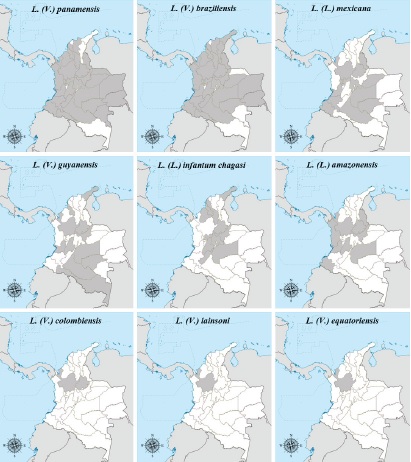
Geographical distribution of Leishmania species in Colombia, 1985-2017
Abstract
Introduction: Knowledge of the geographical distribution of Leishmania species allows guiding the sampling to little-studied areas and implementing strategies to define risk zones and priority areas for control.
Objective: Given that there is no publication that collects this information, the search, review, and compilation of the available scientific literature that has identified species in Colombia is presented in this paper.
Materials and methods: A bibliographic search was performed in PubMed, Web of Knowledge, Google Scholar, SciELO and LILACS with the terms “(Leishmania OR Leishmaniasis) AND species AND Colombia”, without restrictions on publication year, language or infected organism; records of national scientific events and repositories of theses from Colombian universities were also included.
Results: Eighty-six scientific documents published between 1985 and 2017 were found in which the species of Leishmania and their geographical origin were indicated. The species reported, in descending order of frequency, were: Leishmania (Viannia) panamensis, L. (V.) braziliensis, L. (V.) guyanensis, L. (Leishmania) infantum, L. (L.) amazonensis, L. (L.) mexicana, L. (V.) colombiensis, L. (V.) lainsoni and L. (V.) equatorensis; the last three were found with the same frequency. Leishmania species were reported from 29 departments.
Conclusion: Information on the distribution of Leishmania species in Colombia is limited; therefore, it is necessary to gather existing data and propose studies that consolidate the distribution maps of Leishmania species in Colombia. This would allow the detection of areas where species have not been identified as well as the comparison of existing parasite and vector distributions.
Downloads
References
Alvar J, Vélez ID, Bern C, Herrero M, Desjeux P, Cano J, et al. Leishmaniasis worldwide and global estimates of its incidence. PloS ONE. 2012;7:e35671. https://doi.org/10.1371/journal.pone.0035671
Intituto Nacional de Salud. Boletín Epidemiológico Semanal. Diciembre 2016. Reporte No. 52. Fecha de consulta: 15 de marzo de 2017. Disponible en: http://www.ins.gov.co/buscador-eventos/BoletinEpidemiologico/2016%20Bolet%C3%ADn%20epidemiol%C3%B3gico%20semana%2052%20-.pdf
World Health Organization. Leishmaniasis in high-burden countries: An epidemiological update based on data reported in 2014. Wkly Epidemiol Rec. 2016;91:287-96.
Corredor A, Kreutzer RD, Tesh RB, Boshell J, Palau MT, Cáceres E, et al. Distribution and etiology of leishmaniasis in Colombia. Am J Trop Med Hyg. 1990;42:206-14.
