Prevalence of intestinal parasites in a cohort of HIVinfected patients from Antioquia, Colombia
Abstract
Introduction: HIV infection is still a public health problem worldwide and co-infections with other infectious agents including intestinal parasites are of particular concern, mainly in developing countries like Colombia.
Objective: To conduct a cross-sectional study in patients attending an HIV care program in Antioquia given that there have been few intestinal parasites prevalence studies among the HIV population in the country.
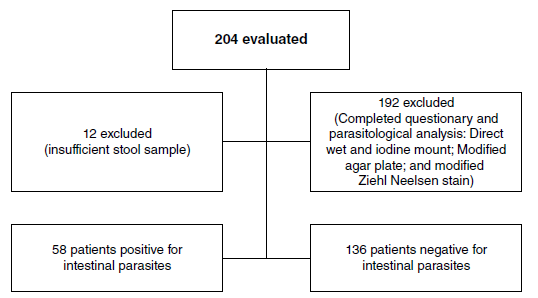
Material and methods: We evaluated stool samples from 192 patients by direct wet mount and concentration, modified Ziehl Neelsen staining, and agar plate culture. Univariate and correlation analyses were done to explore the association between socio-demographic and clinical characteristics and parasitological data.
Results: The overall prevalence of intestinal parasites in HIV-positive subjects was 29.2% (56/192; 95% CI: 22.8% - 35.6%). Entamoeba histolytica/dispar/moshkosvkii with 13.0% (25/192; 95% CI: 8.2% - 17.8%) and Blastocystis with 12.0% (23/192; 95% CI: 7.4% - 16.6%) were the most frequent. Opportunistic parasites like Cryptosporidium spp. and Cystoisospora belli were less prevalent, each one with 0.5% of positive samples (1/192; 95% CI: 0.1% - 1.5%). Commensal protozoa were also detected with a prevalence of 18.8% (36/192; 95% CI: 13.3% - 24.3%). Most of the individuals in the study had a controlled viral load and an LTCD4 count greater than 200 cel/μL. A small percentage (9.3%) had diarrhea. Bivariate analysis and multivariate logistic regression showed that only age and having pets had a significant association with intestinal parasites in this cohort.
Conclusions: Our results confirmed that the evaluated population is at high risk of intestinal parasite infection, which highlights the need for routine screening of gastrointestinal parasites to provide prompt treatment and reduce possible complications.
Downloads
References
Nwosu FC, Avershina E, Wilson R, Rudi K. Gut microbiota in HIV infection: Implication for disease progression and management. Gastroenterol Res Pract. 2014;2014:1-6. https://doi.org/10.1155/2014/803185
Tian L-G, Wang T-P, Lv S, Wang F-F, Guo J, Yin X-M, et al. HIV and intestinal parasite co-infections among a Chinese population: An immunological profile. Infect Dis Poverty. 2013;2:18. https://doi.org/10.1186/2049-9957-2-18
Botero JH, Castaño A, Montoya MN, Ocampo NE, Hurtado MI, Lopera MM. A preliminary study of the prevalence of intestinal parasites in immunocompromised patients with and without gastrointestinal manifestations. Rev Inst Med Trop Sao Paulo. 2003;4:197-200. https://doi.org/10.1590/S0036-46652003000400004
Valbuena AM, Ramírez PX, Castillo JC, Trujillo SJ. Situación del VIH Sida en Colombia 2019. Fondo Colombiano de Enfermedades de Alto Costo. Cuenta Alto Costo. Consulted: Oct 30 2020. Available from: https://cuentadealtocosto.org/site/wp-content/uploads/2020/08/VIH2019.pdf.
