Reconociendo el virus del chikunguña
Resumen
El virus de chikunguña (CHIKV) es un Alfavirus perteneciente al grupo denominado del Viejo Mundo; estos son virus artritogénicos que causan una enfermedad febril caracterizada por artralgias y mialgias. Aunque la muerte por CHIKV es poco frecuente, la enfermedad puede llegar a ser incapacitante y generar un amplio espectro de manifestaciones atípicas, como complicaciones cardiovasculares, respiratorias, oculares, renales y dérmicas, entre otras. Cuando el dolor articular persiste por tres o más meses, da lugar a la forma crónica de la enfermedad denominada reumatismo inflamatorio crónico poschikunguña, el cual es la principal secuela de la enfermedad. Se considera que este virus no es neurotrópico, sin embargo, puede afectar el sistema nervioso central y generar secuelas graves y permanentes, principalmente, en niños y ancianos.
En África, Asia y Europa se habían reportado anteriormente brotes epidémicos por CHIKV, pero solo hasta finales del 2013 se documentó la introducción del virus a las Américas; desde entonces, el virus se ha propagado a 45 países o territorios del continente y el número de casos acumulados ascendió a cerca de dos millones en dos años.
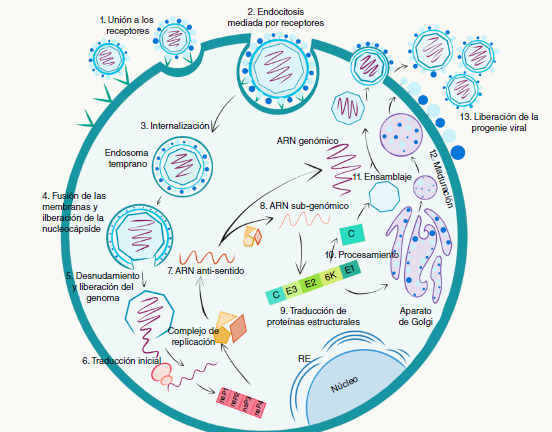
Esta revisión describe de manera general la biología molecular del virus, sus manifestaciones clínicas, su patogénesis y las principales complicaciones posteriores a la infección. Además, reúne la información de la epidemia en Colombia y el continente americano publicada entre el 2014 y el 2020.
Descargas
Referencias bibliográficas
Her Z, Kam Y, Lin R, Ng L. Chikungunya: A bending reality. Microbes Infect. 2009;11:1165-76. https://doi.org/10.1016/j.micinf.2009.09.004
Wahid B, Ali A, Rafique S, Idrees M. Global expansion of chikungunya virus: Mapping the 64-year history. Int J Infect Dis. 2017;58:69-76. https://doi.org/10.1016/j.ijid.2017.03.006
Cassadou S, Boucau S, Petit-Sinturel M, Huc P, Leparc-Goffart I, Ledrans M. Emergence of chikungunya fever on the French side of Saint Martin island, October to December 2013. Eurosurveillance. 2014;19:20752. https://doi.org/10.2807/1560-7917.ES2014.19.13.20752
Organización Mundial de la Salud. Número de casos reportados de chikungunya en países o territorios de las Américas 2017 (por semanas) Semana Epidemiológica / SE 50
(actualizada al 15 de diciembre de 2017); 2017. Fecha de consulta: 1 de agosto de 2018. Disponible en: https://www.paho.org/hq/dmdocuments/2017/2017-dic-15-phe-CHIKV-casosse-50.pdf
Higgs S, Vanlandingham D. Chikungunya virus and its mosquito vectors. Vector-Borne Zoonotic Dis. 2015;15:231-40. https://doi.org/10.1089/vbz.2014.1745
Carvalho R, Lourenço-De-Oliveira R, Braga I. Updating the geographical distribution and frequency of Aedes albopictus in Brazil with remarks regarding its range in the Americas. Mem Inst Oswaldo Cruz. 2014;109:787-96. https://doi.org/10.1590/0074-0276140304
Schilte C, Staikowsky F, Couderc T, Madec Y, Carpentier F, Kassab S, et al. Chikungunya virus-associated long-term arthralgia: A 36-month prospective longitudinal study. PLoS Negl Trop Dis. 2013;7:e2137. https://doi.org/10.1371/journal.pntd.0002137
Javelle E, Ribera A, Degasne I, Gaüzère B-A, Marimoutou C, Simon F. Specific management of post-chikungunya rheumatic disorders: A retrospective study of 159 cases in Reunion Island from 2006-2012. PLoS Negl Trop Dis. 2015;9:e0003603. https://doi.org/10.1371/journal.pntd.0003603
Economopoulou A, Domínguez M, Helynck B, Sissoko D, Wichmann O, Quenel P, et al. Atypical Chikungunya virus infections: Clinical manifestations, mortality and risk factors for severe disease during the 2005-2006 outbreak on Réunion. Epidemiol Infect. 2009;137:534-41. https://doi.org/10.1017/S0950268808001167
Badawi A, Ryoo S, Vasileva D, Yaghoubi S. Prevalence of chronic comorbidities in chikungunya: A systematic review and meta-analysis. Int J Infect Dis. 2018;67:107-13. https://doi.org/10.1016/j.ijid.2017.12.018
