspergillosis with bone involvement
Abstract
Chronic granulomatous disease is the inborn error of immunity with the highest frequency of invasive aspergillosis. In this context, invasive aspergillosis is frequent in adolescence, with rare cases before one year of age. We present a case of chronic granulomatous disease and invasive aspergillosis in a four-month-old infant.
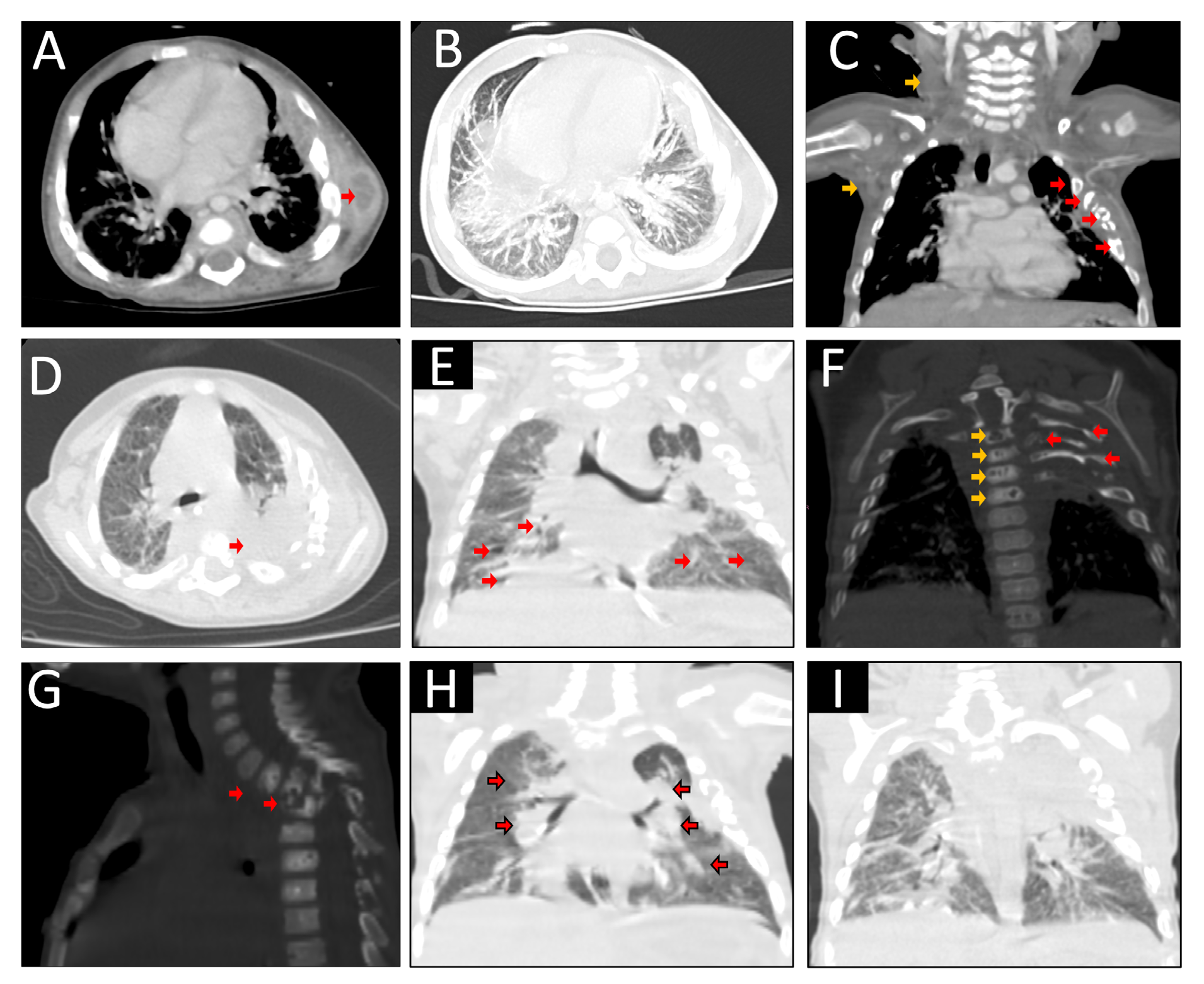
The patient was a male infant living in jail with his hypothyroid mother. He presented with a tumor in the left axillary region when he was four months old, and the chest X-ray suggested rib fractures. The patient was hospitalized on suspicion of child abuse. The chest computed tomography scan showed axillary abscess, rib osteolysis, pneumonia, and pulmonary nodules. He was treated with broad-spectrum antibiotics, and then he was discharged.
Four months later, he was readmitted with fever and extension of the purulent abscess to the left scapular region; a computed tomography scan showed worsening images.