Ministerio de Salud y Protección Social, Universidad de Antioquia. Encuesta Nacional de Parasitismo Intestinal en Población Escolar, Colombia, 2012-2014. 2015. p. 1-174. Accessed on: October 30, 2020. Available from: https://www.minsalud.gov.co/sites/rid/Lists/BibliotecaDigital/RIDE/VS/PP/ET/encuesta-nacional-de-parasitismo-2012-2014.pdf
Agudelo-González S, Murcia-Sánchez F, Salinas D, Osorio J. Infecciones oportunistas en pacientes con VIH en el hospital universitario de Neiva, Colombia. 2007-2012. Infectio. 2015;19:52-9. https://doi.org/10.1016/j.infect.2014.11.008
Navarro-i-Martínez L, Da Silva AJ, Botero-Garcés JH, Montoya-Palacio MN, Del Águila C, Bornay-LLinares FJ. Cryptosporidiosis in HIV-positive patients from Medellín, Colombia. J Eukaryot Microbiol. 2006;53(Suppl.1):S37-9. https://doi.org/10.1111/j.1550-7408.2006.00167.x
García LS, Arrowood M, Kokoskin E, Paltridge GP, Pillai DR, Procop GW, et al. Practical Guidance for Clinical Microbiology Laboratories: Laboratory diagnosis of parasites from the gastrointestinal tract. Clin Microbiol Rev. 2018;31. https://doi.org/10.1128/CMR.00025-17
Flórez AC, García DA, Moncada L, Beltrán M. Prevalence of microsporidia and other intestinal parasites in patients with HIV infection, Bogotá, 2001. Biomédica. 2003;23:274-82. https://doi.org/10.7705/biomedica.v23i3.1221
Botero JH, Montoya MN, Vanegas AL, Díaz A, Navarro-i-Martínez L, Izquierdo F, et al. Frecuencia de microsporidiosis intestinal en pacientes positivos para VIH mediante las técnicas de Gram cromotropo rápido y PCR. Biomédica. 2004;24:375. https://doi.org/10.7705/biomedica.v24i4.1287
Costa-Cruz JM, Ferreira MS, Rossin IR. Intestinal parasites in AIDS and +HIV patients in Uberlândia, Minas Gerais, Brazil. Mem Inst Oswaldo Cruz. 1996;91:685-6. https://doi.org/10.1590/S0074-02761996000600004
Barcelos NB, Silva L de F e, Dias RFG, Menezes Filho HR de, Rodrigues RM. Opportunistic and non-opportunistic intestinal parasites in HIV/ AIDS patients in relation to their clinical and epidemiological status in a specialized medical service in Goiás, Brazil. Rev Inst Med Trop Sao Paulo. 2018;60:1-9. https://doi.org/10.1590/s1678-9946201860013
Rivero-Rodríguez Z, Hernández A, Bracho Á, Salazar S, Villalobos R. Prevalencia de microsporidios intestinales y otros enteroparásitos en pacientes VIH positivos de Maracaibo, Venezuela. Biomédica. 2013;33:538-45. https://doi.org/10.7705/biomedica.v33i4.1468
Silva-Díaz H, Failoc-Rojas VE. Frequency and etiology of enteroparasitosis in patients with human immunodeficiency virus at a hospital of Lambayeque, Perú. Rev Habanera Ciencias Médicas. 2019;18:418-27.
Shirley D-AT, Farr L, Watanabe K, Moonah S. A Review of the global burden, new diagnostics, and current therapeutics for amebiasis. Open Forum Infect Dis. 2018;5:ofy161. https://doi.org/10.1093/ofid/ofy161
Moran P, Ramos F, Ramiro M, Curiel O, González E, Valadez A, et al. Entamoeba histolytica and/or Entamoeba dispar: Infection frequency in HIV+/AIDS patients in México city. Exp Parasitol. 2005;110:331-4. https://doi.org/10.1016/j.exppara.2005.03.023
Samie A, Barrett LJ, Bessong PO, Ramalivhana JN, Mavhandu LG, Njayou M, et al. Seroprevalence of Entamoeba histolytica in the context of HIV and AIDS: The case of Vhembe district, in South Africa’s Limpopo province. Ann Trop Med Parasitol. 2010;104:55-63. https://doi.org/10.1179/136485910X12607012373911
Cheng X, Tachibana H, Chen Y, Zhang Y, Yang B, Qi T, et al. Seroprevalence of Entamoeba histolytica infection in HIV-infected patients in China. Am J Trop Med Hyg. 2007;77:825-8. https://doi.org/10.4269/ajtmh.2012.11-0626
Abdollahi A, Saffar HH, Saffar HH, Sheikhbahaei S, Rasoulinejad M. Is the evaluation of Entamoeba histolytica infection in HIV-positive patients of any clinical significance? Acta Med Iran. 2015;53:46-50.