Powers A, Brault A, Shirako Y, Strauss E, Kang W, Strauss J, et al. Evolutionary relationships and systematics of the alphaviruses. J Virol. 2001;75:10118-31. https://doi.org/10.1128/JVI.75.21.10118-10131.2001
Kulasegaran-Shylini R, Thiviyanathan V, Gorenstein DG, Frolov I. The 5′UTR-specific mutation in VEEV TC-83 genome has a strong effect on RNA replication and subgenomic RNA synthesis, but not on translation of the encoded proteins. Virology. 2009;387:211-21. https://doi.org/10.1016/j.virol.2009.02.027
Volk S, Chen R, Tsetsarkin K, Adams A, García T, Sall A, et al. Genome-scale phylogenetic analyses of chikungunya virus reveal independent emergences of recent epidemics and various evolutionary rates. J Virol. 2010;84:6497-504. https://doi.org/10.1128/JVI.01603-09
Vairo F, Haider N, Kock R, Ntoumi F, Ippolito G, Zumla A. Chikungunya: Epidemiology, pathogenesis, clinical features, management, and prevention. Infect Dis Clin North Am. 2019;33:1003-25. https://doi.org/10.1016/j.idc.2019.08.006
Arankalle V, Shrivastava S, Cherian S, Gunjikar R, Walimbe A, Jadhav S, et al. Genetic divergence of Chikungunya viruses in India (1963-2006) with special reference to the 2005-2006 explosive epidemic. J Gen Virol. 2007;88:1967-76. https://doi.org/10.1099/vir.0.82714-0
Rezza G, Nicoletti L, Angelini R, Romi R, Finarelli A, Panning M, et al. Infection with chikungunya virus in Italy: An outbreak in a temperate region. Lancet. 2007;370:1840-46. https://doi.org/10.1016/S0140-6736(07)61779-6
Grandadam M, Caro V, Plumet S, Thiberge J, Souarès Y, Failloux A, et al. Chikungunya virus, southeastern France. Emerg Infect Dis. 2011;17:910-13. https://doi.org/10.3201/eid1705.101873
Schuffenecker I, Iteman I, Michault A, Murri S, Frangeul L, Vaney MC, et al. Genome microevolution of chikungunya viruses causing the Indian Ocean outbreak. PLoS Med. 2006;3:e263. https://doi.org/10.1371/journal.pmed.0030263
Hapuarachchi HC, Bandara KB, Sumanadasa SD, Hapugoda MD, Lai YL, Lee KS, et al. Re-emergence of Chikungunya virus in South-east Asia: Virological evidence from Sri Lanka and Singapore. J Gen Virol. 2010;91:1067-76. https://doi.org/10.1099/vir.0.015743-0
Tsetsarkin KA, Vanlandingham DL, McGee CE, Higgs S. A single mutation in chikungunya virus affects vector specificity and epidemic potential. PLoS Pathog. 2007;3:e201. https://doi.org/10.1371/journal.ppat.0030201
Sahadeo NSD, Allicock OM, De Salazar PM, Auguste AJ, Widen S, Olowokure B, et al. Understanding the evolution and spread of chikungunya virus in the Americas using complete genome sequences. Virus Evol. 2017;3:vex010. https://doi.org/10.1093/VE/VEX010
Leparc-Goffart I, Nougairede A, Cassadou S, Prat C, de Lamballerie X. Chikungunya in the Americas. Lancet. 2014;383:514. https://doi.org/10.1016/S0140-6736(14)60185-9
Tan Y, Pickett BE, Shrivastava S, Gresh L, Balmaseda A, Amedeo P, et al. Differing epidemiological dynamics of Chikungunya virus in the Americas during the 2014-2015 epidemic. PLoS Negl Trop Dis. 2018;12:e0006670. https://doi.org/10.1371/journal.pntd.0006670
Stapleford KA, Moratorio G, Henningsson R, Chen R, Matheus S, Enfissi A, et al. Wholegenome sequencing analysis from the Chikungunya virus Caribbean outbreak reveals novel evolutionary genomic elements. PLoS Negl Trop Dis. 2016;10:e0004402. https://doi.org/10.1371/journal.pntd.0004402
Rupp JC, Sokoloski KJ, Gebhart NN, Hardy RW. Alphavirus RNA synthesis and non-structural protein functions. J Gen Virol. 2015;96:2483-500. https://doi.org/10.1099/jgv.0.000249
Lulla V, Kim DY, Frolova EI, Frolov I. The amino-terminal domain of alphavirus capsid protein is dispensable for viral particle assembly but regulates RNA encapsidation through cooperative functions of its subdomains. J Virol. 2013;87:12003-19. https://doi.org/10.1128/JVI.01960-13
