Rhino-orbito-cerebral mucormycosis from dental origin: Case report
Abstract
Rhino-orbito-cerebral mucormycosis from dental origin is an acute infection caused by opportunistic fungi belonging to the order of Mucorales, which affects mainly diabetic and immunocompromised patients.
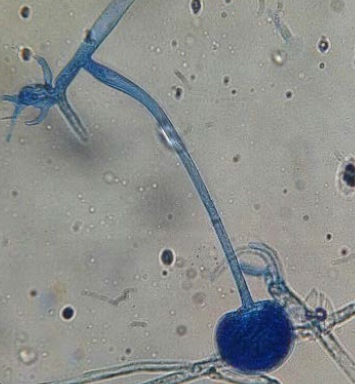
We report the case of a 63-year old diabetic man who performed a dental extraction on himself by his own means and subsequently developed a rhino-orbito-cerebral mucormycosis with cutaneous and palatal affection. The species isolated in the mycological culture was Rhizopus sp.
Downloads
References
Bonifaz A. Mucormicosis y entomoftoromicosis (zigomicosis). En: Micología médica básica. Cuarta edición. México, D.F.: McGraw-Hill; 2012. p. 399-415.
Bonifaz A, Barrón T, Collazo-Jaloma J. Zigomicosis (mucormicosis) cutánea en paciente con leucemia. Actas Dermosifiliogr. 2002;93:514-7.
Bonifaz A, Macías B, Paredes-Farrera F, Arias P, Ponce RM, Araiza J. Palatal zygomycosis: Experience of 21 cases. Oral Dis. 2008;14:569-74. https://doi.org/10.1111/j.1601-0825.2007.01433.x
Idoko KE, Gómez I. Rhinocerebral mucormycosis in an inpatient with acquired immunodeficiency syndrome: A complication of therapy. Infect Dis Clin Pract. 2011;19:431-2. https://doi.org/10.1097/IPC.0b013e31820a530b
Mahadevia P, Brandwein-Gensler M. Infectious diseases of the head and neck. En: Barnes L, editor. Surgical pathology of the head and neck. Third edition. New York: Informa Healthcare; 2009. p. 1609-715.
Khatiwada P, Giri A, Khatiwoda P. Mucormycosis in diabetes mellitus. Journal of Advances in Internal Medicine. 2012;1:73-5. https://doi.org/10.3126/jaim.v1i2.6531
Gale GR, Welch AM. Studies of opportunistic fungi. Am J Med Sci. 1961;241:604-12. https://doi.org/10.1097/00000441-196105000-00008
Ribes JA, Vanover-Sams CL, Baker DJ. Zygomycetes in human disease. Clin Microbiol Rev. 2000;13:236-301. https://doi.org/10.1128/CMR.13.2.236-301.2000
Ibrahim AS, Spellberg B, Edwards J Jr. Iron acquisition: A novel prospective on mucormycosis: Pathogenesis and treatment. Curr Opin Infect Dis. 2008;21:620-5. https://doi.org/10.1097/QCO.0b013e3283165fd1
Kim J, Forston J, Cook H. A fatal outcome from rhinocerebral mucormycosis after dental extractions: A case report. J Oral Maxillofac Surg. 2001;59:693-7. https://doi.org/10.1053/joms.2001.23407
Pandey A, Bansal V, Asthana AK, Trivedi V, Madan M, Das A. Maxillary osteomyelitis by mucormycosis: Report of four cases. Int J Infect Dis. 2011;15:66-9. https://doi.org/10.1016/j.ijid.2010.09.003
Scheckenbach K, Cornely O, Hoffmann TK, Engers R, Bier H, Chaker A, et al. Emerging therapeutic options in fulminant invasive rhinocerebral mucormycosis. Auris Nasus Larynx. 2010;37:322-8. https://doi.org/10.1016/j.anl.2009.09.001
Mimouni O, Curto L, Danvin B, Thomassin M, Dessi P. Sinonasal mucormycosis: Case report. Eur Ann Otorhinolaryngol Head Neck Dis. 2010;127:27-9. https://doi.or/10.1016/j.anorl.2010.02.007
Arnáiz ME, Alonso D, González MC, García JD, Sanz JR, Arnáiz AM. Cutaneous mucormycosis: Report of five cases and review of the literature. J Plast Reconstr Aesthet Surg. 2009;62:434-41. https://doi.org/10.1016/j.bjps.2008.04.040
PatilPM, Bhadani P. Extensive maxillary necrosis following tooth extraction. J Oral Maxillofac Surg. 2011;69:2387-91. https://doi.org/10.1016/j.joms.2010.11.018
Viterbo S, Fasolis M, Garzino-Demo P, Griffa A, Boffano P, Laquinta C, et al. Management and outcomes of three cases of rhinocerebral mucormycosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112:69-74. https://doi.org/10.1016/j.tripleo.2011.04.048
O’Neill BM, Alessi AS, George EB, Piro J. Disseminated rhinocerebral mucormycosis: A case report and review of the literature. J Oral Maxillofacial Surg. 2006;64:326-33.
