Epidemiology and clinical features of venomous snake bites in the Northern Amazon of Ecuador (2017-2021)
Abstract
Introduction: In Ecuador, poisonous snakebites are a public health problem. However, there is no recent hospital information from the Amazon.
Objective: To retrospectively analyse the clinical-epidemiological characteristics of snakebites in patients admitted to a hospital in the Ecuadorian Amazon.
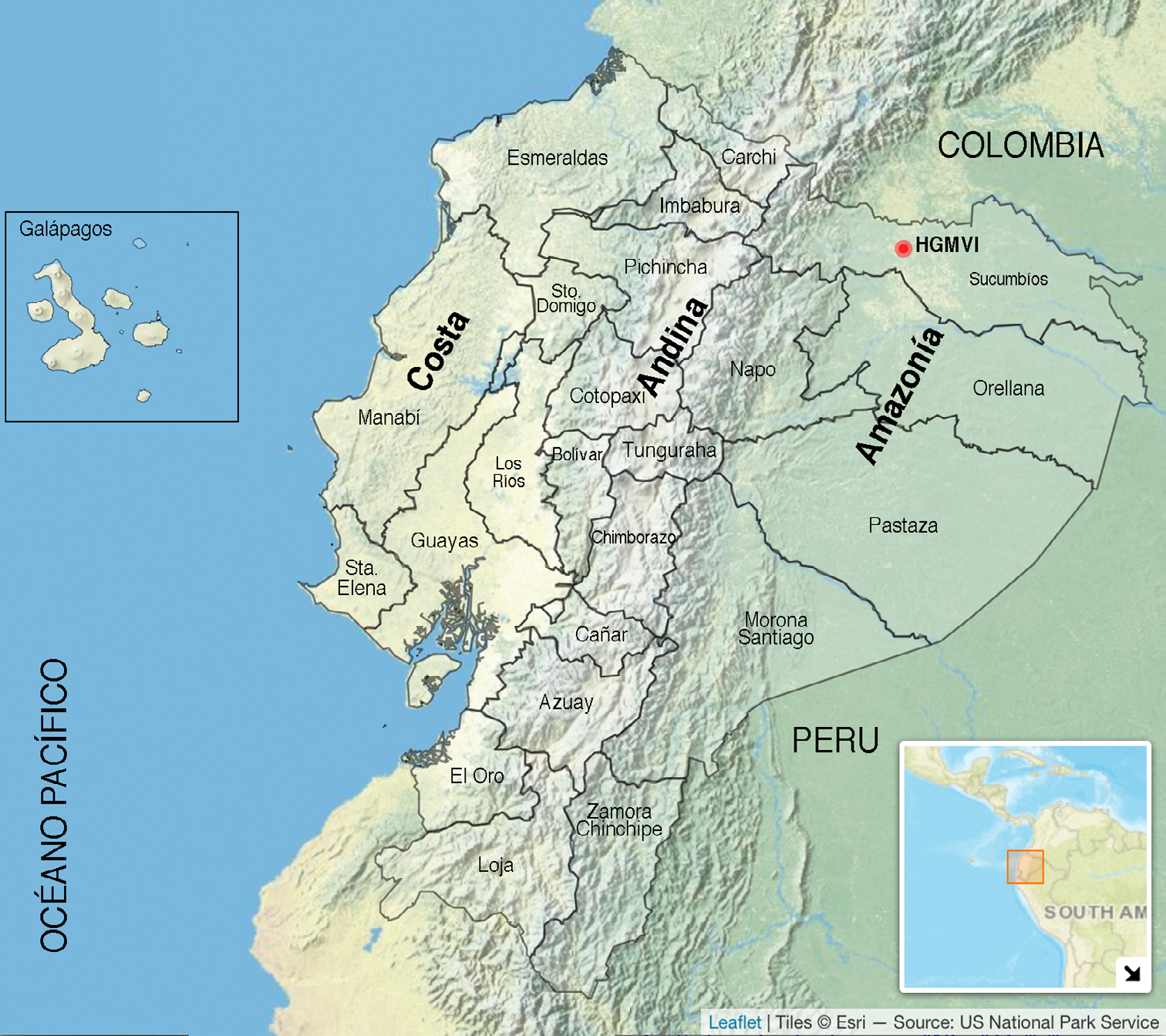
Materials and methods: This is a cross-sectional study conducted at the Nueva Loja-Sucumbíos Provincial Hospital, bordering Colombia (2017-2021). Demographic,
epidemiological and clinical variables, and condition at hospital discharge, were obtained from the epidemiological file of the Ministerio de Salud Pública.