Soonsawad P, Xing L, Milla E, Espinoza JM, Kawano M, Marko M, et al. Structural evidence of glycoprotein assembly in cellular membrane compartments prior to Alphavirus budding. J Virol. 2010;84:11145-51. https://doi.org/10.1128/jvi.00036-10
Yap ML, Klose T, Urakami A, Hasan SS, Akahata W, Rossmann MG. Structural studies of Chikungunya virus maturation. Proc Natl Acad Sci USA. 2017;114:13703-07. https://doi.org/10.1073/pnas.1713166114
Ramsey J, Mukhopadhyay S. Disentangling the frames, the state of research on the alphavirus 6K and TF proteins. Viruses. 2017;9:228. https://doi.org/10.3390/v9080228
Wintachai P, Wikan N, Kuadkitkan A, Jaimipuk T, Ubol S, Pulmanausahakul R, et al. Identification of prohibitin as a Chikungunya virus receptor protein. J Med Virol. 2012;84:1757-70. https://doi.org/10.1002/jmv.23403
Moller-Tank S, Kondratowicz AS, Davey RA, Rennert PD, Maury W. Role of the phosphatidylserine receptor TIM-1 in enveloped-virus entry. J Virol. 2013;87:8327-41. https://doi.org/10.1128/jvi.01025-13
Silva LA, Khomandiak S, Ashbrook AW, Weller R, Heise MT, Morrison TE, et al. A single-amino-acid polymorphism in Chikungunya virus E2 glycoprotein influences glycosaminoglycan utilization. J Virol. 2014;88:2385-97. https://doi.org/10.1128/jvi.03116-13
Zhang R, Kim AS, Fox JM, Nair S, Basore K, Klimstra WB, et al. Mxra8 is a receptor for multiple arthritogenic alphaviruses. Nature. 2018;557:570-4. https://doi.org/10.1038/s41586-018-0121-3
van Duijl-Richter MK, Hoornweg TE, Rodenhuis-Zybert IA, Smit JM. Early events in Chikungunya virus infection-from virus cell binding to membrane fusion. Viruses. 2015;7:3647-74. https://doi.org/10.3390/v7072792
Uchime O, Fields W, Kielian M. The role of E3 in pH protection during alphavirus assembly and exit. J Virol. 2013;87:10255-62. https://doi.org/10.1128/JVI.01507-13
Ozden S, Huerre M, Riviere J-P, Coffey L, Afonso P, Mouly V, et al. Human muscle satellite cells as targets of Chikungunya virus infection. PLoS ONE. 2007;2:e527. https://doi.org/10.1371/journal.pone.0000527
Sharp T, Keating MK, Shieh W-J, Bhatnagar J, Bollweg B, Levine R, et al. Clinical characteristics, histopathology, and tissue immunolocalization of chikungunya virus antigen in fatal cases. Clin Infect Dis. 2020;ciaa837. https://doi.org/10.1093/cid/ciaa837
Morrison TE, Oko L, Montgomery SA, Whitmore AC, Lotstein AR, Gunn BM, et al. A mouse model of chikungunya virus-induced musculoskeletal inflammatory disease: Evidence of arthritis, tenosynovitis, myositis, and persistence. Am J Pathol. 2011;178:32-40. https://doi.org/10.1016/j.ajpath.2010.11.018
Issac TH, Tan EL, Chu JJ. Proteomic profiling of chikungunya virus-infected human muscle cells: Reveal the role of cytoskeleton network in CHIKV replication. J Proteomics. 2014;108:445-64. https://doi.org/10.1016/J.JPROT.2014.06.003
Hussain KM, Lee RC, Ng MM, Chu JJ. Establishment of a novel primary human skeletal myoblast cellular model for chikungunya virus infection and pathogenesis. Sci Rep. 2016;6:21406. https://doi.org/10.1038/srep21406
Couderc T, Chrétien F, Schilte C, Disson O, Brigitte M, Guivel-Benhassine F, et al. A mouse model for Chikungunya: Young age and inefficient type-I interferon signaling are risk factors for severe disease. PLoS Pathog. 2008;4:e29. https://doi.org/10.1371/journal.ppat.0040029
Labadie K, Larcher T, Joubert C, Mannioui A, Delache B, Brochard P, et al. Chikungunya disease in nonhuman primates involves long-term viral persistence in macrophages. J Clin Invest. 2010;120:894-906. https://doi.org/10.1172/JCI40104
Wikan N, Sakoonwatanyoo P, Ubol S, Yoksan S, Smith DR. Chikungunya virus infection of cell lines: Analysis of the East, Central and South African lineage. PLoS ONE. 2012;7:e31102. https://doi.org/10.1371/journal.pone.0031102