https://doi.org/10.1016/j.joms.2005.10.017
Pía W, Spalloni M, Glaser S, Verdugo P. Mucormicosis rinocerebral: sobrevida en un niño con leucemia. Rev Chil Infect. 2004;21:53-6. https://doi.org/10.4067/S0716-10182004000100007
Rangel RA, Martínez HR, Sáenz C, Bosques F, Estrada I. Rhinocerebral and systemic mucormycosis: Clinical experience with 36 cases. J Neurol Sci. 1996;143:19-30. https://doi.org/10.1016/S0022-510X(96)00148-7
Won-Suk OH, Roumanas E. Dental implant-assisted prosthetic rehabilitation of a patient with a bilateral maxillectomy defect secondary to mucormycosis. J Prosthet Dent. 2006;96:88-95. https://doi.org/10.1016/j.prosdent.2006.05.004
Jung SH, Kim SW, Park ChS, Song ChE, Cho JH, Lee JH, et al. Rhinocerebral mucormycosis: Consideration of prognostic factors and treatment modality. Auris Nasus Larynx. 2009;36:274-9. https://doi.org/10.1016/j.anl.2008.07.003
Some similar items:
- Juan Manuel Senior, Clara Saldarriaga, Endocarditis due to infection by Paecilomyces variotii , Biomedica: Vol. 29 No. 2 (2009)
- Carolina Firacative, Germán Torres, María Claudia Rodríguez, Patricia Escandón, First environmental isolation of Cryptococcus gattii serotype B, from Cúcuta, Colombia , Biomedica: Vol. 31 No. 1 (2011)
- Beatriz Montes, Angela Restrepo, Juan G. McEwen, New fungal classification and their applications in medicine. , Biomedica: Vol. 23 No. 2 (2003)
- John Fredy Nieto-Ríos, Douglas Ramón Villafañe-Bermúdez, Gustavo Adolfo Guerrero-Tinoco, Isabel Cristina Ramírez-Sánchez, Lina María Serna-Higuita, Arbey Aristizábal-Alzate, Catalina Ocampo-Kohn, Gabriel Varela, Gustavo Zuluaga-Valencia, Brain abscess caused by Cladophialophora bantiana after renal allograft loss: A case report , Biomedica: Vol. 39 No. Supl. 2 (2019): Enfermedades transmisibles en el trópico, agosto
- Jorge Alberto Cortés, José Franklin Ruiz, Lizeth Natalia Melgarejo-Moreno, Elkin V. Lemos, Candidemia in Colombia , Biomedica: Vol. 40 No. 1 (2020)
- María Alejandra Pérez, Luisa Martínez, Juan Bravo, Brenda Rodríguez, Paola Quintero , Pablo Moncada, Infection due to Aspergillus flavus and Rhizopus oryzae complex in a patient with diabetes mellitus , Biomedica: Vol. 43 No. 1 (2023)
- Beatriz L. Gómez, Patricia Escandón, Fungal infections: A growing threat , Biomedica: Vol. 43 No. Sp. 1 (2023): Agosto, Micología médica
- Lina M. Osorio-Cock, Sandra Catalina Jaramillo-Pulgarín, Alba P. Ferrín-Bastidas, Diana Y. Molina-Colorado, Óscar M. Gómez-Guzmán, Alejandra Zuluaga, Juan G. McEwen-Ochoa, Martha E. Urán-Jiménez, María del Pilar Jiménez-Alzate, Pseudoepitheliomatous hyperplasia: Squamous cell carcinoma versus oral paracoccidioidomycosis, a case from a dermatological perspective , Biomedica: Vol. 43 No. Sp. 1 (2023): Agosto, Micología médica
- Daniel F. Q Smith, Arturo Casadevall, Disaster mycology , Biomedica: Vol. 43 No. Sp. 1 (2023): Agosto, Micología médica
- Patricia Escandón, Shawn R. Lockhart, Nancy A. Chow, Tom M. Chiller, Candida auris: a global pathogen that has taken root in Colombia , Biomedica: Vol. 43 No. Sp. 1 (2023): Agosto, Micología médica
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