Aspergillus fumigatus was isolated from the abscess pus, leading to an invasive aspergillosis diagnosis. The patient was treated with voriconazole for 28 days, and
then he was discharged. The chronic granulomatous disease was diagnosed by the dihydrorhodamine test. The mutated gene causing the inborn error of immunity was CYBB with the variant c.80_83del/Y; the mother was the carrier (c.80_83del/WT).
At 12 months of age, the patient was readmitted for invasive aspergillosis, refractory to treatment, and died.
This exceptional case teaches us how environmental conditions determine exposure to infectious agents in chronic granulomatous disease patients. Also, it illustrates that invasive aspergillosis can develope in infants with this pathology and should be treated aggressively.
Downloads
References
Antachopoulos C, Walsh TJ, Roilides E. Fungal infections in primary immunodeficiencies. Eur J Pediatr. 2007;166:1099-117. https://doi.org/10.1007/s00431-007-0527-7
Zaoutis TE, Heydon K, Chu JH, Walsh TJ, Steinbach WJ. Epidemiology, outcomes, and costs of invasive aspergillosis in immunocompromised children in the United States, 2000. Pediatrics. 2006;117:e711-6. https://doi.org/10.1542/peds.2005-1161
Henriet S, Verweij PE, Holland SM, Warris A. Invasive fungal infections in patients with chronic granulomatous disease. Adv Exp Med Biol. 2013:764:27-55. http://doi.org/10.1007/978-1-4614-4726-9_3
King J, Henriet S, Warris A. Aspergillosis in chronic granulomatous disease. J Fungi (Basel). 2016;2:15. https://doi.org/10.3390/jof2020015
Marciano BE, Spalding C, Fitzgerald A, Mann D, Brown T, Osgood S, et al. Common severe infections in chronic granulomatous disease. Clin Infect Dis. 2015;60:1176-83. https://doi.org/10.1093/cid/ciu1154
Saito S, Oda A, Kasai M, Minami K, Nagumo H, Shiohara M, et al. A neonatal case of chronic granulomatous disease, initially presented with invasive pulmonary aspergillosis. J Infect Chemother. 2014;20:220-3. http://doi.org/10.1016/j.jiac.2013.10.008
Yoo YJ, Sun JS, Lee JH, Jung HJ, Koh YH, Jung J, et al. Atypical presentation of chronic granulomatous disease in a neonate with a pulmonary granuloma mimicking a tumor: A case report. J Korean Soc Radiol. 2020;81:990. http://doi.org/10.3348/jksr.2020.81.4.990
Herman TE, Siegel MJ. Chronic granulomatous disease of childhood: Neonatal Serratia, hepatic abscesses, and pulmonary aspergillosis. J Perinatol. 2002;22:255-6. http://doi.org/10.1038/sj.jp.7210708
Lee BW, Yap HK. Polyarthritis resembling juvenile rheumatoid arthritis in a girl with chronic granulomatous disease. Arthritis Rheum. 1994;37:773-6. http://doi.org/10.1002/art.1780370524
Davoodi P, Wright SA, Brown EV, Perry JR. Rare diagnosis in a neonate who presents with fever. Clin Pediatr (Phila). 2015;54:91-3. http://doi.org/10.1177/0009922814541809
Chang JH, Boxer LA. Case 2: Infant with lung nodules. Paediatr Child Health. 2007;12:313-6. http://doi.org/10.1093/pch/12.4.229
Mouy R, Ropert JC, Donadieu J, Hubert P, de Blic J, Revillon Y, et al. Granulomatose septique chronique révélée par une aspergillose pulmonaire néonatale. Arch Pediatr. 1995;2:861-4. http://doi.org/10.1016/0929-693x(96)81264-4
Guo C, Chen X, Wang J, Liu F, Liang Y, Yang J, et al. Clinical manifestations and genetic analysis of 4 children with chronic granulomatous disease. Medicine (Baltimore). 2020;99:1-7. http://doi.org/10.1097/md.0000000000020599
Theobald I, Fischbach R, Hülskamp G, Franzius C, Frosch M, Roth J, et al. Pulmonale aspergillose als erstmanifestation einer septischen granulomatose (chronic granulomatous disease, CGD) bei eineiigen weiblichen zwillingsfrühgeborenen und ausbreitungsdiagnostik mittels FDG-PET. Radiologe. 2002;42:42-5. https://doi.org/10.1007/s117-002-8116-0
Lamberto Y, Domínguez C, Arechavala A, Saúl P, Chediack V, Cunto E. Aspergilosis invasiva: definiciones, diagnóstico y tratamiento. Medicina (B Aires). 2023;83:82-95.