Zhang X, Huang Y, Wang M, Yang F, Wu C, Huang D, et al. Differences in genome characters and cell tropisms between two chikungunya isolates of Asian lineage and Indian Ocean lineage. Virol J. 2018;15:130. https://doi.org/10.1186/s12985-018-1024-5
Kashyap RS, Morey SH, Chandak NH, Purohit HJ, Taori GM, Daginawala HF. Detection of viral antigen, IgM and IgG antibodies in cerebrospinal fluid of Chikungunya patients with neurological complications. Cerebrospinal Fluid Res. 2010;7:12. https://doi.org/10.1186/1743-8454-7-12
Das T, Jaffar-Bandjee MC, Hoarau JJ, Trotot PK, Denizot M, Lee-Pat-Yuen G, et al. Chikungunya fever: CNS infection and pathologies of a re-emerging arbovirus. Prog Neurobiol. 2010;91:121-9. https://doi.org/10.1016/J.PNEUROBIO.2009.12.006
Fraisier C, Koraka P, Belghazi M, Bakli M, Granjeaud S, Pophillat M, et al. Kinetic analysis of mouse brain proteome alterations following Chikungunya virus infection before and after appearance of clinical symptoms. PLoS ONE. 2014;9:e91397. https://doi.org/10.1371/journal.pone.0091397
Her Z, Malleret B, Chan M, Ong E, Wong S, Kwek D, et al. Active infection of human blood monocytes by Chikungunya virus triggers an innate immune response. J Immunol. 2010;184:5903-13. https://doi.org/10.4049/jimmunol.0904181
Teng T-S, Foo S-S, Simamarta D, Lum F-M, Teo T-H, Lulla A, et al. Viperin restricts chikungunya virus replication and pathology. J Clin Invest. 2012;122:4447-60. https://doi.org/10.1172/JCI63120
Thiberville S, Boisson V, Gaudart J, Simon F, Flahault A, de Lamballerie X. Chikungunya fever: A clinical and virological investigation of outpatients on Réunion Island, South-West Indian Ocean. PLoS Negl Trop Dis. 2013;7:e2004. ttps://doi.org/10.1371/journal.pntd.0002004
Hua C, Combe B. Chikungunya virus-associated disease. Curr Rheumatol Rep. 2017;19:69. https://doi.org/10.1007/s11926-017-0694-0
Rodríguez-Morales AJ, Cardona-Ospina JA, Urbano-Garzón SF, Hurtado-Zapata JS. Prevalence of post-Chikungunya infection chronic inflammatory arthritis: A systematic review and meta-analysis. Arthritis Care Res. 2016;68:1849-58. https://doi.org/10.1002/acr.22900
Edington F, Varjão D, Melo P. Incidence of articular pain and arthritis after chikungunya fever in the Americas: A systematic review of the literature and meta-analysis. Jt Bone Spine. 2018;85:669-78. https://doi.org/10.1016/j.jbspin.2018.03.019
Hoarau JJ, Jaffar-Bandjee MC, Krejbich-Trotot P, Das T, Li-Pat-Yuen G, Dassa B, et al. Persistent chronic inflammation and infection by Chikungunya arthritogenic alphavirus in spite of a robust host immune response. J Immunol. 2010;184:5914-27. https://doi.org/10.4049/jimmunol.0900255
Chow A, Her Z, Ong EK, Chen J, Dimatatac F, Kwek D, et al. Persistent arthralgia induced by Chikungunya virus infection is associated with interleukin-6 and granulocyte macrophage colony-stimulating factor. J Infect Dis. 2011;203:149-57. https://doi.org/10.1093/infdis/jiq042
Poo YS, Rudd PA, Gardner J, Wilson J, Larcher T, Colle M-A, et al. Multiple immune factors are involved in controlling acute and chronic Chikungunya virus infection. PLoS Negl Trop Dis. 2014;8:e3354. https://doi.org/10.1371/journal.pntd.0003354
Pinto JR, da Silva Junior GB, Mota RMS, Martins P, Santos A, de Moura DC, et al. Clinical profile and factors associated with hospitalizatin during a Chikungunya epidemic in Ceará, Brazil. Rev Soc Bras Med Trop. 2019;52:57:e20190167. https://doi.org/10.1590/0037-8682-0167-2019
Rollé A, Schepers K, Cassadou S, Madeux B, Hermann-Storck C, Fabre I, et al. Severe sepsis and septic shock associated with chikungunya virus infection, Guadeloupe, 2014. Emerg Infect Dis. 2016;22:891-94. https://doi.org/10.3201/eid2205.151449
Dorléans F, Hoen B, Najioullah F, Herrmann-Storck C, Schepers K, Abel S, et al. Outbreak of chikungunya in the French Caribbean islands of Martinique and Guadeloupe: Findings from a hospital-based surveillance system (2013-2015). Am J Trop Med Hyg. 2018;98:1819-25. https://doi.org/10.4269/ajtmh.16-0719