Skotarczak B. Genetic diversity and pathogenicity of Blastocystis. Ann Agric Environ Med. 2018;25:411-6. https://doi.org/10.26444/aaem/81315
Kumarasamy V, Anbazhagan D, Subramaniyan V, Vellasamy S. Blastocystis sp., Parasite associated with gastrointestinal disorders: An overview of its pathogenesis, immune modulation, and therapeutic strategies. Curr Pharm Des. 2018;24:3172-5. https://doi.org/10.2174/1381612824666180807101536
Fontanelli-Sulekova L, Gabrielli S, Furzi F, Milardi GL, Biliotti E, De Angelis M, et al. Molecular characterization of Blastocystis subtypes in HIV-positive patients and evaluation of risk factors for colonization. BMC Infect Dis. 2019;19:876. https://doi.org/10.1186/s12879-019-4537-7
Laksemi DA, Suwanti LT, Mufasirin M, Suastika K, Sudarmaja M. Opportunistic parasitic infections in patients with human immunodeficiency virus/acquired immunodeficiency syndrome: A review. Vet World. 2020;13:716-25. https://doi.org/10.14202/vetworld.2020.716-725
Wang Z-D, Liu Q, Liu H-H, Li S, Zhang L, Zhao Y-K, et al. Prevalence of Cryptosporidium, microsporidia and Isospora infection in HIV-infected people: A global systematic review and meta-analysis. Parasit Vectors. 2018;11:28. https://doi.org/10.1186/s13071-017-2558-x
Arzuza O, Arroyo B, Villegas S, Rocha A, Díaz H. Infecciones parasitarias intestinales en pacientes positivos para el virus de la inmunodeficiencia humana (VIH) en la ciudad de Cartagena de Indias, Colombia. Infectio. 2003;7:58-63.
Siuffi M, Angulo M, Velasco CA, López P, Dueñas VH, Rojas C. Relación entre los niveles de carga viral y los niveles de linfocitos CD4 en el diagnóstico de Cryptosporidium spp. en heces de niños de la Clínica pediátrica de VIH/SIDA del Hospital Universitario del Valle, Cali, Colombia. Colomb Med. 2006;37:15-20. https://doi.org/10.25100/cm.v37i1.407
Velasco CA, Méndez F, López P. Cryptosporidiosis in Colombian children with HIV/AIDS infection. Colomb Med. 2011;42:1-13. https://doi.org/10.25100/cm.v42i4.942
Montúfar Andrade F, Quiroga A, Builes C, Saldarriaga C, Aguilar C, Mesa M, et al. Epidemiología de la infección por el virus de inmunodeficiencia humana en pacientes hospitalizados en una institución de alta complejidad y enseñanza universitaria en Medellín, Colombia. Infectio. 2016;20:9-16. https://doi.org/10.1016/j.infect.2015.05.004
López MC, Moneada LI, Murcia MI, Saravia J, Nicholls RS. Frecuencia de parásitos intestinales en pacientes VIH+ en la ciudad de Santa Fe de Bogotá. Rev Fac Med. 1999;47:9-12.
Schär F, Trostdorf U, Giardina F, Khieu V, Muth S, Marti H, et al. Strongyloides stercoralis: Global distribution and risk factors. PLoS Negl Trop Dis. 2013;7:e2288. https://doi.org/10.1371/journal.pntd.0002288
Feitosa G, Bandeira AC, Sampaio DP, Badaró R, Brites C. High prevalence of giardiasis and strongyloidiasis among HIV-infected patients in Bahia, Brazil. Brazilian J Infect Dis. 2001;5:339-44. https://doi.org/10.1590/S1413-86702001000600008
Pinlaor S, Mootsikapun P, Pinlaor P, Pipitgool V, Tuangnadee R. Detection of opportunistic and non-opportunistic intestinal parasites and liver flukes in HIV-positive and HIV-negative subjects. Southeast Asian J Trop Med Public Health. 2005;36:841-5.
Aru RG, Chilcutt BM, Butt S, DeShazo RD. Novel findings in HIV, immune reconstitution disease and Strongyloides stercoralis infection. Am J Med Sci. 2017;353:593-6. https://doi.org/10.1016/j.amjms.2016.05.021
Barnes AN, Davaasuren A, Baasandagva U, Gray GC. A systematic review of zoonotic enteric parasitic diseases among nomadic and pastoral people. PLoS ONE. 2017;12:e0188809. https://doi.org/10.1371/journal.pone.0188809
Harvey TV, Tang AM, da Paixao Sevá A, Albano dos Santos C, Santos Carvalho SM, Magalhães da Rocha CMB, et al. Enteric parasitic infections in children and dogs in resource-poor communities in northeastern Brazil: Identifying priority prevention and control areas. PLoS Negl Trop Dis. 2020;14:e0008378. https://doi.org/10.1371/journal.pntd.0008378