https://doi.org/10.4269/ajtmh.1990.42.206
Ovalle CE, Porras L, Rey M, Ríos M, Camargo YC. Distribución geográfica de especies de Leishmania aisladas de pacientes consultantes al Instituto Nacional de Dermatología Federico Lleras Acosta, ESE, 1995-2005. Biomédica. 2006;26:145-51. https://doi.org/10.7705/biomedica.v26i1.1508
Ramírez JD, Hernández C, León CM, Ayala MS, Flórez C, González C. Taxonomy, diversity, temporal and geographical distribution of cutaneous leishmaniasis in Colombia: A retrospective study. Sci Rep. 2016;6:28266. https://doi.org/10.1038/srep28266
Saravia NG, Weigle K, Navas C, Segura I, Valderrama L, Valencia AZ, et al. Heterogeneity, geographic distribution, and pathogenicity of serodemes of Leishmania viannia in Colombia. mAm J Trop Med Hyg. 2002;66:738-44. https://doi.org/10.4269/ajtmh.2002.66.738
Patiño LH, Méndez C, Rodríguez O, Romero Y, Velandia D, Alvarado M, et al. Spatial distribution, Leishmania species and clinical traits of cutaneous leishmaniasis cases in the Colombian army. PLoS Negl Trop Dis. 2017;11:e0005876. https://doi.org/10.1371/journal.pntd.0005876
Arroyo C, Garzón J. Investigación de un foco de leishmaniasis cutánea en la zona andina del departamento de Nariño. Biomédica. 1995;16:25-31. https://doi.org/10.7705/biomedica.v16i1.887
Ferro C, Marín D, Góngora R, Carrasquilla MC, Trujillo JE, Rueda NK, et al. Phlebotomine vector ecology in the domestic transmission of American cutaneous leishmaniasis in Chaparral, Colombia. Am J Trop Med Hyg. 2011;85:847-56. https://doi.org/10.4269/ajtmh.2011.10-0560
Moreno M, Ferro C, Rosales-Chilama M, Rubiano L, Delgado M, Cossio A, et al. First report of Warileya rotundipennis (Psychodidae: Phlebotominae) naturally infected with Leishmania (Viannia) in a focus of cutaneous leishmaniasis in Colombia. Acta Tropica. 2015;148:191-6. https://doi.org/10.1016/j.actatropica.2015.04.017
Sierra D, Ochoa M, Calle JI, García G, Colorado D, Vélez ID. Leishmania (Leishmania) mexicana en el corregimiento de San Matías, municipio de Gómez Plata, Antioquia, Colombia. Biomédica. 2006;26:232-5. https://doi.org/10.7705/biomedica.v26i1.1517
Vélez ID, Carrillo LM, López L, Rodríguez E, Robledo SM.An epidemic outbreak of canine cutaneous leishmaniasis in Colombia caused by Leishmania braziliensis and Leishmania panamensis. Am J Trop Med Hyg. 2012;86:807-11. https://doi.org/10.4269/ajtmh.2012.11-0408
Kreutzer RD, Corredor A, Grimaldi G, Grogl M, Rowton ED, Young DG, et al. Characterization of Leishmania colombiensis Sp. N (Kinetoplastida: Trypanosomatidae), a new parasite infecting humans, animals, and phlebotomine sand flies in Colombia and Panama. Am J Trop Med Hyg. 1991;44:662-75. https://doi.org/10.4269/ajtmh.1991.44.662
Fernández OL, Díaz-Toro Y, Ovalle C, Valderrama L, Muvdi S, Rodríguez I, et al. Miltefosine and antimonial drug susceptibility of Leishmania Viannia species and populations in regions of high transmission in Colombia. PLoS Negl Trop Dis. 2014;8:e2871. https://doi.org/10.1371/journal.pntd.0002871
Saravia NG, Segura I, Holguín AF, Santrich C, Valderrama L, Ocampo C. Epidemiologic, genetic, and clinical associations among phenotypically distinct populations of Leishmania (Viannia) in Colombia. Am J Trop Med Hyg. 1998;59:86-94. https://doi.org/10.4269/ajtmh.1998.59.86
Rodríguez G, Corredor A, Cáceres E, Cassiano G, Arroyo C, Palau M, et al. Leishmaniasis difusa. Biomédica. 1985;5:95-111. https://doi.org/10.7705/biomedica.v5i3-4.1909
Hernández C, Álvarez C, González C, Ayala MS, León CM, Ramírez JD. Identification of six New World Leishmania species through the implementation of a High-Resolution Melting (HRM) genotyping assay. Parasit Vectors. 2014;7:501. https://doi.org/10.1186/s13071-014-0501-y
Posada L, Vélez A, Acosta L, Cadena H, Agudelo D, Vélez I. Descripción de un foco endémico de leishmaniasis cutánea en Puerto Valdivia, Antioquia, Colombia. CES Salud Pública. 2014;5:3-10.