Danis-Lozano R, Díaz-González EE, Trujillo-Murillo K del C, Caballero-Sosa S, Sepúlveda-Delgado J, Malo-García I, et al. Clinical characterization of acute and convalescent illness of confirmed chikungunya cases from Chiapas, S. Mexico: A cross sectional study. PLoS ONE. 2017;12:e0186923. https://doi.org/10.1371/journal.pone.0186923
Galán-Huerta KA, Martínez-Landeros E, Delgado-Gallegos JL, Caballero-Sosa S, Malo-García I, Fernández-Salas I, et al. Molecular and clinical characterization of Chikungunya virus infections in Southeast México. Viruses. 2018;10:248. https://doi.org/10.3390/v10050248
Hsu CH, Cruz-López F, Vargas-Torres D, Pérez-Padilla J, Lorenzi O, Rivera A, et al. Risk factors for hospitalization of patients with chikungunya virus infection at sentinel hospitals in Puerto Rico. PLoS Negl Trop Dis. 2019;13:e0007084. https://doi.org/10.1371/journal.pntd.0007084
Torres JR, Códova L, Castro JS, Rodríguez L, Saravia V, Arvelaez J, et al. Chikungunya fever: Atypical and lethal cases in the Western hemisphere: A Venezuelan experience. IDCases. 2015;2:6-10. https://doi.org/10.1016/j.idcr.2014.12.002
Torres JR, Córdova L, Saravia V, Arvelaez J, Castro JS. Nasal skin necrosis: An unexpected new finding in severe Chikungunya fever. Clin Infect Dis. 2016;62:78-81. https://doi.org/10.1093/cid/civ718
Rueda JC, Santos AM, Angarita JI, Giraldo R, Saldarriaga E-L2, Ballesteros J, et al. Demographic and clinical characteristics of chikungunya patients from six Colombian cities, 2014-2015. Emerg Microbes Infect. 2019;8:1490-500. https://doi.org/10.1080/22221751.2019.1678366
Calvo EP, Coronel-Ruiz C, Velazco S, Velandia-Romero M, Castellanos JE. Diagnóstico diferencial de dengue y chikungunya en pacientes pediátricos. Biomédica. 2015;36:35-3. https://doi.org/10.7705/biomedica.v36i0.2982
Raad JJ, Rosero AS, Martínez JV, Parodye A, Raadf RJ, Caballero D, et al. Respuesta inmunitaria de una población del caribe colombiano infectada con el virus chikungunya. Rev Colomb Reumatol. 2016;23:85-91. https://doi.org/10.1016/j.rcreu.2016.03.003
Mercado M, Acosta-Reyes J, Parra E, Guzmán L, Beltrán M, Gasque P, et al. Renal involvement in fatal cases of chikungunya virus infection. J Clin Virol. 2018;103:16-8. https://doi.org/10.1016/J.JCV.2018.03.009
De la Hoz JM , Bayona B, Viloria S, Accini JL, Juan-Vergara HS, Viasus D. Fatal cases of Chikungunya virus infection in Colombia: Diagnostic and treatment challenges. J Clin Virol. 2015;69:27-9. https://doi.org/10.1016/j.jcv.2015.05.021
Muñoz CM, Castillo JO, Salas D, Valderrama MA, Rangel CT, Vargas HP, et al. Atypical mucocutaneous manifestations in neonates and infants with chikungunya fever in the municipalities of Cúcuta, Los Patios and Villa del Rosario, Norte de Santander, Colombia, 2014. Biomédica. 2016;36:368-77. https://doi.org/10.7705/biomedica.v36i3.2760
Villamil-Gómez WE, Ramírez-Vallejo E, Cardona-Ospina JA, Silvera LA, Rodríguez-Morales AJ. Electrocardiographic alterations in patients with chikungunya fever from Sucre, Colombia: A 42-case series. Travel Med Infect Dis. 2016;14:510-2. https://doi.org/10.1016/J.TMAID.2016.06.004
Bonifay T, Prince C, Neyra C, Demar M, Rousset D, Kallel H, et al. Atypical and severe manifestations of chikungunya virus infection in French Guiana: A hospital-based study. PLoS ONE. 2018;13:e0207406. https://doi.org/10.1371/journal.pone.0207406
Pan American Health Organization/Health Information Platform for the Americas. PAHO/WHO Data - Weekly Report. Fecha de consulta: 12 de agosto de 2020. Disponible en: https://www.paho.org/data/index.php/en/mnu-topics/chikv-en/550-chikv-weekly-en.html
De Brito CAA. Alert: Severe cases and deaths associated with Chikungunya in Brazil. Rev Soc Bras Med Trop. 2017;50:585-9. https://doi.org/10.1590/0037-8682-0479-2016
