Severe pediculosis capitis in a nursery school girl
Abstract
Pediculosis capitis is the most frequent ectoparasitosis around the world. The infestation is caused by Pediculus humanus capitis (head louse), which affects hair, scalp, and skin.
It rarely presents with more symptoms and in the majority of the cases, it shows a benign course if treated properly.
We present the case of a nursery school girl with head lice infestation for 18 months. She did not improve after the shampoo treatment. This case was associated with furunculosis, skin lesions, multiple adenopathies, and anemia.
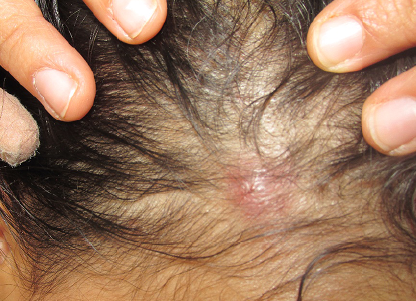
Initially, the presence of boils, alopecia, and lymphadenopathy was evident. The persistence of pediculosis capitis and intense scratching induced changes on skin integrity, facilitating opportunistic bacterial superinfection that led to impetiginization, furunculosis, excoriations, hematic scabs, anemia, alopecia, and lymphadenopathies. Pediculosis capitis affected the patient triggering psychological, economic, social, and other health problems.
The patient presented uncommon symptoms (furunculosis, anemia, fever, alopecia, and adenopathies) resulting from the persistence of risk factors and the absence of head inspection and mechanical removal of insects. The education about the risk factors, as well as sanitary controls, are essential to contain the infestation.
Downloads
References
Feldmeier H. Pediculosis capitis: New insights into epidemiology, diagnosis and treatment. Eur J Clin Microbiol Infect Dis. 2012;31:2105-10. https://doi.org/10.1007/s10096-012-1575-0
Bonilla DL, Durden LA, Eremeeva ME, Dasch GA. The biology and taxonomy of head and body lice—implications for louse-borne disease prevention. PLoS Pathog. 2013;9:e1003724. https://doi.org/10.1371/journal.ppat.1003724
Doroodgar A, Sadr F, Doroodgar M, Doroodgar M, Sayyah M. Examining the prevalence rate of Pediculus capitis infestation according to sex and social factors in primary school children. Asian Pacific J Trop Dis. 2014;4:25-9. https://doi.org/10.1016/S2222-1808(14)60308-X
Moncada LI, Ríos SM, Fernández JA, Rivas F, Sáenz ML. Prevalencia y factores asociados a la pediculosis en niños de un jardín infantil de Bogotá. Biomédica. 2008;28:245-51. https://doi.org/10.7705/biomedica.v28i2.95
López-Valencia D, Medina-Ortega A, Vásquez-Arteaga L. Prevalence and variables associated with pediculosis capitis in kindergarten children from Popayán, Colombia. Revista de la Facultad de Medicina. 2017;65:425-8. https://doi.org/10.15443/revfacmed.v65.n3.58812
Meister L, Ochsendorf F. Head lice: Epidemiology, biology, diagnosis, and treatment. Dtsch Arztebl Int. 2016;113:763-72. https://doi.org/10.3238/arztebl.2016.0763
Madke B, Khopkar U. Pediculosis capitis: An update. Indian J Dermatol Venereol Leprol. 2012;78:429-38. https://doi.org/10.4103/0378-6323.98072
Amanzougaghene N, Fenollar F, Sangaré AK, Sissoko MS, Doumbo OK, Raoult D, et al. Detection of bacterial pathogens including potential new species in human head lice from Mali. PLoS One. 2017;12:e0184621. https://doi.org/10.1371/journal.pone.0184621
Connor CJ, Selby JC, Wanat KA. Severe pediculosis capitus: A case of “crusted lice” with autoeczematization. Dermatol Online J. 2016;22.
Ko CJ, Elston DM. Pediculosis. J Am Acad Dermatol. 2004;50:1-4. https://doi.org/10.1016/S0190-9622(03)02729-4
Jahnke C, Bauer E, Hengge UR, Feldmeier H. Accuracy of diagnosis of pediculosis capitis: Visual inspection vs wet combing. Arch Dermatol. 2009;145:309-13. https://doi.org/10.1001/archdermatol.2008.587
Frankowski BL, Bocchini JA. Clinical report—head lice. Pediatrics. 2010;126:392-403. https://doi.org/10.1542/peds.2010-1308
Driscoll DM, Tronic B. Pediculosis capitis. N Engl J Med. 1996;335:790. https://doi.org/10.1056/NEJM199609123351105
Rodríguez-Fernández R, Gómez-Campderá J. Pediculosis en la infancia. Acta Pediatr Esp. 2006;64:419-24.
