Liver abscess due to Granulicatella adiacens in an immunocompetent patient: Case report
Abstract
Pyogenic liver abscesses due to Granulicatella adiacens are infections associated with high mortality, mainly in immunocompromised patients. The main microorganisms associated with liver abscesses are Klebsiella pneumoniae, and Escherichia coli, though it may also be polymicrobial. However, case reports describing liver infection by Granulicatella adiacens are scarce.
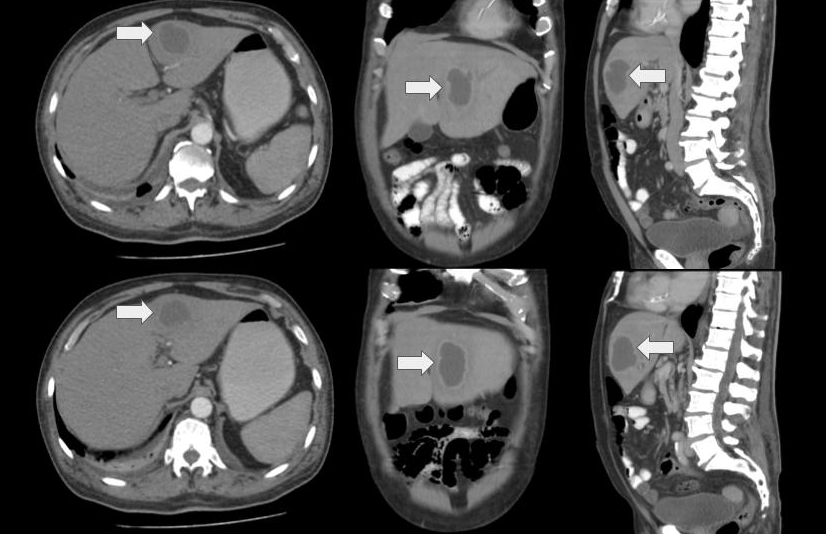
We present the case of an immunocompetent adult patient who presented 15 days of evolution consisting of quantified fever peaks associated with asthenia, adynamia, chills, jaundice and coluria. The initial clinical examination revealed a generalized icteric tint without abdominal pain, and blood pressure with a tendency to hypotension. Biliopancreatic confluent neoplasia, secondary cholangitis and sepsis of biliary origin were suspected, initiating fluid resuscitation and antibiotic therapy; blood cultures and complementary diagnostic studies were taken. Hepatobiliary ultrasound with evidence of an abscess of 73 x 62 mm in segment IV; the bile duct and pancreas were within normal limits. To better characterize the lesion evidenced in the liver, a contrast-enhanced computed tomography of the abdomen was performed. The patient completed antibiotic management with ciprofloxacin, vancomycin, and metronidazole in good condition and was successfully discharged.
This is the first pyogenic liver abscess reported caused by Granulicatella adiacens in an immunocompetent patient, in whom early microbiological diagnosis in conjunction with targeted antibiotic treatment and percutaneous drainage of the lesion was decisive in the clinical outcome.
Downloads
References
Serraino C, Elia C, Bracco C, Rinaldi G, Pomero F, Silvestri A, et al. Characteristics and management of pyogenic liver abscess: A European experience. Medicine (Baltimore). 2018;97(19):e0628. https://doi.org/10.1097/MD.0000000000010628
Perna A, Ricciardi L, Sturiale CL, Fantoni M, Tamburrelli FC, Bonfiglio N, et al. Skipped vertebral spontaneous spondylodiscitis caused by Granulicatella adiacens: Case report and a systematic literature review. J Clin Orthop Trauma. 2020;11:937-41. https://doi.org/10.1016/j.jcot.2019.07.002
Gupta S, Garg M, Misra S, Singhal S. Granulicatella adiacens abscess: Two rare cases and review. J Lab Physicians. 2018;10:121-3. https://doi.org/10.4103/JLP.JLP_58_17
Roediger R, Lisker-Melman M. Pyogenic and amebic infections of the liver. Gastroenterol Clin North Am. 2020;49:361-77. https://doi.org/10.1016/j.gtc.2020.01.013
Elfessi Z, Liu E, Dukarevich Y, Caniff K, Marquez K, Shabbir Z. Sepsis induced bacterial peritonitis caused by Granulicatella adiacens. Am J Emerg Med. 2019;37:2263.e1-2263.e3. https://doi.org/10.1016/j.ajem.2019.158428
Cargill JS, Scott KS, Gascoyne-Binzi D, Sandoe JAT. Granulicatella infection: Diagnosis and management. J Med Microbiol. 2012:61;755-61. https://doi.org/10.1099/jmm.0.039693-0
Alberti MO, Hindler JA, Humphries RM. Antimicrobial susceptibilities of Abiotrophia defectiva, Granulicatella adiacens, and Granulicatella elegans. Antimicrob Agents Chemother. 2015;60:1411-20. https://doi.org/10.1128/AAC.02645-15
Khim G, Em S, Mo S, Townell N. Liver abscess: Diagnostic and management issues found in the low resource setting. Br Med Bull. 2019;132:45-52. https://doi.org/10.1093/bmb/ldz032
Teo L, Looi A, Seah LL. An unusual causative agent for an orbital abscess: Granulicatella adiacens. Orbit. 2011;30:162-4. https://doi.org/10.3109/01676830.2011.569631
Yang S, Wu L, Xu L, Huang X, Sun X, Yang L, et al. Lung abscess secondary to lung cancer with a coinfection of Granulicatella adiacens and other bacteria: A case report. BMC Infect Dis. 2021;21:662. https://doi.org/10.1186/s12879-021-06191-8
Quénard F, Seng P, Lagier JC, Fenollar F, Stein A. Prosthetic joint infection caused by Granulicatella adiacens: A case series and review of literature. BMC Musculoskelet Disord. 2017;18:276. https://doi.org/10.1186/s12891-017-1630-1
Lardière-Deguelte S, Ragot E, Amroun K, Piardi T, Dokmak S, Bruno O, et al. Hepatic abscess: Diagnosis and management. J Visc Surg. 2015;152:231-43. https://doi.org/10.1016/j.jviscsurg.2015.01.013
Liu Y, Li Z, Liu A, Xu J, Li Y, Liu J, et al. Early percutaneous catheter drainage in protecting against prolonged fever among patients with pyogenic liver abscess: A retrospective cohort study. Ann Med. 2022;54:2269-77. https://doi.org/10.1080/07853890.2022.2110612
Haider SJ, Tarulli M, McNulty NJ, Hoffer EK. Lliver abscesses: Factors that influence outcome of percutaneous drainage. AJR Am J Roentgenol. 2017;209:205-213. https://doi.org/10.2214/AJR.16.17713
Some similar items:
- Guido Ricardo González, Ana María Navarro, Ángela Regina Zambrano, Ana María Arrunátegui, Nodular hepatic lesions secondary to myeloma IgA presenting as fever of unknown origin , Biomedica: Vol. 30 No. 4 (2010)
- Gustavo Aroca, María Vélez-Verbel , Andrés Cadena , Lil Geraldine Avendaño , Sandra Hernández, Angélica Sierra, Omar Cabarcas, Santos Ángel Depine, COVID-19 in hemodialysis patients in Colombia: Report of seven cases , Biomedica: Vol. 40 No. Supl. 2 (2020): SARS-CoV-2 y COVID-19
Copyright (c) 2023 Biomedica

This work is licensed under a Creative Commons Attribution 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