Freitas ARR, Cavalcanti L, von Zuben AP, Donalisio MR. Excess mortality related to Chikungunya epidemics in the context of co-circulation of other Arboviruses in Brazil. PLoS Curr.2017;9:ecurrents.outbreaks.14608e586cd321d8d5088652d7a0d884. https://doi.org/10.1371/currents.outbreaks.14608e586cd321d8d5088652d7a0d884
Freitas AR, Alarcón-Elbal PM, Donalisio MR. Excess mortality in Guadeloupe and Martinique, islands of the French West Indies, during the chikungunya epidemic of 2014. Epidemiol Infect. 2018;146:2059-65. https://doi.org/10.1017/S0950268818002315
Freitas ARR, Donalisio MR, Alarcón-Elbal PM. Excess mortality and causes associated with Chikungunya, Puerto Rico, 2014-2015. Emerg Infect Dis. 2018;24:2352-5. https://doi.org/10.3201/eid2412.170639
Freitas ARR, Alarcón-Elbal PM, Paulino-Ramírez R, Donalisio MR. Excess mortality profile during the Asian genotype chikungunya epidemic in the Dominican Republic, 2014. Trans R Soc Trop Med Hyg. 2018;112:443-9. https://doi.org/10.1093/trstmh/try072
Gérardin P, Fianu A, Malvy D, Boussaïd K, Rollot O, Michault A, et al. Perceived morbidity and community burden after a Chikungunya outbreak: The TELECHIK survey, a populationbased cohort study. BMC Med. 2011;9:5. https://doi.org/10.1186/1741-7015-9-5
Soumahoro M-K, Gérardin P, Boëlle P-Y, Perrau J, Fianu A, Pouchot J, et al. Impact of Chikungunya virus infection on health status and quality of life: A retrospective cohort study. PLoS ONE. 2009;4:e7800. https://doi.org/10.1371/journal.pone.0007800
Rahim AA, Thekkekara RJ, Bina T, Paul BJ. Disability with persistent pain following an pidemic of chikungunya in rural south India. J Rheumatol. 2016;43:440-4. https://doi.org/10.3899/jrheum.141609
Mehta R, Gerardin P, de Brito CAA, Soares CN, Ferreira MLB, Solomon T. The neurological complications of chikungunya virus: A systematic review. Rev Med Virol. 2018;28:e1978. https://doi.org/10.1002/rmv.1978
Duvignaud A, Fianu A, Bertolotti A, Jaubert J, Michault A, Poubeau P, et al. Rheumatism and chronic fatigue, the two facets of post-chikungunya disease: The TELECHIK cohort study on Reunion island. Epidemiol Infect. 2018;146:633-41. https://doi.org/10.1017/S0950268818000031
Passi GR, Khan YZ, Chitnis DS. Chikungunya infection in neonates. Indian Pediatr. 2008;45:240-2.
Gérardin P, Barau G, Michault A, Bintner M, Randrianaivo H, Choker G, et al. Multidisciplinary prospective study of mother-to-child chikungunya virus infections on the island of La Réunion. PLoS Med. 2008;5:413-23. https://doi.org/10.1371/journal.pmed.0050060
Gérardin P, Sampériz S, Ramful D, Boumahni B, Bintner M, Alessandri J-L, et al. Neurocognitive outcome of children exposed to perinatal mother-to-child Chikungunya virus infection: The CHIMERE Cohort Study on Reunion Island. PLoS Negl Trop Dis. 2014;8:e2996. https://doi.org/10.1371/journal.pntd.0002996
Torres JR, Falleiros-Arlant LH, Dueñas L, Pleitez-Navarrete J, Salgado DM, del Castillo JB. Congenital and perinatal complications of chikungunya fever: a Latin American experience. Int J Infect Dis. 2016;51:85-8. https://doi.org/10.1016/j.ijid.2016.09.009
Villamil-Gómez W, Alba-Silvera L, Menco-Ramos A, González-Vergara A, Molinares-Palacios T, Barrios-Corrales M, et al. Congenital Chikungunya virus infection in Sincelejo, Colombia: A case series. J Trop Pediatr. 2015;61:386-92. https://doi.org/10.1093/tropej/fmv051
Instituto Nacional de Salud. Boletín Epidemiológico Semana 53. 2014. Fecha de consulta: 15 de julio de 2020. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2014 Boletin epidemiologico semana 53.pdf
Instituto Nacional de Salud. Boletín Epidemiológico Semana 52. 2015. Fecha de consulta: 15 de julio de 2020. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2015 Boletin epidemiologico Semana 52.pdf
Instituto Nacional de Salud. Boletín Epidemiológico Semana 52. 2016. Fecha de consulta: 15 de julio de 2020. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2016 Boletín epidemiológico semana 52 -.pdf
