Una perspectiva histórica sobre la autoinmunidad contra las citocinas: doble impacto a la enfermedad autoinmunitaria
Resumen
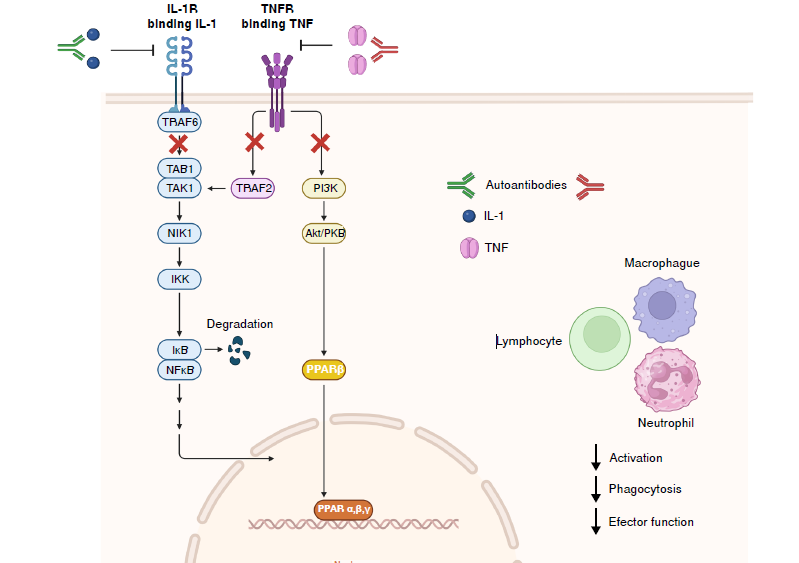
Las reacciones autoinmunitarias se caracterizan por el desarrollo de anticuerpos y la activación de linfocitos T contra autoantígenos. Esto desata una respuesta inmunitaria efectora contra los tejidos que expresan antígenos reconocidos por la autoinmunidad.
Los antígenos atacados por anticuerpos se denominan “autoantígenos” y son de diferentes tipos, como receptores, enzimas y proteínas de canal.
La reacción autoinmunitaria es potenciada por citocinas que median la activación de los linfocitos Th1, Th2 o Th17. Las citocinas liberadas también pueden ser reconocidas como autoantígenos y, por lo tanto, pueden ser objetivos de la reacción autoinmunitaria.
Los efectos de la autoinmunidad en las citocinas o sus receptores son diversos, razón por la cual los mecanismos de este tipo de reacción autoinmunitaria se discuten en esta revisión.
Descargas
Referencias bibliográficas
Zhang JM, An J. Cytokines, inflammation, and pain. Int Anesthesiol Clin. 2007;45:27-37. https://doi.org/10.1097/AIA.0b013e318034194e
Kany S, Vollrath JT, Relja B. Cytokines in inflammatory disease. Int J Mol Sci. 2019;20:6008. https://doi.org/10.3390/ijms20236008
O’Shea JJ, Ma A, Lipsky P. Cytokines and autoimmunity. Nat Rev Immunol. 2002;2:37-45. https://doi.org/10.1038/nri702
Browne SK. Anticytokine autoantibody-associated immunodeficiency. Annu Rev Immunol. 2014;32:635-57. https://doi.org/10.1146/annurev-immunol-032713-120222
Knight V. Immunodeficiency and autoantibodies to cytokines. J Appl Lab Med. 2022;7:151-64. https://doi.org/10.1093/jalm/jfab099
Thurner L, Kessel C, Fadle N, Regitz E, Seidel F, Kindermann I, et al. IL-1RA antibodies in myocarditis after SARS-CoV-2 vaccination. N Engl J Med. 2022;387:1524-7. https://doi.org/10.1056/NEJMc2210543
Kärner J, Pihlap M, Ranki A, Krohn K, Trebusak-Podkrajsek K, Bratanic N, et al. IL-6-specific autoantibodies among APECED and thymoma patients. Immun Inflamm Dis. 2016;4:235-43. https://doi.org/10.1002/iid3.107
Migliorini P, Italiani P, Pratesi F, Puxeddu I, Boraschi D. The IL-1 family cytokines and receptors in autoimmune diseases. Autoimmun Rev. 2020;19:102617. https://doi.org/10.1016/j.autrev.2020.102617
Shao M, Sun XL, Sun H, He J, Zhang RJ, Zhang X, et al. Clinical relevance of autoantibodies against interleukin-2 in patients with systemic lupus erythematosus. Chin Med J (Engl). 2018;131:1520-6. https://doi.org/10.4103/0366-6999.235867
Zhou W, Wang W. Autoantibodies against type I IFNs are associated with severe COVID-19 pneumonia. Signal Transduct Target Ther. 2021;6:96. https://doi.org/10.1038/s41392-021-00530-9
Kaufmann SH. Remembering Emil von Behring: From tetanus treatment to antibody cooperation with phagocytes. mBio. 2017;8:e00117-17. https://doi.org/10.1128/mBio.00117-17
Isaacs A, Lindenmann J. Classics in oncology: Virus interference: I. the interferon. CA Cancer J Clin. 1988;38:280-290. https://doi.org/10.3322/canjclin.38.5.280
Metcalf D. The colony stimulating factors. Discovery, development, and clinical applications. Cancer. 1990;65:2185-95.