Hall RR, McMichael AJ. Circumscribed alopecia: An unusual manifestation of pediculosis capitis. Pediatr Dermatol. 2012;29:513-4. https://doi.org/10.1111/j.1525-1470.2011.01596.x
Speare R, Canyon D V, Melrose W. Quantification of blood intake of the head louse: Pediculus humanus capitis. Int J Dermatol. 2006;45:543-6. https://doi.org/10.1111/j.1365-4632.2005.02520.x
Guss DA, Koenig M, Castillo EM. Severe iron deficiency anemia and lice infestation. J Emerg Med. 2011;41:362-5. https://doi.org/10.1016/j.jemermed.2010.05.030
Hau V, Muhi-Iddin N. A ghost covered in lice: A case of severe blood loss with long-standing heavy pediculosis capitis infestation. BMJ Case Rep. 2014;2014. https://doi.org/10.1136/bcr-2014-206623
López-Valencia D, Medina-Ortega A, Mosquera-Monje S, Vásquez-Arteaga L. Actualización y perspectiva integrada de la pediculosis. Rev Asoc Colomb Dermatol. 2017;25:38-48.
Ponce-García G, Villanueva-Segura K, Trujillo-Rodríguez G, Rodríguez-Sánchez IP, López-Monroy B, Flores AE. First detection of the Kdr mutation T929I in head lice (Phthiraptera: Pediculidae) in schoolchildren of the Metropolitan Area of Nuevo León and Yucatán, México. J Med Entomol. 2017;54:1025-30. https://doi.org/10.1093/jme/tjx045
Gellatly KJ, Krim S, Palenchar DJ, Shepherd K, Yoon KS, Rhodes CJ, et al. Expansion of the knockdown resistance frequency map for human head lice (Phthiraptera: Pediculidae) in the United States using quantitative sequencing. J Med Entomol. 2016;53:653-9. https://doi.org/10.1093/jme/tjw023
Some similar items:
- Elizabeth Borrero, Gabriel Carrasquilla, Neal Alexander, Decentralization and health system reform: What is their impact on malaria incidence in Colombian municipalities? , Biomedica: Vol. 32 (2012): Suplemento 1, Malaria
- Margarita Arboleda, María Fernanda Pérez, Diana Fernández, Luz Yaned Usuga, Miler Meza, Clinical and laboratory profile of Plasmodium vivax malaria patients hospitalized in Apartadó, , Biomedica: Vol. 32 (2012): Suplemento 1, Malaria
- Rosa Magdalena Uscátegui, Adriana M. Correa, Jaime Carmona-Fonseca, Changes in retinol, hemoglobin and ferritin concentrations in Colombian children with malaria , Biomedica: Vol. 29 No. 2 (2009)
- Myrtha Arango, Elizabeth Castañeda, Clara Inés Agudelo, Catalina De Bedout, Carlos Andrés Agudelo, Angela Tobón, Melva Linares, Yorlady Valencia, Ángela Restrepo, The Colombian Histoplasmosis Study Group, Histoplasmosis: results of the Colombian National Survey, 1992-2008 , Biomedica: Vol. 31 No. 3 (2011)
- Jairo Echeverry, Carlos Mauricio Hurtado, Myriam Gutiérrez, Clinical manifestations of lead levels in children exposed to automobile battery recycling processes in Soacha and Bogotá, D.C. , Biomedica: Vol. 28 No. 1 (2008)
- Sandra Lorena Girón, Julio César Mateus, Fabián Méndez, Impact of an open waste disposal site on the occurrence of respiratory symptoms and on health care costs of children , Biomedica: Vol. 29 No. 3 (2009)
- José Joaquín Carvajal, Ligia Inés Moncada, Mauricio Humberto Rodríguez, Ligia del Pilar Pérez, Víctor Alberto Olano, Characterization of Aedes albopictus (Skuse, 1894) (Diptera:Culicidae) larval habitats near the Amazon River in Colombia , Biomedica: Vol. 29 No. 3 (2009)
- Patricia Escobar, Katherine Paola Luna, Indira Paola Hernández, César Mauricio Rueda, María Magdalena Zorro, Simon L. Croft, In vitro susceptibility of Trypanosoma cruzi strains from Santander, Colombia, to hexadecylphosphocholine (miltefosine), nifurtimox and benznidazole , Biomedica: Vol. 29 No. 3 (2009)
- Gustavo Pradilla, Julio César Mantilla, Reynaldo Badillo, Human rabies encephalitis by a vampire bat bite in an urban area of Colombia , Biomedica: Vol. 29 No. 2 (2009)
- Mauricio Beltrán, María Cristina Navas, María Patricia Arbeláez, Jorge Donado, Sergio Jaramillo, Fernando De la Hoz, Cecilia Estrada, Lucía del Pilar Cortés, Amalia de Maldonado, Gloria Rey, Seroprevalence of hepatitis B virus and human immunodeficiency virus infection in a population of multiply-transfused patients in Colombia , Biomedica: Vol. 29 No. 2 (2009)
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