Instituto Nacional de Salud. Boletín Epidemiológico Semana 52. 2017. Fecha de consulta: 15 de julio de 2020. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2017 Boletín epidemiológico semana 52.pdf
Instituto Nacional de Salud. Boletín Epidemiológico Semana 52. 2018. Fecha de consulta: 15 de julio de 2020. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2018 Boletín epidemiológico semana 52.pdf
Instituto Nacional de Salud. Boletín Epidemiológico Semana 52. 2019. Fecha de consulta: 15 de julio de 2020. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2019_Boletin_epidemiologico_semana_52.pdf
Instituto Nacional de Salud. Boletín Epidemiológico Semana 33. 2020. Fecha de consulta: 26 de agosto de 2020. Disponible en: https://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2020_Boletin_epidemiologico_semana_33.pdf
Oviedo-Pastrana M, Méndez N, Mattar S, Arrieta G, Gomezcaceres L. Lessons learned of emerging Chikungunya virus in two populations of social vulnerability of the Colombian tropics: Epidemiological analysis. Arch Public Heal. 2018;76:36. https://doi.org/10.1186/s13690-018-0284-2
Calvo EP, Sánchez-Quete F, Durán S, Sandoval I, Castellanos JE. Easy and inexpensive molecular detection of dengue, chikungunya and zika viruses in febrile patients. Acta Trop. 2016;163:32-7. https://doi.org/10.1016/j.actatropica.2016.07.021
Mercado M, Acosta-Reyes J, Parra E, Pardo L, Rico A, Campo E, et al. Clinical and histopathological features of fatal cases with dengue and chikungunya virus co-infection in Colombia, 2014 to 2015. Eurosurveillance. 2016;21:30244. https://doi.org/10.2807/1560-7917.ES.2016.21.22.30244
Carrillo-Hernández MY, Ruiz-Saenz J, Villamizar LJ, Gómez-Rangel SY, Martínez-Gutiérrez M. Co-circulation and simultaneous co-infection of dengue, chikungunya, and zika viruses in patients with febrile syndrome at the Colombian-Venezuelan border. BMC Infect Dis. 2018;18:61. https://doi.org/10.1186/s12879-018-2976-1
Mercado-Reyes M, Acosta-Reyes J, Navarro-Lechuga E, Corchuelo S, Rico A, Parra E, et al. Dengue, chikungunya and zika virus coinfection: Results of the national surveillance during the zika epidemic in Colombia. Epidemiol Infect. 2019;147:e-77. https://doi.org/10.1017/S095026881800359X
Mattar S, Miranda J, Pinzón H, Tique V, Bolanos A, Aponte J, et al. Outbreak of chikungunya virus in the north Caribbean area of Colombia: clinical presentation and phylogenetic analysis. J Infect Dev Ctries. 2015;9:1126-32. https://doi.org/10.3855/jidc.6670
Pinzón-Redondo H, Paternina-Caicedo A, Barrios-Redondo K, Zarate-Vergara A, Tirado-Pérez I, Fortich R, et al. Risk factors for severity of chikungunya in children: A prospective assessment. Pediatr Infect Dis J. 2016;35:702-4. https://doi.org/10.1097/INF.0000000000001135
Villamil-Gómez W, Silvera LA, Páez-Castellanos J, Rodriguez-Morales AJ. Guillain–Barré syndrome after Chikungunya infection: A case in Colombia. Enferm Infecc Microbiol Clin. 2016;34:140-1. https://doi.org/10.1016/J.EIMC.2015.05.012
Rodríguez-Morales AJ, Calvache-Benavides CE, Giraldo-Gómez J, Hurtado-Hurtado N, Yepes-Echeverri MC, García-Loaíza J, et al. Post-chikungunya chronic arthralgia: Results from a retrospective follow-up study of 131 cases in Tolima, Colombia. Travel Med Infect Dis. 2016;14:58-9. https://doi.org/10.1016/J.TMAID.2015.09.001
Rodríguez-Morales AJ, Villamil-Gómez W, Merlano-Espinosa M, Simone-Kleber L. Postchikungunya chronic arthralgia: A first retrospective follow-up study of 39 cases in Colombia. Clin Rheumatol. 2016;35:831-2. https://doi.org/10.1007/s10067-015-3041-8
Consuegra-Rodríguez MP, Hidalgo-Zambrano DM, Vásquez-Serna H, Jiménez-Cañizales CE, Parra-Valencia E, Rodríguez-Morales AJ. Post-chikungunya chronic inflammatory rheumatism: Follow-up of cases after 1 year of infection in Tolima, Colombia. Travel Med Infect Dis. 2018;21:62-8. https://doi.org/10.1016/J.TMAID.2017.11.013