https://doi.org/10.1002/1097-0142(19900515)65:10<2185::AID-CNCR2820651015>3.0.CO;2-U
Dumonde DC, Wolstencroft RA, Panayi GS, Matthew M, Morley J, Howson WT. "Lymphokines": non-antibody mediators of cellular immunity generated by lymphocyte activation. Nature. 1969 Oct 4;224(5214):38-42. https://doi.org/10.1038/224038a0
Cohen S, Bigazzi PE, Yoshida T. Commentary. Similarities of T cell function in cell-mediated immunity and antibody production. Cell Immunol. 1974 Apr;12(1):150-9. doi: 10.1016/0008-8749(74)90066-5. PMID: 4156495. https://doi.org/10.1016/0008-8749(74)90066-5
Prümmer O, Seyfarth C, Scherbaum WA, Drees N, Porzsolt F. Interferon-alpha antibodies in autoimmune diseases. J Interferon Res. 1989;9(Suppl.1):S67-74. https://doi.org/10.1089/jir.1989.9.S1-67
Ogushi F, Tani K, Endo T, Tada H, Kawano T, Asano T, et al. Autoantibodies to IL-1 alpha in sera from rapidly progressive idiopathic pulmonary fibrosis. J Med Invest. 2001;48:181-9. https://doi.org/10.2152/jmi.48.181
Puel A, Bastard P, Bustamante J, Casanova JL. Human autoantibodies underlying infectious diseases. J Exp Med. 2022;219:e20211387. https://doi.org/10.1084/jem.20211387
Tangye SG, Al-Herz W, Bousfiha A, Cunningham-Rundles C, Franco JL, Holland SM, et al. Human inborn errors of immunity: 2022 Update on the Classification from the International Union of Immunological Societies Expert Committee. J Clin Immunol. 2022;42:1473-507. https://doi.org/10.1007/s10875-022-01241-4
Hjelm-Skog AL, Wadhwa M, Hassan M, Gharizadeh B, Bird C, Ragnhammar P, et al. Alteration of interleukin 2 (IL-2) pharmacokinetics and function by IL-2 antibodies induced after treatment of colorectal carcinoma patients with a combination of monoclonal antibody 17-1A, granulocyte macrophage colony-stimulating factor, and IL-2. Clin Cancer Res. 2001;7:1163-70. https://doi.org/10.1097/00006534-200105000-00127
Bousfiha A, Jeddane L, Al-Herz W, Ailal F, Casanova JL, Chatila T, et al. The 2015 IUIS Phenotypic Classification for Primary Immunodeficiencies. J Clin Immunol. 2015;35:727-38. https://doi.org/10.1007/s10875-015-0201-1
Singh A, Jindal AK, Joshi V, Anjani G, Rawat A. An updated review on phenocopies of primary immunodeficiency diseases. Genes Dis. 2020;7:12-25. https://doi.org/10.1016/j.gendis.2019.08.004
Shamriz O, Tal Y, Talmon A, Nahum A. Chronic mucocutaneous candidiasis in early life: Insights into immune mechanisms and novel targeted therapies. Front Immunol. 2020;11:593289. https://doi.org/10.3389/fimmu.2020.593289
Ku CL, Chi CY, von Bernuth H, Doffinger R. Autoantibodies against cytokines: Phenocopies of primary immunodeficiencies? Hum Genet. 2020;139:783-94. https://doi.org/10.1007/s00439-020-02154-3
Salvaterra E, Campo I. Pulmonary alveolar proteinosis: From classification to therapy. Breathe (Sheff). 2020;16:200018. https://doi.org/10.1183/20734735.0018-2020
Carey B, Trapnell BC. The molecular basis of pulmonary alveolar proteinosis. Clin Immunol. 2010;135:223-35. https://doi.org/10.1016/j.clim.2010.01.006
Ataya A, Knight V, Carey BC, Lee E, Tarling EJ, Wang T. The role of GM-CSF autoantibodies in infection and autoimmune pulmonary alveolar proteinosis: A concise review. Front Immunol. 2021;12:752856. https://doi.org/10.3389/fimmu.2021.752856
Raziq FI, Abubaker A, Smith E, Uddin M. Secondary pulmonary alveolar proteinosis in GATA-2 deficiency (MonoMAC syndrome). BMJ Case Rep. 2020;13:e238290. https://doi.org/10.1136/bcr-2020-238290
Bodansky A, Vázquez SE, Chou J, Novak T, Al-Musa A, Young C, et al. NFKB2 haploinsufficiency identified via screening for IFN-α2 autoantibodies in children and adolescents hospitalized with SARS-CoV-2-related complications. J Allergy Clin Immunol. 2023;151:926-30.e2. https://doi.org/10.1016/j.jaci.2022.09.037