Martínez LP, Rebollo JA, Luna AL, Cochero S, Bejarano EE. Molecular identification of the parasites causing cutaneous leishmaniasis on the Caribbean coast of Colombia. Parasitol Res. 2010;106:647-52. https://doi.org/10.1007/s00436-009-1712-6
Alexander B, Lozano C, Barker DC, McCannb SHE, Adler GH. Detection of Leishmania (Viannia) braziliensis complex in wild mammals from Colombian coffee plantations by PCR and DNA hybridization. Acta Trop. 1998;69:41-50. https://doi.org/10.1016/S0001-706X(97)00114-9
Vásquez-Trujillo A, González-Reina AE, Góngora-Orjuela A, Prieto-Suárez E, Palomares JE, Buitrago-Álvarez LS. Seasonal variation and natural infection of Lutzomyia antunesi (Diptera: Psychodidae: Phlebotominae), an endemic species in the Orinoquia region of Colombia. Mem Inst Oswaldo Cruz. 2013;108:463-9.
https://doi.org/10.1590/S0074-0276108042013011
Santaella J, Ocampo CB, Saravia NG, Méndez F, Góngora R, Gómez MA, et al. Leishmania (Viannia) infection in the domestic dog in Chaparral, Colombia. Am J Trop Med Hyg. 2011;84:674-80. https://doi.org/10.4269/ajtmh.2011.10-0159
Cochero S, Anaya Y, Díaz Y, Paternina M, Luna A, Paternina L, et al. Infección natural de Lutzomyia cayennensis cayennensis con parásitos tripanosomatídeos (Kinetoplastida: Trypanosomatidae) en Los Montes de María, Colombia. Rev Cubana Med Trop. 2007;59:35-9.
Santrich C, Segura I, Arias AL, Saravia NG. Mucosal disease caused by Leishmania braziliensis guyanensis. Am J Trop Med Hyg. 1990;42:51-5. https://doi.org/10.4269/ajtmh.1990.42.51
Saravia NG, Holguín AF, McMahon-Pratt D, D’Alessandro A. Mucocutaneous leishmaniasis in Colombia - Leishmania-braziliensis subspecies diversity. Am J Trop Med Hyg. 1985;34:714-20. https://doi.org/10.4269/ajtmh.1985.34.714
Weigle KA, Saravia NG, de Dávalos M, Moreno LH, D’Alessandro A. Leishmania braziliensis from the Pacific coast region of Colombia: Foci of transmission, clinical spectrum and isoenzyme phenotypes. Am J Trop Med Hyg. 1986;35:722-31. https://doi.org/10.4269/ajtmh.1986.35.722
Mestra L, López L, Robledo SM, Muskus CE, Nicholls RS, Vélez ID. Transfusiontransmitted visceral leishmaniasis caused by Leishmania (Leishmania) mexicana in an immunocompromised patient: A case report. Transfusion. 2011;51:1919-23. https://doi.org/10.1111/j.1537-2995.2011.03092.x
Travi BL, Montoya J, Solarte Y, Lozano L, Jaramillo C. Leishmaniasis in Colombia. I. Studies on the phlebotomine fauna associated with endemic foci in the Pacific Coast region. Am J Trop Med Hyg. 1988;39:261-6. https://doi.org/10.4269/ajtmh.1988.39.261
Young DG, Morales A, Kreutzer RD, Alexander JB, Corredor A, Tesh RB. Isolation of Leishmania-braziliensis (Kinetoplastida, Trypanosomatidae) from cryopreserved Colombian sand flies (Diptera, Psychodidae). J Med Entomol. 1987;24:587-9. https://doi.org/10.1093/jmedent/24.5.587
Travi BL, Montoya J, Gallego J, Jaramillo C, Llano R, Vélez ID. Bionomics of Lutzomyia evansi (Diptera: Psychodidae) vector of visceral leishmaniasis in northern Colombia. J Med Entomol. 1996;33:278-85. https://doi.org/10.1093/jmedent/33.3.278
Travi BL, Vélez ID, Brutus L, Segura I, Jaramillo C, Montoya J. Lutzomyia evansi, an alternate vector of Leishmania chagasi in a Colombian focus of visceral leishmaniasis. Trans R Soc Trop Med Hyg. 1990;84:676-7. https://doi.org/10.1016/0035-9203(90)90142-2
Vélez ID, Travi B, Gallego J, Palma G, Agudelo S, Montoya J, et al. Evaluación ecoepidemiológica de la leishmaniosis visceral en la comunidad indígena Zenú de San Andrés de Sotavento, Córdoba: primer paso para su control. Revista Colombiana de Entomología. 1995;21:111-22.