Chang AY, Encinales L, Porras A, Pacheco N, Reid SP, Martins K, et al. Frequency of chronic joint pain following chikungunya virus infection: A Colombian cohort study. Arthritis Rheumatol (Hoboken, NJ). 2018;70:578-84. https://doi.org/10.1002/art.40384
Alvis-Zakzuk N, Díaz-Jiménez D, Castillo-Rodríguez L, Castañeda-Orjuela C, Paternina-Caicedo Á, Pinzón-Redondo H, et al. Economic costs of Chikungunya virus in Colombia. alue Heal Reg Issues. 2018;17:32-7. https://doi.org/10.1016/j.vhri.2018.01.004
Cardona-Ospina JA, Díaz-Quijano FA, Rodríguez-Morales AJ. Burden of chikungunya in Latin American countries: Estimates of disability-adjusted life-years (DALY) lost in the 2014 epidemic. Int J Infect Dis. 2015;38:60-1. https://doi.org/10.1016/j.ijid.2015.07.015
Rodríguez-Moralesa AJ, Anaya JM. Impact of emerging arthritogenic arboviruses in Colombia and Latin America. Rev Colomb Reumatol. 2016;23:145-7. https://doi.org/10.1016/j.rcreu.2016.08.001
Villero-Wolf Y, Mattar S, Puerta-González A, Arrieta G, Muskus C, Hoyos R, et al. Genomic epidemiology of Chikungunya virus in Colombia reveals genetic variability of strains and multiple geographic introductions in outbreak, 2014. Sci Rep. 2019;9:9970. https://doi.org/10.1038/s41598-019-45981-8
Algunos artículos similares:
- Patricio Mora , Paúl Quinatoa , Diego Morales, Actualización de la distribución espaciotemporal de Aedes albopictus en Ecuador , Biomédica: Vol. 45 Núm. 3 (2025)
- Daniel Eduardo Henao, Fabián Alberto Jaimes, Medicina basada en la evidencia: una aproximación epistemológica , Biomédica: Vol. 29 Núm. 1 (2009)
- Luz Elena Velásquez, Catalina Gómez, Erika Valencia, Laura Salazar, Eudoro Casas, Estudio de foco de paragonimosis en Fuente Clara, Robledo, área periurbana de Medellín, Antioquia , Biomédica: Vol. 28 Núm. 3 (2008)
- Juan P. Gómez, Juan C. Quintana, Patricia Arbeláez, Jorge Fernández, Juan F. Silva, Jacqueline Barona, Juan C. Gutiérrez, Abel Díaz, Rafael Otero, Picaduras por escorpión Tityus asthenes en Mutatá, Colombia: aspectos epidemiológicos, clínicos y toxinológicos , Biomédica: Vol. 30 Núm. 1 (2010)
- Juan Gabriel Piñeros, Malaria y determinantes sociales de la salud: un nuevo marco heurístico desde la medicina social latinoamericana , Biomédica: Vol. 30 Núm. 2 (2010)
- Richard Hoyos, Lisandro Pacheco, Luz Adriana Agudelo, German Zafra, Pedro Blanco, Omar Triana, Seroprevalencia de la enfermedad de Chagas y factores de riesgo asociados en una población de Morroa, Sucre , Biomédica: Vol. 27 Núm. 1esp (2007): Enfermedad de Chagas
- Gloria Inés Múnera, Jairo Andrés Méndez, Gloria Janneth Rey, Importancia de los análisis serológicos, moleculares y virológicos en la vigilancia de la fiebre amarilla en Colombia, 2006-2008 , Biomédica: Vol. 30 Núm. 3 (2010)
- Angélica María Delgado-Vega, Javier Martín, Julio Granados, Juan Manuel Anaya, Epidemiología genética de la artritis reumatoide: ¿qué esperar de América Latina? , Biomédica: Vol. 26 Núm. 4 (2006)
- Diana Marcela Echeverry, Juan Miguel Rengifo, Jhon Carlos Castaño, Germán Alberto Téllez, María Mercedes González, Prevalencia de Mammomonogamus laryngeus (Strongylida: Syngamidae) en ganado bovino de la central de beneficio del municipio de La Tebaida, Quindío, Colombia , Biomédica: Vol. 31 Núm. 3 (2011)
- Gladys Acuña-González, Carlo E. Medina-Solís, Gerardo Maupomé, Mauricio Escoffie-Ramírez, Jesús Hernández-Romano, María de L. Márquez-Corona, Arturo J. Islas-Márquez, Juan J. Villalobos-Rodelo, Factores de riesgo hereditarios y socioeconómicos para labio o paladar hendido no asociados a un síndrome en México: estudio de casos y controles pareado , Biomédica: Vol. 31 Núm. 3 (2011)
| Estadísticas de artículo | |
|---|---|
| Vistas de resúmenes | |
| Vistas de PDF | |
| Descargas de PDF | |
| Vistas de HTML | |
| Otras vistas | |

