Fensterl V, Sen GC. Interferons and viral infections. Biofactors. 2009;35:14-20. https://doi.org/10.1002/biof.6
Le Page C, Génin P, Baines MG, Hiscott J. Interferon activation and innate immunity. Rev Immunogenet. 2000;2:374-86. https://doi.org/10.1159/000014079
Browne SK, Holland SM. Immunodeficiency secondary to anticytokine autoantibodies. Curr Opin Allergy Clin Immunol. 2010;10:534-41. https://doi.org/10.1097/ACI.0b013e328340ff72
Chen LF, Yang CD, Cheng XB. Anti-interferon autoantibodies in adult-onset immunodeficiency syndrome and severe COVID-19 infection. Front Immunol. 2021;12:788368. https://doi.org/10.3389/fimmu.2021.788368
Bloomfield M, Parackova Z, Cabelova T, Pospisilova I, Kabicek P, Houstkova H, et al. Anti-IL6 autoantibodies in an infant with CRP-less septic shock. Front Immunol. 2019;10:2629. https://doi.org/10.3389/fimmu.2019.02629
Puel A, Döffinger R, Natividad A, Chrabieh M, Bárcenas-Morales G, Picard C, et al. Autoantibodies against IL-17A, IL-17F, and IL-22 in patients with chronic mucocutaneous candidiasis and autoimmune polyendocrine syndrome type I. J Exp Med. 2010;207:291-7. https://doi.org/10.1084/jem.20091983
Pérol L, Lindner JM, Caudana P, Núñez NG, Baeyens A, Valle A, et al. Loss of immune tolerance to IL-2 in type 1 diabetes. Nat Commun. 2016;7:13027. https://doi.org/10.1038/ncomms13027
Arango-Franco CA, Migaud M, Ramírez-Sánchez IC, Arango-Bustamante K, Moncada-Vélez M, Rojas J, et al. Anti-GM-CSF neutralizing autoantibodies in Colombian patients with disseminated cryptococcosis. J Clin Immunol. 2023;43:921-32. https://doi.org/10.1007/s10875-023-01353-z
Browne SK, Burbelo PD, Chetchotisakd P, Suputtamongkol Y, Kiertiburanakul S, Shaw PA, et al. Adult-onset immunodeficiency in Thailand and Taiwan. N Engl J Med. 2012;367:725-34. https://doi.org/10.1056/NEJMoa1111160
Chen YH, Spencer S, Laurence A, Thaventhiran JE, Uhlig HH. Inborn errors of IL-6 family cytokine responses. Curr Opin Immunol. 2021;72:135-45. https://doi.org/10.1016/j.coi.2021.05.012
Jarrell JA, Baker MC, Perugino CA, Liu H, Bloom MS, Maehara T, et al. Neutralizing anti- IL-1 receptor antagonist autoantibodies induce inflammatory and fibrotic mediators in IgG4-related disease. J Allergy Clin Immunol. 2022;149:358-68. https://doi.org/10.1016/j.jaci.2021.06.018
Patton A, Mullenix MC, Swanson SJ, Koren E. An acid dissociation bridging ELISA for detection of antibodies directed against therapeutic proteins in the presence of antigen. J Immunol Methods. 2005;304:189-95. https://doi.org/10.1016/j.jim.2005.06.009
Pfeifer J, Thurner B, Kessel C, Fadle N, Kheiroddin P, Regitz E, et al. Autoantibodies against interleukin-1 receptor antagonist in multisystem inflammatory syndrome in children: A multicentre, retrospective, cohort study. Lancet Rheumatol. 2022;4:e329-37. https://doi.org/10.1016/S2665-9913(22)00073-9
Cheng A, Kashyap A, Salvator H, Rosen LB, Colby D, Ardeshir-Larijani F, et al. Anti-interleukin-23 autoantibodies in adult-onset immunodeficiency. N Engl J Med. 2024;390:1105-17. https://doi.org/10.1056/NEJMoa2303316
Griffin H, Cerón-Gutiérrez L, Gharahdaghi N, Ebrahimi S, Davies S, Loo PS, et al. Neutralizing autoantibodies against interleukin-10 in inflammatory bowel disease. N Engl J Med. 2024;391:434-41. https://doi.org/10.1056/NEJMoa2400013
Derechos de autor 2024 Biomédica

Esta obra está bajo una licencia internacional Creative Commons Atribución 4.0.
| Estadísticas de artículo | |
|---|---|
| Vistas de resúmenes | |
| Vistas de PDF | |
| Descargas de PDF | |
| Vistas de HTML | |
| Otras vistas | |

