Results: In 5 years, 147 patients (29.4 per year) were hospitalized with no mortality. They corresponded to 26, 34, 32, 29 and 26 cases, in 2017, 2018, 2019, 2020 and 2021, respectively. Men with 99 (67.3%), aged 21-30 years with 28, mixed race with 94 cases, students, and farmers, were the most affected. The most affected (99; 67.3%) were men, people 21 to 30 years-old (28; 19.0%), mestizos (94; 63.9%), students, and farmers. The median age was 28 (range: 4-81) years. Prevalence was higher in April, June, and September. All accidents were caused by Viperidae snakes. Twenty (13.6%) cases were mild, (61.2%) were moderate and 37 (25.2%) were severe. The feet with 45 were the most bitten. Pre-hospitalization anti-venom serum was received by 53.1% and tourniquet by 19.8% patients. Median hospital arrival time was 5 (range 1-192) hours, mostly between 2-3 hours with 41 cases. No statistically significant differences were found considering the severity.
Conclusions: A high prevalence of snakebites was evidenced in the north of the Amazon in Ecuador, with a higher incidence in the rainy season and all by Viperidae species. It is important to highlight the null mortality. Information campaigns on prevention and first aid, such as discouraging the use of tourniquets, especially among vulnerable groups.
Downloads
References
World Health Organization. Snakebite envenoming. Fecha de consulta: 12 de enero de 2022. Disponible en: https://www.who.int/news-room/fact-sheets/detail/snakebiteenvenoming
Williams DJ, Faiz MA, Abela-Ridder B, Ainsworth S, Bulfone TC, Nickerson AD, et al. Strategy for a globally coordinated response to a priority neglected tropical disease: Snakebite envenoming. PLoS Negl Trop Dis. 2019;13:1-12. https://doi.org/10.1371/journal.pntd.0007059
Varela AL, Ron SR. Geografía y clima. Fecha de consulta: 14 de enero de 2022. Disponible en: https://bioweb.bio/faunaweb/amphibiaweb/GeografiaClima/
Yáñez-Arenas C, Díaz-Gamboa L, Patrón-Rivero C, López-Reyes K, Chiappa-Carrara X. Estimating geographic patterns of ophidism risk in Ecuador. Neotropical Biodiversity. 2018;4:55-61. http://doi.org/10.1080/23766808.2018.1454762
Chippaux JP. Incidence and mortality due to snakebite in the Americas. PLoS Negl Trop Dis. 2017;11:1-39. https://doi.org/10.1371/journal.pntd.0005662
Ministerio de Salud Pública. Manejo clínico de pacientes con mordeduras de serpientes venenosas y picaduras de escorpiones. Primera edición. Quito: Dirección Nacional de Prevención y Control y Dirección Nacional de Normatización; 2017. p. 1-113.