Lowenstein C, Vasco K, Sarzosa S, Salinas L, Torres A, Perry MJ, et al. Determinants of childhood zoonotic enteric infections in a semirural community of Quito, Ecuador. Am J Trop Med Hyg. 2020;102:1269-78. https://doi.org/10.4269/ajtmh.19-0690
Witkowski JM, Bryl E, Fulop T. Should we try to alleviate immunosenescence and inflammaging - Why, how, and to what extent? Curr Pharm Des. 2019;25:4154-62. https://doi.org/10.2174/1381612825666191111153016
Suleiman BA, Yahaya M, Olaniyan FA, Sule AG, Sufiyan MB. Determinants of healthrelated quality of life among human immunodeficiency virus-positive (HIV-positive) patients at Ahmadu Bello University teaching hospital, Zaria, Nigeria- 2015. BMC Public Health. 2020;20:531. https://doi.org/10.1186/s12889-020-08659-9
Abange WB, Nkenfou CN, Gonsu-Kamga H, Nguedia CA, Kamgaing N, Lozupone C, et al. Intestinal parasites infections among HIV infected children under antiretrovirals treatment in Yaounde, Cameroon. J Trop Pediatr. 2020;66:178-86. https://doi.org/10.1093/tropej/fmz048
Zorbozan O, Quliyeva G, Tunali V, Ozbilgin A, Turgay N, Gokengin AD. Intestinal protozoa in HIV-infected patients: A retrospective analysis. Turkish J Parasitol. 2018;42:187-90. https://doi.org/10.5152/tpd.2018.5835
Taye B, Desta K, Ejigu S, Dori GU. The magnitude and risk factors of intestinal parasitic infection in relation to human immunodeficiency virus infection and immune status, at ALERT Hospital, Addis Ababa, Ethiopia. Parasitol Int. 2014;63:550-6. https://doi.org/10.1016/j.parint.2014.02.002
Some similar items:
- José Moreno-Montoya, Ana M. Barragán, Margin Martínez, Amanda Rodríguez, Ángela Carmela González, Quality of life and perceived social support in people with HIV in Bogotá, Colombia , Biomedica: Vol. 38 No. 4 (2018)
- Elizabeth Borrero, Gabriel Carrasquilla, Neal Alexander, Decentralization and health system reform: What is their impact on malaria incidence in Colombian municipalities? , Biomedica: Vol. 32 (2012): Suplemento 1, Malaria
- Raúl Murillo, Ricardo Cendales, Carolina Wiesner, Marion Piñeros, Sandra Tovar, Effectiveness of cytology-based cervical cancer screening in the Colombian health system , Biomedica: Vol. 29 No. 3 (2009)
- Sandra Lorena Girón, Julio César Mateus, Fabián Méndez, Impact of an open waste disposal site on the occurrence of respiratory symptoms and on health care costs of children , Biomedica: Vol. 29 No. 3 (2009)
- José Joaquín Carvajal, Ligia Inés Moncada, Mauricio Humberto Rodríguez, Ligia del Pilar Pérez, Víctor Alberto Olano, Characterization of Aedes albopictus (Skuse, 1894) (Diptera:Culicidae) larval habitats near the Amazon River in Colombia , Biomedica: Vol. 29 No. 3 (2009)
- Andrés Páez, Gloria Rey, Carlos Agudelo, Alvaro Dulce, Edgar Parra, Hernando Díaz-Granados, Damaris Heredia, Luis Polo, Outbreak of urban rabies transmitted by dogs in Santa Marta, northern Colombia , Biomedica: Vol. 29 No. 3 (2009)
- Patricia Escobar, Katherine Paola Luna, Indira Paola Hernández, César Mauricio Rueda, María Magdalena Zorro, Simon L. Croft, In vitro susceptibility of Trypanosoma cruzi strains from Santander, Colombia, to hexadecylphosphocholine (miltefosine), nifurtimox and benznidazole , Biomedica: Vol. 29 No. 3 (2009)
- Gustavo Pradilla, Julio César Mantilla, Reynaldo Badillo, Human rabies encephalitis by a vampire bat bite in an urban area of Colombia , Biomedica: Vol. 29 No. 2 (2009)
- Paola Andrea Rueda , Sara Orozco , Juan Raúl Castro , Ángela María Londoño, Elsa María Vásquez, Andrea Arango, Carlos Esteban Builes , Incidence and prevalence of vitiligo by gender and age in the Colombian population , Biomedica: Vol. 45 No. 4 (2025)
- Rosa Magdalena Uscátegui, Adriana M. Correa, Jaime Carmona-Fonseca, Changes in retinol, hemoglobin and ferritin concentrations in Colombian children with malaria , Biomedica: Vol. 29 No. 2 (2009)
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |
Funding data
-
Departamento Administrativo de Ciencia, Tecnología e Innovación (COLCIENCIAS)
Grant numbers Convocatoria para Proyectos de Ciencia, Tecnología e Innovación en Salud 2017 Project ID 1115-777-57608

