Corredor A, Gallego JF, Tesh RB, Morales A, de Carrasquilla CF, Young DG, et al. Epidemiology of visceral leishmaniasis in Colombia. Am J Trop Med Hyg. 1989;40:480-6. https://doi.org/10.4269/ajtmh.1989.40.480
Ferro C, Morrison AC, Torres M, Pardo R, Wilson ML, Tesh RB. Age structure, blood-feeding behavior, and Leishmania chagasi infection in Lutzomyia longipalpis (Diptera: Psychodidae) at an endemic focus of visceral leishmaniasis in Colombia. J Med Entomol. 1995;32:618-29. https://doi.org/10.1093/jmedent/32.5.618
Santamaría E, Ponce N, Zipa Y, Ferro C. Presencia en el peridomicilio de vectores infectados con Leishmania (Viannia) panamensis en dos focos endémicos en el occidente de Boyacá, piedemonte del valle del Magdalena medio, Colombia. Biomédica. 2006;26:82-94. https://doi.org/10.7705/biomedica.v26i1.1503
Flórez M, Martínez JP, Gutiérrez R, Luna KP, Serrano VH, Ferro C, et al. Lutzomyia longipalpis (Diptera: Psychodidae) en un foco suburbano de leishmaniosis visceral en el Cañón del Chicamocha en Santander, Colombia. Biomédica. 2006;26:109-20. https://doi.org/10.7705/biomedica.v26i1.1505
Travi BL, Osorio Y, Becerra MT, Adler GH. Dynamics of Leishmania chagasi infection in small mammals of the undisturbed and degraded tropical dry forests of northern Colombia. Trans R Soc Trop Med Hyg. 1998;92:275-8. https://doi.org/10.1016/S0035-9203(98)91009-4
Ocampo CB, Ferro MC, Cadena H, Góngora R, Pérez M, Valderrama-Ardila CH, et al. Environmental factors associated with American cutaneous leishmaniasis in a new Andean focus in Colombia. Trop Med Int Health. 2012;17:1309-17. https://doi.org/10.1111/j.1365-3156.2012.03065.x
Travi BL, Tabares CJ, Cadena H. Leishmania (Viannia) braziliensis infection in two Colombian dogs: A note on infectivity for sand flies and response to treatment. Biomédica. 2006;26:249-53. https://doi.org/10.7705/biomedica.v26i1.1520
Vásquez-Trujillo A, Gonzáles A, Góngora-Orjuela A, Cabrera O, Santamaría E, Buitrago Álvarez L. Identificación de Leishmania (Viannia) guyanensis en caninos, en zona rural del municipio de Villavicencio, Meta, Colombia. Orinoquia. 2008;12:173-81.
Loyola EG, Alzate A, Sánchez A, González A. Epidemiology of a natural focus of Leishmaniabraziliensis in the pacific lowlands of Colombia. III. Natural infections in wild mammals. Trans R Soc Trop Med Hyg. 1988;82:406-7. https://doi.org/10.1016/0035-9203(88)90136-8
Castro LS, Franca Ade O, Ferreira Ede C, Hans Filho G, Higa Junior MG, Gontijo CM, et al. Leishmania infantum as a causative agent of cutaneous leishmaniasis in the state of Mato Grosso do Sul, Brazil. Rev Inst Med Trop Sao Paulo. 2016;58:23. https://doi.org/10.1590/S1678-9946201658023
Noyes H, Chance M, Ponce C, Ponce E, Maingon R. Leishmania chagasi: Genotypically similar parasites from Honduras cause both visceral and cutaneous leishmaniasis in humans. Exp Parasitol. 1997;85:264-73. https://doi.org/10.1006/expr.1996.4133
World Health Organization. Control of the Leishmaniases. Report of a meeting of the WHO Expert Committee on the control of Leishmaniases. Tech Rep Ser 949. Geneva: WHO; 2010. p. 1-186.