Smalligan R, Cole J, Brito N, Laing GD, Mertz BL, Manock S, et al. Crotaline snake bite in the Ecuadorian Amazon: Randomised double blind comparative trial of three South American polyspecific antivenoms. Br Med J. 2004;329:1-7. https://doi.org/10.1136/bmj.329.7475.1129
Manock SR, Suárez G, Graham D, Ávila-Aguero ML, Warrell DA. Neurotoxic envenoming by South American coral snake (Micrurus lemniscatus helleri): Case report from eastern Ecuador and review. Trans R Soc Trop Med Hyg. 2008;102:1127-32. https://doi.org/10.1016/j.trstmh.2008.03.026
Ochoa-Avilés A, Heredia-Andino OS, Escandón SA, Celorio-Carvajal CA, Arias-Peláez MC, Zaruma-Torres F, et al. Viperidae snakebites in Ecuador: A review of epidemiological and ecological aspects. Toxicon X. 2020;7:1-8. https://doi.org/10.1016/j.toxcx.2020.100051
Praba-Egge AD, Cone SW, Araim O, Freire IL, Paida G V, Escalante JT, et al. Snakebites in the rainforests of Ecuador. World J Surg. 2003;27:234-40. https://doi.org/10.1007/s00268-002-6552-9
Kerrigan KR. Venomous snakebite in eastern Ecuador. Am J Trop Med Hyg. 1991;44:93-9. https://doi.org/10.4269/ajtmh.1991.44.93
Ministerio de Salud Pública-Subsecretaría de Vigilancia de la Salud Pública. Efectos tóxicos año 2020. Fecha de consulta: 21 de enero de 2022. Disponible en: https://www.salud.gob.ec/wp-content/uploads/2021/01/Toxicos-y-quimicos-SE-53.pdf
Instituto Nacional de Estadística y Censos. Estadísticas. Fecha de consulta: 12 de enero de 2022. Disponible en: https://www.ecuadorencifras.gob.ec/estadisticas/
López V, Espíndola F, Calles J, Ulloa J. Atlas “Amazonía Ecuatoriana Bajo Presión”. Quito: EcoCiencia; 2013. p. 1-56. Fecha de consulta: 12 de enero de 2022. Disponible en: https://www.amazoniasocioambiental.org/wp-content/uploads/2017/01/AmazoniaEcuatoriana_bajo_presion.pdf
Larrick JW, Yost JA, Kaplan J. Snake bite among the Waorani indians of Eastern Ecuador. Trans R Soc Trop Med Hyg. 1978;72:542-3. https://doi.org/10.1016/0035-9203(78)90184-0
González-Andrade F, Chippaux JP. Snake bite envenomation in Ecuador. Trans R Soc Trop Med Hyg. 2010;104:588-91. https://doi.org/10.1016/j.trstmh.2010.05.006
Creagh I, Pérez Y, Gámez D, Dueñas O. Características clínico epidemiológicas de los accidentes ofídicos. Ecuador, 2014. IntraMed Journal. 2017;6:7.
Giovannini P. Medicinal plants of the Achuar (Jivaro) of Amazonian Ecuador: Ethnobotanical survey and comparison with other Amazonian pharmacopoeias. J Ethnopharmacol. 2015;164:78-88. https://doi.org/10.1016/j.jep.2015.01.038
Gobierno Autónomo Descentralizado de la Provincia de Sucumbíos. Actualización Plan de Desarrollo y Ordenamiento Territorial, 2015. Fecha de consulta: 12 de enero de 2020. Disponible en: http://app.sni.gob.ec/sni-link/sni/PORTAL_SNI/data_sigad_plus/sigadplusdocumentofinal/2160000210001_PDyOT%20Sucumbios%20-%202015%20(actual
izaci%C3%B3n)_17-08-2015_18-31-36.pdf
World Health Organization. International Statistical Classification of Diseases and Related Health Problems, 10th Revision, 2016. Fecha de consulta: 21 de marzo de 2020.Disponible en: https://icd.who.int/browse10/2016/en
The Jamovi project. Jamovi. 2019. Fecha de consulta: 12 de enero de 2020. Disponible en: https://www.jamovi.org
Means R, Cabrera J, Moreno X, Amini R. Remote South American snakebite with extensive myonecrosis. Clin Pract Cases Emerg Med. 2017;1:47-9. https://doi.org/10.5811/cpcem.2016.11.31220
Theakston RDG, Laiug GD, Fielding CM, Lascano AF, Touzet JM, Vallejo F, et al. Treatment of snake bites by Bothrops species and Lachesis muta in Ecuador: Laboratory screening of candidate antivenoms. Trans R Soc Trop Med Hyg. 1995;89:550-4. https://doi.org/10.1016/0035-9203(95)90105-1