Bukkems LMP, van Dommelen L, Regis M, van den Heuvel E, Nieuwenhuizen L. The use of galactomannan antigen assays for the diagnosis of invasive pulmonary aspergillosis in the hematological patient: A systematic review and meta-analysis. J Fungi (Basel). 2023;9:674. https://doi.org/10.3390/jof9060674
Yeoh DK, McMullan BJ, Clark JE, Slavin MA, Haeusler GM, Blyth CC. The challenge of diagnosing invasive pulmonary aspergillosis in children: A review of existing and emerging tools. Mycopathologia. 2023;188:731-43. https://doi.org/10.1007/s11046-023-00714-4
Patterson TF, Thompson GR, Denning DW, Fishman JA, Hadley S, Herbrecht R, et al. Practice guidelines for the diagnosis and management of aspergillosis: 2016 update by the Infectious Diseases Society of America. Clin Infect Dis. 2016;63:e1-60. https://doi.org/10.1093/cid/ciw326
Douglas AP, Smibert OliviaC, Bajel A, Halliday CL, Lavee O, McMullan B, et al. Consensus guidelines for the diagnosis and management of invasive aspergillosis, 2021. Intern Med J. 2021;51:143-76. https://doi.org/10.1111/imj.15591
Abo YN, Gwee A, Osowicki J. Rare infant case of pulmonary aspergilloma highlighting common challenges with voriconazole dosing. Pediatr Infect Dis J. 2021;40:227-30. https://doi.org/10.1097/INF.0000000000002959
Kuruvilla M, de la Morena MT. Antibiotic prophylaxis in primary immune deficiency disorders. J Allergy Clin Immunol Pract. 2013;1:573-82. http://doi.org/10.1016/j.jaip.2013.09.013
Some similar items:
- Juan Gabriel Piñeros, Margarita Arboleda, Juan Camilo Jaramillo, Silvia Blair, Report of five cases of severe neonatal Plasmodium vivax malaria in Urabá, Colombia , Biomedica: Vol. 28 No. 4 (2008)
- Jairo Echeverry, Carlos Mauricio Hurtado, Myriam Gutiérrez, Clinical manifestations of lead levels in children exposed to automobile battery recycling processes in Soacha and Bogotá, D.C. , Biomedica: Vol. 28 No. 1 (2008)
- Olga Lucía Morales, María de la Luz Valencia, Carolina Gómez, María del Pilar Pérez, Emilio Sanín, Luz Marina Vásquez, Chest wall mesenchymal hamartoma: a case report , Biomedica: Vol. 30 No. 1 (2010)
- Claudia Llerena, Santiago Elías Fadul, María Consuelo Garzón, Graciela Mejía, Dora Leticia Orjuela, Luz Mary García, Hilda Beatriz Álvarez, Fernando Javier Ruiz, Drug-resistant Mycobacterium tuberculosis in children under 15 years , Biomedica: Vol. 30 No. 3 (2010)
- Yinth Andrea Bernal, Luis Eduardo Díaz, Jinneth Acosta, Cecilia Crane, Stella Carrasco-Rodríguez, Antonio José Bermúdez, Myriam Sánchez-Gómez, Immunocytochemical and molecular studies with primary cultures of molar tissue , Biomedica: Vol. 26 No. 4 (2006)
- Husein Husein-El Ahmed, Guillermo Arturo Cañadas-De la Fuente, Rafael Fernández-Castillo, Emilio González-Jiménez, Jesús Cantero-Hinojosa, Marita Lardón-Fernández, Generalized cutaneous candidiasis in newborn at term , Biomedica: Vol. 32 No. 2 (2012)
- María Lilia Díaz, Sulma Muñoz, Liz Betty Garcíad, Tuberculosis in the San José University Hospital in Popayán, Colombia, 1998-2000. , Biomedica: Vol. 24 (2004): Suplemento 1
- Beatriz Eugenia Alvarado, Luis Reinel Vásquez, Social determinants, feeding practices and nutritional consequences of intestinal parasitism in young children. , Biomedica: Vol. 26 No. 1 (2006)
- Martín Romero, Diana Chávez, Magalí De los Ríos, Nelson Alvis-Guzmán, Cost-effectiveness of nilotinib, dasatinib and imatinib as first-line treatment for chronic myeloid leukemia in Colombia, 2012 , Biomedica: Vol. 34 No. 1 (2014)
- Doris Martha Salgado, Jairo Antonio Rodríguez, Liliana del Pilar Lozano, Tatiana Esther Zabaleta, Perinatal dengue , Biomedica: Vol. 33 (2013): Suplemento 1, Fiebres hemorrágicas
Copyright (c) 2024 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