Ferro C, López M, Fuya P, Lugo L, Cordovez JM, González C. Spatial distribution of sand fly vectors and eco-epidemiology of cutaneous leishmaniasis transmission in Colombia. PloS One. 2015;10:e0139391. https://doi.org/10.1371/journal.pone.0139391
Some similar items:
- Gregory H. Adler, María Teresa Becerra, Bruno L. Travi, Feeding success of Lutzomyia evansi (Diptera: Psychodidae) experimentally exposed to small mammal hosts in an endemic focus of Leishmania chagasi in northern Colombia. , Biomedica: Vol. 23 No. 4 (2003)
- Eduar Elías Bejarano, Rafael José Vivero, Sandra Uribe, First record of the sand fly Warileya (Hertigia) hertigi from Antioquia, Colombia , Biomedica: Vol. 38 No. 2 (2018)
- Clemencia Ovalle-Bracho, Carolina Camargo, Yira Díaz-Toro, Marcela Parra-Muñoz, Molecular typing of Leishmania (Leishmania) amazonensis and species of the subgenus Viannia associated with cutaneous and mucosal leishmaniasis in Colombia: A concordance study , Biomedica: Vol. 38 No. 1 (2018)
- Margaret Paternina-Gómez, Yirys Díaz-Olmos, Luis Enrique Paternina, Eduar Elías Bejarano, High prevalence of infection with Leishmania (Kinetoplastea: Trypanosomatidae) in dogs in northern Colombia , Biomedica: Vol. 33 No. 3 (2013)
- Johana Marin, Daniel Urrea, Carlos Muskus, María Clara Echeverry, Ana María Mejía, Omar Triana, High-resolution melting analysis based on specific genomic regions: A promising tool for the diagnosis and typing of species causing cutaneous leishmaniasis in Colombia , Biomedica: Vol. 37 No. 4 (2017)
- Rafael J. Vivero, María Angélica Contreras, Juan D. Suaza, Iván D. Vélez, Charles Porter, Sandra Uribe, Species of sand flies (Diptera: Psychodidae) collected from natural reserves in the Pacific and Darien regions of Colombia , Biomedica: Vol. 37 No. Sup. 2 (2017): Suplemento 2, Entomología médica, 2017
- Elizabeth Borrero, Gabriel Carrasquilla, Neal Alexander, Decentralization and health system reform: What is their impact on malaria incidence in Colombian municipalities? , Biomedica: Vol. 32 (2012): Suplemento 1, Malaria
- María Angélica Contreras, Rafael José Vivero, Eduar Elías Bejarano, Lina María Carrillo, Iván Darío Vélez, New records of phlebotomine sand flies (Diptera: Psychodidae) near the Amoya River in Chaparral, Tolima , Biomedica: Vol. 32 No. 2 (2012)
- Raúl Murillo, Ricardo Cendales, Carolina Wiesner, Marion Piñeros, Sandra Tovar, Effectiveness of cytology-based cervical cancer screening in the Colombian health system , Biomedica: Vol. 29 No. 3 (2009)
- Andrés Páez, Gloria Rey, Carlos Agudelo, Alvaro Dulce, Edgar Parra, Hernando Díaz-Granados, Damaris Heredia, Luis Polo, Outbreak of urban rabies transmitted by dogs in Santa Marta, northern Colombia , Biomedica: Vol. 29 No. 3 (2009)
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |

