Da Silva AM, Colombini M, Moura-Da-Silva AM, De Souza RM, Monteiro WM, Bernarde PS. Epidemiological and clinical aspects of snakebites in the Upper Juruá River Region, Western Brazilian Amazonia. Acta Amaz. 2020;50:90-9. https://www.amazoniasocioambiental.org/wp-content/uploads/2017/01/AmazoniaEcuatoriana_bajo_presion.pdf
Valverde-Muñoz G, Romero-Álvarez D. Measuring the epidemiological uncertainty in snakebite case reports in 2016 Ecuador. Int J Infect Dis. 2018;73:211. https://doi.org/10.1016/j.ijid.2018.04.3894
Warrell DA. Guidelines of management of snake bite. Lancet. 2010;375:77-88. https://doi.org/10.1016/S0140-6736(09)61754-2
Oliveira FN, Brito MT, Morais ICO de, Fook SML, Albuquerque HN. Accidents caused by Bothrops and Bothropoides in the State of Paraiba: Epidemiological and clinical aspects. Rev Soc Bras Med Trop. 2010;43:662-7. https://doi.org/10.1590/S0037-86822010000600012
Otero-Patiño R. Snake bites in Colombia. En: Gopalakrishnakone P, Faiz S, Gnanathasan C, Habib A, Fernando R, Yang CC, editores. Clinical Toxinology. Dordrecht: Springer; 2014. p. 1-42. https://doi.org/10.1007/978-94-007-6288-6_41-2
Ortiz-Prado E, Yeager J, Andrade F, Schiavi-Guzmán C, Abedrabbo-Figueroa P, Terán E, et al. Snake antivenom production in Ecuador: Poor implementation, and an unplanned cessation leads to a call for a renaissance. Toxicon. 2021;202:90-7. https://doi.org/10.1016/j.toxicon.2021.09.014
Some similar items:
- Leonardo De Sousa, Adolfo Borges, Enzo De Sousa-Insana, Aleikar Vásquez-Suárez, Mortality caused by venomous animals in Venezuela (2000-2009): A new epidemiological pattern , Biomedica: Vol. 41 No. 1 (2021)
- Daniel Eduardo Henao, Fabián Alberto Jaimes, Evidence-based medicine: an epistemological approach , Biomedica: Vol. 29 No. 1 (2009)
- Luz Elena Velásquez, Catalina Gómez, Erika Valencia, Laura Salazar, Eudoro Casas, Paragonimosis in the peri-urban zone of Medellín, Antioquia , Biomedica: Vol. 28 No. 3 (2008)
- Juan P. Gómez, Juan C. Quintana, Patricia Arbeláez, Jorge Fernández, Juan F. Silva, Jacqueline Barona, Juan C. Gutiérrez, Abel Díaz, Rafael Otero, Tityus asthenes scorpion stings: epidemiological, clinical and toxicological aspects , Biomedica: Vol. 30 No. 1 (2010)
- Juan Gabriel Piñeros, Malaria and social health determinants: a new heuristic framework from the perspective of Latin American social medicine , Biomedica: Vol. 30 No. 2 (2010)
- Richard Hoyos, Lisandro Pacheco, Luz Adriana Agudelo, German Zafra, Pedro Blanco, Omar Triana, Seroprevalence of Chagas disease and associated risk factors in a population of Morroa, Sucre , Biomedica: Vol. 27 No. 1esp (2007): Enfermedad de Chagas
- Angélica María Delgado-Vega, Javier Martín, Julio Granados, Juan Manuel Anaya, Epidemiología genética de la artritis reumatoide: ¿qué esperar de América Latina? , Biomedica: Vol. 26 No. 4 (2006)
- Diana Marcela Echeverry, Juan Miguel Rengifo, Jhon Carlos Castaño, Germán Alberto Téllez, María Mercedes González, Prevalence of Mammomonogamus laryngeus (Strongylida: Syngamidae) nematodes in a bovine slaughterhouse , Biomedica: Vol. 31 No. 3 (2011)
- Gladys Acuña-González, Carlo E. Medina-Solís, Gerardo Maupomé, Mauricio Escoffie-Ramírez, Jesús Hernández-Romano, María de L. Márquez-Corona, Arturo J. Islas-Márquez, Juan J. Villalobos-Rodelo, Family history and socioeconomic risk factors for non-syndromic cleft lip and palate: A matched case-control study in a less developed country , Biomedica: Vol. 31 No. 3 (2011)
- Pablo Chaparro, Julio Padilla, Malaria mortality in Colombia, 1979-2008 , Biomedica: Vol. 32 (2012): Suplemento 1, Malaria
Copyright (c) 2023 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























